Type:
Educational Exhibit
Keywords:
Inflammation, Education and training, Education, Ultrasound-Colour Doppler, Ultrasound, Musculoskeletal system, Musculoskeletal soft tissue, Musculoskeletal joint
Authors:
U. Hasan1, T. Li1, D. Sadowsky1, T. Rashid1, J. Goldschmiedt1, H. Patel2; 1Valhalla, NY/US, 2Valhalla/US
DOI:
10.26044/ecr2019/C-1685
Findings and procedure details
Equipment
- Philips EQIP 7® Ultrasound Machine
- 12-5 MHz Linear Transducer
- Remaining standard departmental equipment seen in Figures 6 and 7.

Fig. 6: Standard departmental equipment used in most US-guided MSK injections
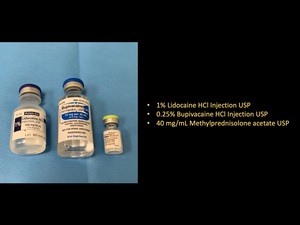
Fig. 7: Standard medications used in most US-guided MSK injections
Pre-Procedural Preparation
- The patient is brought into the ultrasound room,
and an adequate history is obtained.
- A focused physical exam is performed is performed with evaluation of active and passive range of motion.
- Dynamic sonographic evaluation of the rotator cuff is performed on each patient.
- Risks and benefits of the procedure are explained and informed consent is obtained.
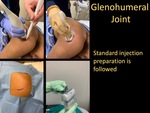
Standard Injection Preparation
- After identifying the region of interest,
the skin is marked.
- Sterile gloves are worn and the region is prepped with 3 sterile betadine swabs.
- A sterile drape is placed over the field.
- The 18-Gauge 1.5-inch needle is used to draw up the medication mixture into the 5cc syringe,
and 5-10cc of 1% Lidocaine HCl into the 10cc syringe.
- The sterile ultrasound gel is placed on the transducer,
followed by sterile transducer cover and more sterile ultrasound gel on top.
- The transducer is placed on the region of interest.
- A wheel of 1% Lidocaine HCl is placed in the subcutaneous tissues at the site of injection,
using a 25-Gauge 1.5-inch needle.
Procedural Steps
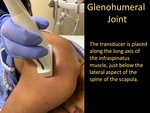
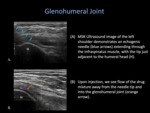
Glenohumeral Joint
- The patient is placed in a decubitus position with the unaffected arm-side on the table.
- With the ipsilateral arm adducted,
the transducer is placed along the long axis of the infraspinatus muscle,
just below the lateral aspect of the spine of the scapula,
until the humeral head and posterior glenoid is visualized in the same image.
- Doppler augmentation is utilized to avoid any major blood vessels.
- Standard injection preparation is followed.
- The medication mixture used for this injection contains: 80 mg Methylprednisolone,
3 cc of 1% Lidocaine and 3 cc of 0.25% Bupivacaine.
- Once numb,
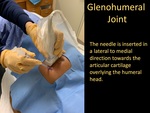
the 25-Gauge 1.5-inch needle is advanced through the subcutaneous wheel of lidocaine,
in a lateral to medial direction towards the articular cartilage overlying the humeral head.
- The needle tip is advanced until it contacts bone and then retracted slightly.
- A small amount of 1% Lidocaine is injected to ensure intra-articular placement.
- With the needle in place,
the 10cc syringe is disconnected and replaced with the 5cc syringe containing the medication mixture.
- The medication is slowly injected,
making sure to be cognizant of lack of resistance.
- The needle is withdrawn and pressure is held on the injection site to achieve hemostasis.
- The gel is cleaned up with gauze and a sterile bandage is placed.
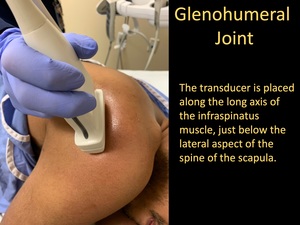
Fig. 8: Glenohumeral Joint Injection
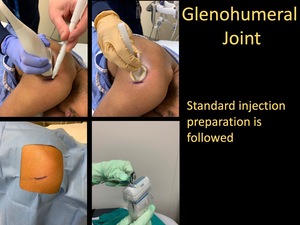
Fig. 9: Glenohumeral Joint Injection
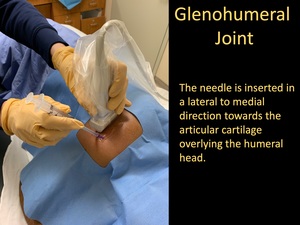
Fig. 10: Glenohumeral Joint Injection
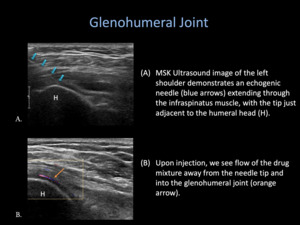
Fig. 11: Glenohumeral Joint Injection
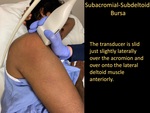
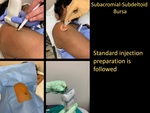
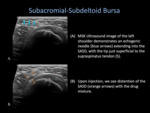
Subacromial-Subdeltoid Bursa
- The patient is placed in a decubitus position with the unaffected arm-side on the table.
- The transducer is placed along the long-axis of the acromion.
- The transducer is then slid just slightly laterally over the acromion and over onto the lateral deltoid muscle,
until the SASD is visible.
- Doppler augmentation is utilized to avoid any major blood vessels.
- Standard injection preparation is followed.
- The medication mixture used for this injection contains: 40 mg Methylprednisolone,
1 cc of 1% Lidocaine and 1 cc of 0.25% Bupivacaine.
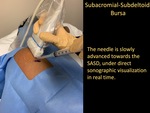
- Once numb,
the 25-Gauge 1.5-inch needle is slowly advanced towards the SASD bursa.
- Once it is felt that the needle tip is aligned with the narrow linear hypoechoic bursa,
a small amount of 1% Lidocaine is injected to ensure placement into bursa,
which will distend with resistance.
- With the needle in place,
the 10cc syringe is disconnected and replaced with the 5cc syringe containing the medication mixture.
- The medication is slowly injected,
making sure to be cognizant of lack of resistance and visualizing the bursal distention in real time.
- The needle is withdrawn and pressure is held on the injection site to achieve hemostasis.
- The gel is cleaned up with gauze and a sterile bandage is placed.
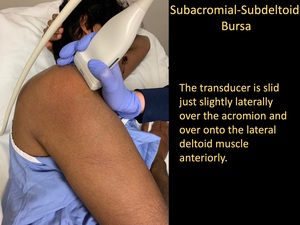
Fig. 12: Subacromial-subdeltoid Bursa Injection
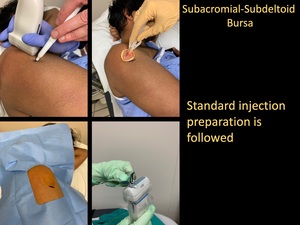
Fig. 13: Subacromial-subdeltoid Bursa Injection
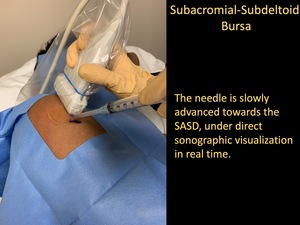
Fig. 14: Subacromial-subdeltoid Bursa Injection
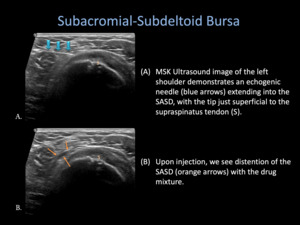
Fig. 15: Subacromial-Subdeltoid Bursa Injection
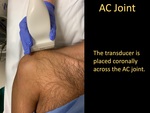
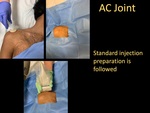
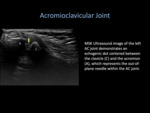
Acromioclavicular Joint
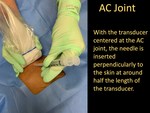
- We utilize the out-of-plane approach while performing injections into the acromioclavicular joint.
- The patient is placed in a supine position.
- The transducer is placed coronally across the AC joint.
- Attempts should be made to center the AC joint in the field of view.
- This way,
the needle will be inserted perpendicularly to the skin at around half the length of the transducer.
- Standard injection preparation is followed.
- The medication mixture used for this injection contains: 40 mg Methylprednisolone,
0.5 cc 1% Lidocaine and 0.5 cc 0.25% Bupivacaine.
- Once numb,
the 25-Gauge 1.5-inch needle is slowly advanced as the AC joint is fairly superficial.
- As the needle is out-of-plane to the transducer,
it will appear as an echogenic dot,
advancing towards the joint capsule.
- A small amount of Lidocaine is injected to ensure placement into the joint capsule,
which will distend with injection.
- With the needle in place,
the 10cc syringe is disconnected and replaced with the 5cc syringe containing the medication mixture.
- The medication is slowly injected,
making sure to be cognizant of lack of resistance and visualizing the capsular distention in real time.
- The needle is withdrawn and pressure is held on the injection site to achieve hemostasis.
- The gel is cleaned up with gauze and a sterile bandage is placed.
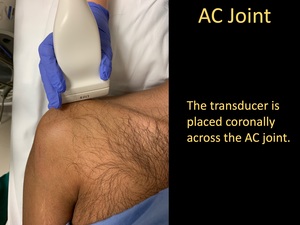
Fig. 16: AC Joint Injection
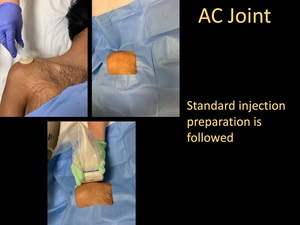
Fig. 17: AC Joint Injection
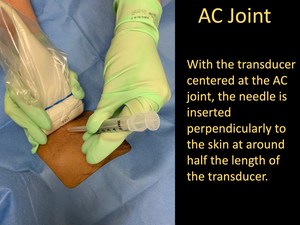
Fig. 18: AC Joint Injection
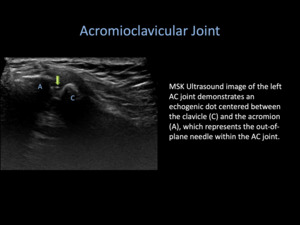
Fig. 19: Acromioclavicular Joint Injection
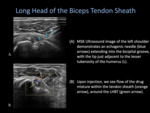
Biceps Tendon Sheath
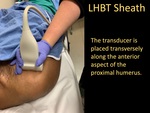
- The patient is placed in a supine position with the affected arm in a supinated configuration.
- The transducer is placed transversely along the anterior aspect of the proximal humerus.
- The long head of the biceps tendon (LHBT) is identified in the bicipital groove.
- Doppler augmentation is utilized to avoid any major blood vessels.
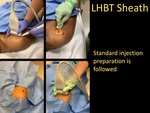
- Standard injection preparation is followed.
- The medication mixture used for this injection contains: 40 mg Methylprednisolone,
1 cc 1% Lidocaine and 1 cc 0.25% Bupivacaine.
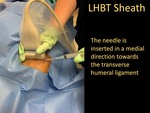
- Once numb,
the 25-Gauge 1.5-inch needle is advanced through the subcutaneous wheel of lidocaine,
directed towards the transverse humeral ligament.
- The needle tip should be followed deep to the LHBT,
where it should contact bone at the floor of the bicipital groove,
and then retracted slightly.
- A small amount of Lidocaine is injected to ensure placement into the LHBT sheath,
which will distend with injection.
- Injection directly into the tendon should be avoided,
as it may lead to rupture.
- With the needle in place,
the 10cc syringe is disconnected and replaced with the 5cc syringe containing the medication mixture.
- The medication is slowly injected,
making sure to be cognizant of lack of resistance,
and visualizing sheath distention in real time.
- The needle is withdrawn and pressure is held on the injection site to achieve hemostasis.
- The gel is cleaned up with gauze and a sterile bandage is placed.
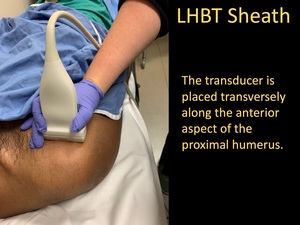
Fig. 20: LHBT Sheath Injection
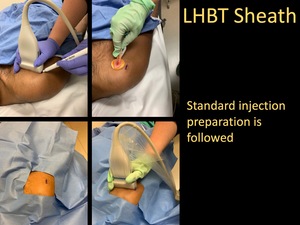
Fig. 21: LHBT Sheath Injection
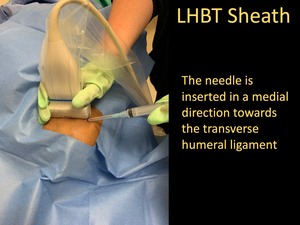
Fig. 22: LHBT Sheath Injection
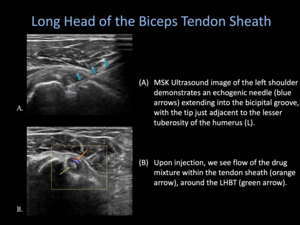
Fig. 23: LHBT Sheath Injection
Tips and Tricks
- We find that asking to play ambient music of the patient’s choice helps set a comfortable tone prior to starting the procedure.
- We utilize warm ultrasound jelly (Fig.
24).
- We are able to perform most US-guided injections around the shoulder joint using a 25-Gauge 1.5-inch needle.
Using a smaller gauge needle not only improves patient discomfort but also decreases their perception of expected pain.
- We perform most of our injections with the patient in a supine or contralateral decubitus position,
instead of a seated position,
which helps relax the patient.
- We use an aerosolized topical cold spray at the site of the injection,
to minimize discomfort from needle insertion.
- In the absence of the cold spray,
we use a few drops of 1% lidocaine on the skin,
at the site of the injection,
which act as a tactile warning so that the patient is able to brace themselves for the pinch of the needle insertion.
- We utilize single-needle technique for all of our injections around the shoulder.
This reduces patient discomfort and chances for post-procedural infections.
- In addition to visualizing the needle tip under US-guidance,
we use bony landmarks to provide tactile feedback which may assist in correct needle placement,
such as contacting the floor of the bicipital groove for LHBT sheath injections.
- We utilize the recently described "injection jet sign" [9] to confirm adequate needle placement,
and drug delivery.
- To minimize artifacts from air bubbles,
we prime the hub by dropping a few drops of the drug mixture.
before injecting the remainder.
- During most injections,
we give our patients stress balls which they can seem to appreciate.
- After the injections,
we give our patients reusable ice packs to use as needed,
to avoid post-procedural discomfort.

Fig. 25: Reusable Ice Pack