The study population of 75 cases consisted of 49,3% men (37/75) and 50,7% women (38/75).
The median age was 59 (range 18-96).
The majority of samples were obtained by CT-guided biopsy (47/75,
62.7%),
23 (30.7%) by intra-operative biopsy and five (6.7%) were acquired by bronchoscopy.
Etiology
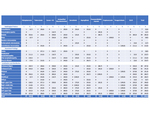
The table below summarizes the etiologies of GLD in our study population. Infection was the most common cause of GLD (47/75,
62.7%),
non-infectious causes occurred in 13.3% (10/75) and GLUS corresponded to 24% (18/75) of the cases.
Among infectious causes of GLD,
the great majority was fungal or mycobacterial,
led by Histoplasma capsulatum (27/75,
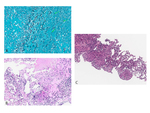
36%) (Fig.
2A) and Mycobacterium tuberculosis (7/75,
9.3%) (Fig.
2B).
Unclassified mycobacterial infection represented 6.7% of cases (5/75).
Other fungal infections included Paracoccidioidomycosis (3/75,
4.0%),
Aspergillosis (3/75,
4.0%) and Cryptococosis (1/75,
1.3%).
Only one case of parasitic infection occurred,
represented by Paragominiasis. Among non-infectious causes,
sarcoidosis occurred in 4 cases (5.4%) (Fig.
2C) and granulomatous inflammation associated with cancer occurred in 6 cases (8.0%).
Other non-infectious causes did not occur in our study population.
| Diagnosis |
Total cases (%) |
| Infectious |
47 (62.7) |
| Fungal |
34 |
| Histoplasmosis |
27 |
| Paracoccidioidomycosis |
3 |
| Aspergillosis |
3 |
| Cryptococcosis |
1 |
| Mycobacteriosis |
12 |
| Tuberculosis |
7 |
| Unclassified |
5 |
| Paragonimiasis |
1 |
| Non-infectious |
10 (13.3) |
| Sarcoidosis |
4 |
| Cancer associated with GI |
6 |
| GLUS |
18 (24) |
| Total |
75 (100) |
(%) = Percentage of total number of cases
GI = Granulomatous Inflammation
GLUS = Granulomatous Lesions of Unknown Significance
Table – Etiology of Granulomatous Lung Diseases
Chest CT Findings
The main radiological pattern,
location and distribution,
as well as associated imaging findings are summarized in Table 1.
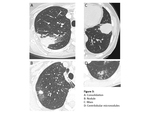
The nodular pattern was the commonest CT finding overall (49/75,
65.3%),
the second was centrilobular micronodules (9/75,
12%),
followed by consolidation (7/75,
9.3%) and mass (6/75,
8.9%) (Fig.
3).
The majority of cases had unilateral pulmonary findings (59/75,
78.7%),
more commonly in the right side (31/75,
41.3%).
Two-thirds of the cases showed a focal lesion on chest CT (50/75); multifocal (20/75,
26.7%) and diffuse (5/75,
6.7%) distribution of lesions were less common.
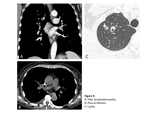
Among associated findings,
hilar or mediastinal lymphadenopathy occurred respectively in 16% (12/75) and 10.7% (8/75) of the cases; pleural effusion (8/75) and cavitation (8/75) also occurred in 10.7% of cases (Fig.
4).
Nodular pattern was the most common imaging feature in Histoplasmosis cases (25/27,
92.6%),
whereas it occurred in half of cases (24/48) of GLD of other causes (p<0.05).
None of the cases of Histoplasmosis presented micronodules or ground glass opacities as the main patterns.
Cavitation also was not present in any case.
Regarding distribution of the lung lesions,
all cases except one (26/27,
96.3%) were focal in Histoplasmosis,
while in other causes of GLD focal distribution occurred in 50% (24/48) of cases (p<0.05) (Table 2).
Among patients with tuberculosis,
the second etiology of GLD in our study population,
the most common imaging pattern was centrilobular micronodules (3/7,
42.9%),
significantly more frequent than in other causes of GLD (6/68,
8.8%).
Cavitation also was highly suggestive of mycobacterial infection,
occuring in 57.1% (4/7) of cases of tuberculosis,
compared to only 2 cases (2.9%) of all other causes of GLD,
considering that one of these 2 cases occurred in a patient with unclassified mycobacteriosis (Tables 3 and 4).
All 4 cases of sarcoidosis had multifocal distribution and patterns varied between consolidation,
nodular and perilymphatic micronodules.
Mediastinal or hilar lymphadenopathy occurred in majority of cases.