Type:
Educational Exhibit
Keywords:
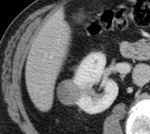
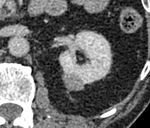
Cancer, Ablation procedures, CT, Oncology, Kidney, Interventional non-vascular
Authors:
M. F. S. Shaukat, S. Sultana , M. Djearaman, S. Hussain; BIRMINGHAM/UK
DOI:
10.26044/ecr2019/C-1859
Background
The incidence of renal cell carcinoma (RCC) has been gradually increasing.
However,
there have been improvements in treatment options also [1].
Most renal cancers are now detected at early-stage being suitable for nephron-sparing ablative procedures,
such as radiofrequency ablation (RFA),
cryoablation,
micro-wave ablation (MWA).
Compared to minimally invasive surgery for RCC,
percutaneous ablation is less invasive with fewer complications and faster convalescence [2].
Percutaneous ablation procedures may be repeated when not completely successful in single session or performed repeatedly in patients with syndromic renal cancers who unfortunately develop multiple tumors through-out their life-time.
Also,
percutaneous ablation is the only local treatment option in patients that are unable to undergo surgery.
Cost to the health care system potentially can be reduced with increased use of percutaneous ablative techniques as compared to nephron sparing surgery.
(3,4)
The most important disadvantage of any percutaneous ablation procedure is a higher local tumor recurrence rate relative to partial nephrectomy.
(5) However,
there is paucity of long-term disease-free survival data on percutaneous ablation of small RCCs.