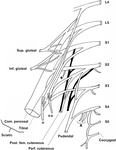
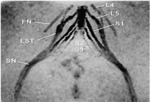
Normal anatomy of the lumbosacral plexus:
The lumbar and sacral plexuses are formed by the ventral rami of L1–L4 and the ventral rami of L4–S3.
Together,
via the lumbosacral trunk,
they form the lumbosacral plexus,
which innervates the lower extremity.
The lumbar plexus is formed in the psoas muscle.
It gives rise to nerves which exit either lateral (iliohypogastric,
ilioinguinal,
genitofemoral,
femoral,
and lateral femoral cutaneous nerve) or medial (obturator nerve and lumbosacral trunk) to the psoas muscle.
The sacral plexus is formed anterior to the piriformis muscle and gives the sciatic nerve,
the superior and inferior gluteal nerves,
and the pudendal and posterior femoral cutaneous nerves.
The lumbosacral trunk,
which is made up of L5 and a small branch of L4, connects the lumbar and sacral plexuses; it is for this reason that the term lumbosacral plexus is used to refer to the combined neural complex(Fig.
4 and 5).
Imaging technique includes:
- Conventional Neurography
- 2D T1,
T2 and fat suppresion sequences in three orthogonal planes obtained in thin cuts.
- 3D isotropic T1.
- Post contrast T1 fat suppression in three orthogonal planes.
Appearance of the normal nerves at MRN:
1-Similar in size to adjacent artery and gradually decreases distally.
2- T1-W: Isointense to skeletal muscle,
STIR/fat saturation and T2-W: Iso to minimally hyperintense,
3D SPACE: on 3D SPACE (sampling perfection with application optimized contrasts using varying flip angle evolutions) uniform symmetric hyperintensity.
3-Preserved fascicular pattern at T1-W and T2-W.
4-Smooth continuous course without focal deviation with clear perineural fat planes.
5-No enhancement except in area of deficient blood nerve barrier as the dorsal root ganglion (Fig.
6).
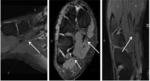
Findings:
a-Size: Focal or diffuse enlargement i.e.: larger than the adjacent artery.
b--Fascicular pattern: Single or multiple fascicles enlargement,
disruption or loss of fascicular pattern.
c.
Signal intensity: asymmetric hyperintensity on 3D SPACE orT2 hyper intensity (becoming similar to adjacent veins).
d- Continuity and course: focal / diffuse deviation or discontinuity.
Mild nonspecific T2 hyper intensity of the nerves can be seen in asymptomatic subjects due to magic angle artifact,
mild or subclinical neuropathy .Increased nerve signal intensity is particularly commonly seen on STIR images due to high fluid sensitivity as well as good fat suppression.
T1-W MR images are useful in differentiating nerve from the adjacent vessels (arteries usually seen as flow voids while veins usually seen as T1 hyper intense due to inflow phenomenon).
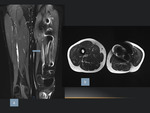
STIR images in sagittal plane are very useful to detect individual segmental plexus.
Since the plexus is usually hyperintense on STIR images.
Alterations of signal,
size and course of the abnormal plexus segments compared with the ipsilateral normal appearing segments or the contralateral normal plexus should be carefully looked for (Table 2),(Fig.
7 and 8).
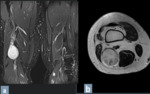
- Muscle changes in response to nerve affection:
MR can demonstrate regional muscle denervation changes in addition to the direct signs of nerve abnormality.
These muscle findings evolve from edema like signal on fat suppressed T2W MR images in acute stages to fatty replacement and atrophy with chronicity (Table 3).
2. Functional Neurography
Peripheral nerves are highly anisotropic structures with a marked diffusion restriction in its perpendicular plane and facilitated diffusion along the main axis of the nerve ( ie parallel to the nerve fibers ).
These physiological features allow the application of classical diffusion weighted sequences.
DW-MRN improves the neural visualization by maximizing the contrast between the nerves and the signal from suppressed background tissues.
This enables MIP evaluation of the nerve plexus to be performed,
allowing the nerves to be appraised over longer trajectories and to well stand out in comparison to the back ground improving assessment of any nerve pathology and well characterizationof the degree of affection of various portions of the nerve (Fig.
9).
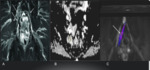
DTI are valuable and reliable methods for the noninvasive evaluation of peripheral nerve tumors.
DTI allows interrogation of the microarchitecture of the nerves,
which is beyond the resolution of anatomic imaging techniques.This technique has proven clinical utility in a number of brain and spinal cord studies.
However,
early feasibility data from peripheral nerve are becoming available in the last few years(Fig.
10).
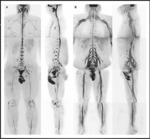
3.Whole body MRN :
•Whole body MR imaging has been around for many years for the evaluation of metastatic disease,
myeloma,
and lymphoma.
Takahara et al.
described a free breathing DW whole body MR imaging technique with background body signal suppression and an STIR prepulse for robust fat suppression,
which enables a longer effective imaging time than that with breath-hold imaging and allows acquisition of a large number of thin sections and three-dimensional analyses(Fig.
11).