Keywords:
Neuroradiology brain, MR-Functional imaging, Diagnostic procedure, Seizure disorders
Authors:
V. Sawlani, K. Kawsar, D. McCorry, A. Hawkins, J. Herbert, R. Chelvarajah; Birmingham/UK
DOI:
10.26044/ecr2019/C-1993
Results
Results
9/26 refractory epilepsy patients were operated by anterior temporal lobectomy (RATL =7 and LATL =2).
7/26 patients underwent insertion of Vagal nerve stimulator
None of the operated patient were found to have any memory deficit on clinical follow up.
Six out of nine patients had detailed neuropsychiatric assessment at one year follow up,
while three are waiting to be done soon.
In these six patients,
whom post-surgical psychometric test were performed; comparison with pre-surgical baseline assessment showed no decline in any domain of cognition re-assessment,
including intellectual functioning,
memory,
processing speed,
executive functioning or naming ability.
Two patient showed improved visual memory index from preoperative status.
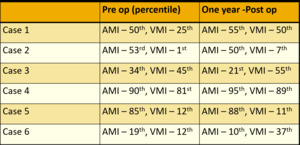
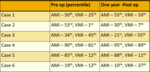
Fig. 4: Pre and post operative Auditory and Visual Memory Index
Case 1
- 22 year old,
right-handed landscape gardener
- Onset of seizure at 16 years.
Complex partial seizure of “tapping the pen on the table”,
staring and then collapse followed by a secondary generalization.
- Scalp VT: A single event was captured that showed orofacial automatisms
- EEG: high amplitude right temporal and zygomatic activity with right hemisphere post-ictal slowing
- Inter-ictal recordings were also concordant.
Right temporal complexes and slow wave activity.
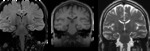
- MRI: unequivocal appearance of right side hippocampal sclerosis
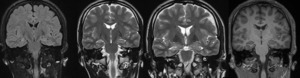
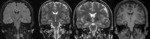
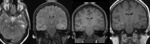
Fig. 5: Case 1. Coronal FLAIR, T2W and T1W MRI shows unequivocal appearances of right hippocampal sclerosis.
- Pre-operative Neuropsychological Assessment: showed average intellectual functioning in 50th centile with no lateralizing memory deficit

Fig. 6: Case 1. Pre-operative neuropsychological assessment showed average intellectual functioning in 50th centile with no lateralizing memory deficit
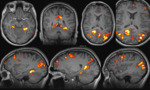
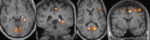
- Memory fMRI Hometown walking paradigm performed which showed bilateral activation of the para-hippocampal gyri (left>right).
- There was concordance in localization of seizures electrographically,
radiographically,
and semiologically in right hippocampus - Good surgical candidate
- The patient had image-guided right temporal lobe surgical resection for epilepsy and histology demonstrated right hippocampal sclerosis.
- He had a near total seizure free outcome and no suggestion of decline in cognitive function compared to the pre-surgical status.
- Visual memory index improved from 45th percentile to 55th percentile.
Case 2
- 26 year old right-handed female
- Onset of Seizures at age 15
- High seizure burden,
average five per month; significant perimenstrual clustering of up to 15 seizures on a day
- Semiology:- Deja vu on occasions and clammy hands leading to clouding of awareness.
Witnessed bilateral hand “clawing,” drooling,
teeth clenching,
and aimless walking.
Grunts during seizures without any discernible words
- Scalp VT captured one event which was stereotypic to the above habitual seizure description and in addition demonstrating a right hand dystonic posturing.
Evolution of sharp and slow activity from left temporal region.
- MRI showed low grade glioma in middle/inferior temporal gyrus.
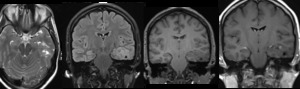
Fig. 8: Case 2. Low grade glioma in the left medial temporal lobe involving the hippocampal structures (arrowed).
- There was no reliable discrepancy between visual and verbal memory,
both were in the low average range.
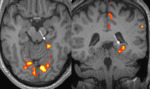
- The patient’s memory fMRI scan is demonstrated bilateral activation in para-hippocampal gyri.
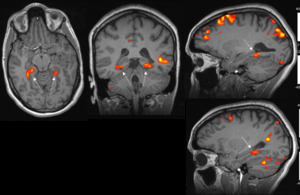
Fig. 9: Case 2. Memory fMRI – Imaginary Walk Paradigm shows almost symmetrical activation in bilateral para-hippocampal gyri (arrowed).
- The patient had had image,
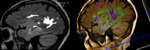
DTI and ECoG-guided left temporal lobe resection for tumour-based epilepsy and histology demonstrated WHO grade I pilocytic astrocytoma.
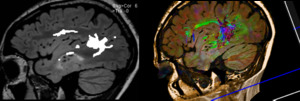
Fig. 10: Case 2. ECOG guided surgery with DTI (Arcuate fasciculus)- Lesionectomy and radical Hippocampectomy performed.
- She has been seizure free for the last six months with no cognitive decline on clinical assessment.
Case 3
- 39 year female having febrile convulsions since age of 19
- Complex partial seizure- one per fortnight,
Aura’s and ‘absence’ several per week
- Feeling of fear with deja-vu follow with staring and stiffness.
Some period of post-ictal speech loss
- Teacher by profession.
Speaks 4 languages. Reports memory problems- deteriorated over last 5 years
- Treatment - On Levetiracetam and Lamotrigine
- MRI revealed left sided hippocampal sclerosis.
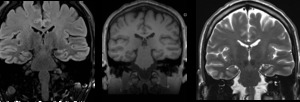
Fig. 11: Case 3. MRI shows left-sided hippocampal sclerosis.
- Pre-operative neuropsychological assessment showed GAI 125 (superior range),
including VCI.
Executive functions all in superior range BNT 60/60 and AMI 95,
VMI 100.
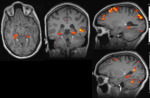
- The Home Town Walking memory fMRI from Day 1 and 2 showed reproducible activation in the dominant hemisphere.
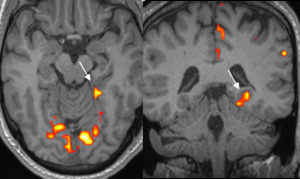
Fig. 12: Case 3. Day 1 imaginary Walk Paradigm shows activation only in left para-hippocampal gyrus (arrowed).
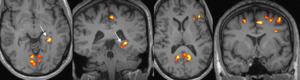
Fig. 13: Case 3. Day 2 fMRI examination shows similar activation in left para-hippocampal gyrus (arrowed), anterior language areas, dorsolateral prefrontal cortex, and secondary visual cortex.
- In this case there was concordance in localization of seizures electrographically,
radiographically,
and semiologically to the left hippocampus in a patient with adult onset epilepsy.
- There is potentially high risk of memory deficit and the patient has been put on a vagal nerve stimulator (VNS).