Out of 38 patients,
12 (31,6%) were diagnosed with PAS and 26 (68,4%) did not show PAS.
When considering the clinical outcome,
8 patients (21,1%) showed poor outcome and 30 good outcome (Figs.
3,4).
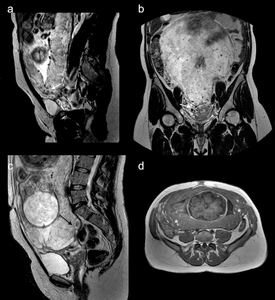
Fig. 3: Figure 3. A case of good outcome in a 33-year old pregnant with invasive placenta. Sagittal (a, c), and coronal (b) T2-weighted images and axial T1-weighted image (d) showing abnormal flow voids (white arrow in a and b), uterine bulging (black arrow in c) and heterogeneous signal intensity due to focal hemorrhage (white asterisks in d). The patient had minor bleeding and underwent conservative treatment (bakri balloon and b-lynch suture). Invasive placenta with accretism was demonstrated at the delivery.
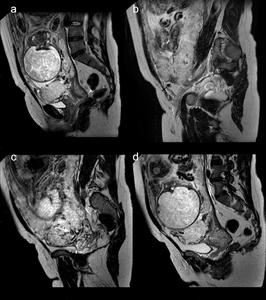
Fig. 4: Figure 4. A case of poor outcome in a 36-year old pregnant with invasive placenta. Sagittal (a, b, c, d) T2-weighted images showing intraplacental dark bands (white asterisks in a), placental recess (black arrow in b), intraplacental abnormal vascularity (white arrow in c), myometrial thinning with focal indistinctness of its delineation (black asterisk in c) and signs of percretism with bladder invasion (white P” in d). The patient underwent emergency hysterectomy and PAS with percretism was histologically confirmed.
The Discriminant Analysis provided two specific predictive models,
one for the PAS diagnosis and one for the clinical outcome prediction.
Percretism signs were found to be the most important predictive variable,
both considering the PAS and the clinical outcome prediction.
In detail,
the predictive model selected two MR signs for the predictive function of PAS: intraplacental abnormal vascularity and percretism signs.
The area under the curve (AUC) of the predictive model for PAS was 0.833 with a cut-off of 0.39 (67% sensitivity and 100% specificity,
p=0.001).
When considering the predictive function of clinical outcome,
myometrial thinning and percretism signs were selected.
AUC of the predictive model for clinical outcome was 0.971 with a cut-off of 0.55 (100% sensitivity and 77% specificity,
p<0.001).
(Fig.5)
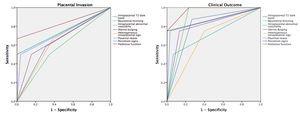
Fig. 5: Figure 5. ROC curve analysis of MR findings and predictive functions for PAS and clinical outcome.
Interestingly,
the predictive power increased in term of sensitivity (from 67 to 100%) if the subject moved from the PAS to the clinical outcome.
These results may have a beneficial effect from a clinical point of view because they focus the attention on the “critical” patients.