Study population
The Institutional Review Board approved this retrospective study and waived the requirement of informed written consent.
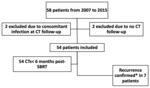
We searched our database for consecutive patients who underwent SBRT due to lung cancer stages I or II[15] or pulmonary metastasis at our institution from 2007 to 2015.
Patients were excluded if they had only a single CT performed during the follow-up or confirmed pulmonary infection during follow-up CT (by clinical suspicion,
radiological changes and treatment).
Patients selection is demonstrated on Figure 1. Clinical,
radiological and SBRT data were obtained from our digital medical records.
Stereotactic Body Radiation Therapy
For administration of SBRT,
a semi-rigid device for positioning and immobilization of the patients was developed and a commercial device was used.
The immobilization device was indexed to the patient's body and treatment bed.
We performed internal organ and tumor movement analysis with 4DCT or three consecutive CT sequences: 1) normal breathing CT; 2) forced inspiration CT and 3) forced expiration and / or CT with slow acquisition of images.
Using this approach,
we defined the internal target volume (ITV) that consider a personalized movement assessment.
A standard margin of 0.5 cm–1.0 cm was added to the ITV to create planning target volume [3].
SBRT was performed using linear accelerator and based on image guidance.Pre-treatment positioning of the tumor and patient was evaluated with cone beam CT images.
Tumor and patient related displacements were corrected immediately before each SBRT fractions using CBCT technique[16].
Chest CT protocol
CT scans were performed by two different devices: a dual-source 256 row detector and a 64-row detector.The acquisition parameters were the same for both devices,
as follows: 170–220mAs; 120kVp; tube rotation time,
0.5s; pitch,
0.12; field of view 400–500mm.
When contrast was required,
the timing was determined with a test bolus consisting of 10–15ml of iohexol solution with an iodine concentration of 300 mg ml-1 injected at a flow rate of 4.0–5.5 ml /s-1.
Contrast imaging was performed with 1,0-1,5 ml/kg injected at the same flow rate.
Images were reconstructed in axial view using a slice thickness of 1mm and an increment of 0.7mm.
Image analysis
Three board-certified radiologists with 1,
4 and 10 years of experience after the end of thoracic radiology fellowship training reviewed the CT examinations.
The readers were blinded for clinical data of the patients,
including the presence of recurrence.
The radiologists reviewed the CT scans at two different time points: (a) early follow-up (0-6 months post-SBRT) and (b) late follow-up (> 6 months post-SBRT).
Readers also classified the CT findings as expected changes after SBRT or recurrence.
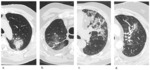
Imaging features expected on early period were defined as: (a) diffuse consolidation; (b) patchy consolidation; (c) diffuse ground glass opacity (GGO); (d) patchy GGO; (e) absence of new opacities[10,
14].
Table 1 summarizes the scoring system for acute changes after SBRT and Figure 2 displays them on CT.
On late follow-up,
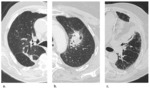
expected imaging features were divided into: (a) modified conventional pattern; (b) scar-like fibrosis; (c) mass-like fibrosis; and (d) no abnormalities. Table 2 summarizes the scoring system for late changes after SBRT and Figure 3 displays them on CT.
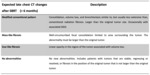
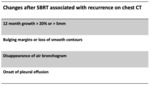
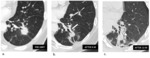
Recurrence findings on chest CT were defined as presence of (a) enlarging opacity (12-month growth > 20% or 5 mm); (b) bulging margins or loss of smooth contour; (c) loss of an air bronchogram; or (d) onset of pleural effusion. Table 3 summarizes changes after SBRT associated with recurrence[11] and Figure 4 displays a case of recurrence.
Statistical analysis
Continuous variables were tested for normality with the Kolmogorov-Smimov and Shapiro Wilk tests.
The values are expressed as median and percentiles 25 and 75 or as the mean and standard deviation for parametric and non-parametric data respectively.
The categorical data are presented as absolute values and percentages and were tested using Pearson χ2 test and Fisher exact test,
if applicable.
The Mc’Nemar test was used by compare two methods.
Interobserver agreement was assessed by Wilcoxon and Kappa statistics. Kappa values were interpreted qualitatively.
Kappa value of 0.81–1.00 was considered strong agreement[17].
Statistical significance was considered with p≤0,05.