Recommended MRI Imaging Protocols
Static and dynamic sequences should be acquired; T2-weighted images (T2WI) are recommended for both,
due to its greater anatomic detail.
( Fig. 1 ).
[3]
T1WI should complement the examination,
whenever a pelvic lesion is detected.
- Static images → Detection and classification of structural abnormalities
→ Pelvic floor anatomy
→ Defects of the supporting structures
→ Anal sphincter complex
- Dynamic images (during squeezing,
straining and defecation) → functional abnormalities that are assessed by metric measurements of the three compartments
→ Pelvic organ mobility
→ Pelvic floor relaxation
→ Pelvic organ prolapse (POP)
→ Associated compartment defects
No oral or intravenous contrast is necessary.
[3]
Anatomy brief review
◊ Pelvic compartments
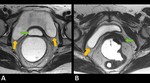
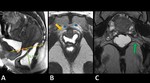
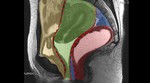
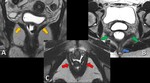
Pelvic floor is one functional unity commonly divided into three different compartments ( Fig. 2 ):
- Anterior Compartment (AC) - Bladder and Urethra
- Cystocele
- Urethral Hypermobility
- Middle Compartment (MC) - Uterus,
Cervix and Vagina
- Uterine/Vaginal prolapse
- Posterior Compartment (PC) - Anus,
Anal Canal,
Rectum,
Sigmoid colon
- Pelvic Floor Relaxation
- Rectocele
- Intussusception
The cul-de-sac is often considered a "virtual" compartment,
where pathological processes also occur:
- Enterocele
- Peritoneocele
- Sigmoidocele
◊ Supporting Structures
Endopelvic Fascia - located immediately beneath the peritoneum; it has various thickenings or condensations in specific areas.
[5]
⇒ Most of Endopelvic Fascia ( Fig. 3 ) is not directly visualized in MRI → Defects are inferred based on secondary signs! [6]
° Level I (suspension) - Cephalic 2–3 cm of the vagina and above
- Provides the upper vaginal support (Parametrium and Paracolpium) [6,7]
° Level II (attachment) - Mid-portion of the vagina (between level I and III)
- Transverse support of the vagina (Paracolpium)
- Urinary bladder support (through the anterior vaginal wall)
- Prevents the anterior protrusion of the rectal wall (through the posterior vaginal wall and rectovaginal fascia)
- Prevents the bowel from herniating inferiorly (rectovaginal fascia) [4]
° Level III - At the level of the hymen ring and the 2–3 cm above it → directly attached to the surrounding structures (urethra,
perineal body, levator ani muscles)
- Urethral support [4,5,7]
⇓
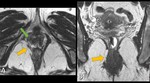
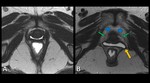
Static images in normal patients show ( Fig. 4 ):
- Symmetrical urethral ligaments on an axial scan (no distortion or defect)
- Bladder neck positioned close to the pubis symphysis
- Vaginal lumen with a widened H-appearance in axial sequences and the lateral vaginal walls are close to the puborectalis muscle [3,4]
Pelvic Diaphragm - The levator ani (pubococcygeus,
puborectalis and iliococcygeus muscles) and ischiococcygeus muscles.
[4,5,7] ( Fig. 5 )
- Iliococcygeus forms,
posteriorly,
a firm midline raphe ⇒ Levator plate
- Puborectalis ⇒ U-shaped sling - elevates the bladder neck and compress it against the pubic symphysis [4,5,7]
Urogenital Diaphragm - Connective tissue and the deep transverse muscle of the perineum (anterior to the anorectum) [4,8]
Pelvic organ prolapse vs pelvic floor relaxation
Different entities,
but frequently coexistent in pelvic floor weakness
Pelvic organ prolapse - abnormal descent of a pelvic organ through the hiatus beneath it [3]:
- bladder (cystocele)
- vagina (vaginal prolapse)
- uterus (uterine prolapse)
- mesenteric fat (peritoneocele)
- small intestine (enterocele)
- sigmoid colon (sigmoidocele)
Pelvic floor relaxation - excessive descent and widening of the entire pelvic
floor during rest and/or evacuation,
regardless of whether prolapse is present.
[3]
How to look at the MRI?
◊ Dynamic Images - Identifying and grading the abnormality(ies)
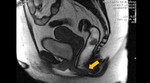
1 - Maximum straining - Is there:
- Loss of urine through the urethra?
- Urethral hypermobility? ( Fig. 6 )
- Kinking of the urethrovesical junction?
- An enterocele? Which is the content of the peritoneal sac?
- Loss of rectal gel during straining? ( Fig. 7 )
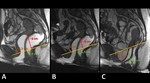
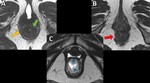
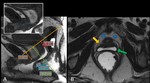
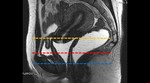
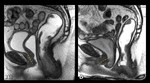
2 - Rest,
squeezing and defectation - Trace the Anorectal Angle (ARA) ( Fig. 8 ) - expresses the functioning of the Puborectal muscle
- At rest – 93º
- During squeezing - sharpening of 10-15°
- During straining or defecation - 15-25° more obtuse [3]
ARA should close with squeezing and open with defecation ⇒ The change of ARA with dynamic sequences is more important than the absolute values.
[3]
3 - Rest,
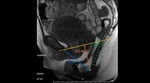
maximum straining and defecation - Trace the pubococcygeal line (PCL) ( Fig. 9 )
3.1 - Measure the perpendicular distance between the PCL and each reference point (values above the reference line have a minus sign,
values below a plus sign): [3,4,6]
- Anterior compartment → the most inferior aspect of the bladder base
- Middle compartment → the most distal edge of the cervix or the vaginal vault in case of previous hysterectomy
- Posterior compartment → the anorectal junction
⇒ Cystocele and POP are graded accordingly to the “rule-of-three", starting at 1 cm below the PCL [3]:
- Grade I - 1–3 cm
- Grade II - 3–6 cm
- Grade III - > 6 cm
Refer cystocele and POP as pathological just when grade II or III.
[3]
⇒ Anorectal Junction descent (ARJ) is graded starting at 3 cm below the PCL [3]:
- Grade I - 3 - 5 cm below the PCL
- Grade II - > 5 cm below the PCL
〉 The difference between rest and maximum straining should be noted - Pelvic Organ Mobility.
〉 The full extent of POP is only visible during evacuation! [3]
4 - End of evacuation phase
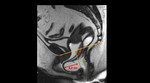
4.1 -Is there a rectocele? (Measure the distance between the anterior rectal wall and a vertical line that goes through the anterior wall of the anal canal) ( Fig. 10 )
⇒ Grade rectoceles using the “rule-of-two” - pathological starting from II [3]
- Grade I - < 2 cm
- Grade II - 2–4 cm
- Grade III - > 4 cm
4.2 - Is there any mucosal invagination/rectal prolapse? ( Fig. 11 )
4.3 -Was rectal emptying adequate? Was it delayed?
→ In the presence of incomplete evacuation or delayed evacuation time (more than 30 seconds to evacuate 2/3 of the rectal content),
anismus should be considered.
[3,6]
___________________________________________________________
Δ Routinely measuring pelvic floor relaxation reached no consensus! [2]
- H-line (hiatus length)
- M-line (descent of the levator plate)
- Levator plate angle
⇓
Measured in the sagittal plane ( Fig. 12 )
Normal values [6]:
- H-line during straining 5.8 ± 0.5 cm
- M-line during straining 1.3 ± 0.5 cm
- Levator plate angle during straining 11.7 ± 4.8° [9]
- Transverse width of the levator hiatus (axial plane)
- Iliococcygeus angle (coronal plane)
⇓
Measured in the axial and coronal planes - Optional sequences [3]
___________________________________________________________
◊ Static Images - Finding the underlying structural defect responsible for the previously identified abnormalities.
- Urethral support system - maintains urinary continence
- Level III endopelvic fascial defects
→ Widening of the retropubic space - Moustache sign ( Fig. 4, Fig. 18, Fig. 19 ) [3,4,7]
- Puborectalis muscle detachment,
disruption,
atrophy or avulsion ( Fig. 13 ) [3,4,7]
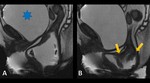
- Vaginal support system - prevents prolapse
- Level I and II paravaginal fascial defects
→ Loss of the H-shape of the vagina
→ Sagging of the posterior bladder wall → "Saddlebag" sign ( Fig. 14 ) [3,4,7]
- Iliococcygeus diffuse or focal muscle abnormality
- Anal sphincter complex - maintains anal continence [3,4,6]
- Mucosa/Submucosa
- Internal anal sphincter
- External anal sphincter



![Fig. 8: Midsagittal T2-weighted MR images obtained during squeezing (A.), at rest (B.) and during defecation (C.) demonstrating the Anorectal Angle (ARA) measurement. Although the ARA at rest is higher than the recommended normal value [2], there is a normal sharpening during squeezing and a normal widening during defecation.](https://epos.myesr.org/posterimage/esr/ecr2019/149283/media/793981?maxheight=150&maxwidth=150)