The embryonic origins of the spleen are obscure,
with most studies describing its origin from mesenchymal cells between the layers of the dorsal mesogastrium,
adjacent to the splanchnic mesodermal plate.
Mesenchymal cells differentiate to form the splenic capsule,
connective tissue and its parenchyma.
The spleen is an organ of the haematologic system and has a role in immune response,
storage of red blood cells and hematopoiesis.
NORMAL SPLEEN
The spleen is wedge-shaped and located in the left upper quadrant protected by the left 9th to 11th ribs.
It is enclosed by a thin capsule,
which is easily ruptured.
Size varies from person-to-person but the average is 2.5cm thick,
7.5cm broad and 12.5cm in length in the adult population.
Splenic artery is responsible for the arterial supply and the splenic vein for the venous drainage.
Splenic hilar lymph nodes drain to retropancreatic lymph nodes,
then to celiac lymph nodes.
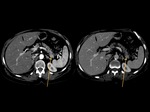
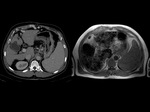
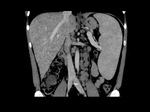
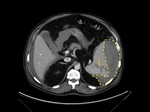
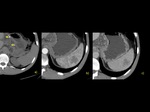
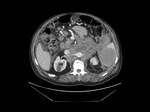
Splenic enhancement on arterial phase is typically heterogeneous,
called zebra or psychedelic spleen,
therefore splenic parenchyma should be assessed in portal venous phase.Fig. 1
1.
CONGENITAL ANOMALIES
1.1.
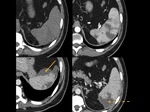
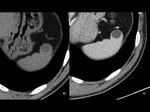
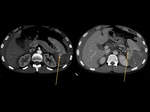
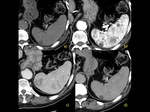
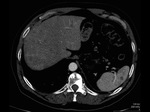
Accessory spleen – 10% of population.Fig. 2
1.2.
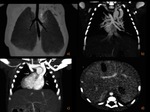
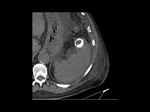
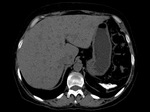
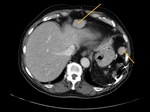
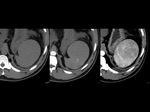
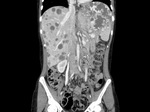
Asplenia – Association with heterotaxy,
isomerism,
congenital heart disease and total anomalous pulmonary venous return.Fig. 3
1.3.
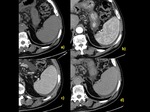
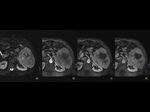
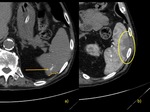
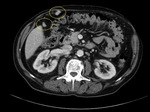
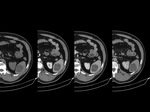
Polysplenia - also known as left isomerism,
is a type of heterotaxy syndrome where there are multiple spleens.
Association with congenital heart disease (>50%),
gastro-intestinal malformations,
including midgut malrotation (80%),
biliary atresia,
tracheo-esophageal fistula; genito-urinary malformations,
inferior vena cava and portal vein anomalies.Fig. 4
1.4.
Retrorenal spleen
1.5.
Splenogonadal fusion
1.6.
Wandering spleen - Rare condition in which the spleen migrates from its usual anatomical position to the lower abdomen or pelvis.
2.
PORTAL HYPERTENSION
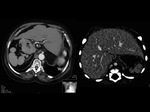
- Splenomegaly
- Most commonly homogeneous or with some infartion zones.
Rarely there may be seen siderotic nodules,
also known as Gamna-Gandy bodies,
of the spleen,
are most commonly encountered in portal hypertension.
The pathophysiological process is the result of microhemorrhage resulting in hemosiderin and calcium deposition followed by fibroblastic reaction.Fig. 5
- Dilated portal vein +/- mesenteric veins
- Paraumbilical vein repermeabilization: pathognomonic
- Collateral varices
- Ascites
- Cause of portal hypertension often identified (most common: cirrhosis and portal vein thrombosis)
3.
INFLAMATORY DISEASES
3.1.
Bacterial Abscess
A splenic abscess is a localized collection of pus that is generally caused by the haematogenous or local spread of infection (75% of cases).
Other causes include penetrating trauma (15%) and prior splenic infarction (10%).
Pyogenic abscesses can be single or multiple.
On CT,
bacterial abscesses are frequently visualized as a low-attenuation center of fluid or necrotic tissue.
Minimal peripheral contrast enhancement may be present.
The presence of gas in an intra-splenic collection is diagnostic for an abscess,
although the majority of splenic abscesses do not contain air.
3.2.
Fungal abscess
Multiple small,
low-attenuation areas that are usually well demarcated and that range from a few millimeters to 2 cm in size are shown at CT.
Rim enhancement is not typically seen.
3.3.
Malaria
Although rare in the occidental countries,
malaria is still the primary cause of spontaneous splenic rupture around the world.
In most cases,
the initial event appears to be the formation of a subcapsular hematoma.
Defective hemostasis,
due to thrombocytopenia or treatment of fever with aspirin,
may contribute to intrasplenic hemorrhage.
Spontaneous rupture of the spleen is an important and life-threatening complication and occurs in up to an estimated 2% of cases.
Most of the cases of spontaneous splenic rupture in malaria occur during acute infection and are associated with P.Vivax,
although there have been rare cases associated with other Plasmodium species. Fig. 6
3.4.
Hydatid disease
Hydatid cysts are almost always caused by Echinococcus granulosus and usually involve the liver or lungs but occasionally may also involve the spleen.
It is not often seen except in areas where it is endemic,
including Argentina and some Mediterrean countries like Portugal.
CT demonstrates a sharply marginated,
round or ovoid mass that has water attenuation.
Higher attenuation within the lesion may occur secondary to the formation of daughter cysts.
Ringlike calcifications may be seen in the periphery in inactive cysts.Fig. 7
3.5.
Spleen Tuberculosis
Infection with Mycobacterium tuberculosis of the spleen usually occurs in a miliary form by hematogenous dissemination.
On CT it appears as irregular areas of low CT attenuation,
as military nodules smaller than a few millimeters in diameter may not be discretely defined with current CT resolution.
Often there is mild splenomegaly.
When the lesions increase in size,
they may appear as small focal splenic nodules of low attenuation at CT.
Occasionally,
infarcts may occur from septic emboli.
Abdominal lymphadenopathy of low attenuation may be present.
Serial studies demonstrate evolutional change ultimately to calcium deposits,
representing healed calcified granulomas.
3.6.
Inflammatory Pseudotumour
An extremely rare lesion of the spleen consisting of a well-circumscribed mass composed of localized areas of inflammatory and reparative fibroblastic changes as well as a granulomatous component,
although its cause is still not clear.
CT demonstrates a rounded mass of low attenuation with inhomogeneous delayed enhancement.
Central stellate areas of low attenuation may persist within the mass,
corresponding to focal areas of fibrosis.
Calcification may be present.Fig. 8
3.7.
Sarcoidosis
Sarcoidosis is a systemic disease of unknown cause,
characterized by the presence of non-caseous granulomas and the proliferation of epithelioid cells.
Hepatic and splenic involvement occurs in 50-80% of cases,
tipically light and homogeneous hepatosplenomegaly,
usually associated with the typical pulmonary and mediastinal findings.
In about 5-15% of cases,
hypodense nodules (5-20mm) may be seen,
representing coalescent granulomas.Fig. 9
4.
SPLENIC CYSTS
Splenic cysts are usually found incidentally.
They only become symptomatic if large enough to cause extrinsic mass effect on adjacent organs or by developing complicating features of hemorrhage,
rupture,
or superimposed infection.
They can be divided into primary true cysts,
nonparasitic (epidermoid) or parasitic (echinococcai),
which possess a cellular lining,
and secondary false cysts,
which have no cellular lining and are presumed to result from trauma,
infarction or infection.
The contents of the cysts may be serous,
hemorrhagic,
inflammatory,
or degenerative from an infarction.
True and false cysts may be difficult to distinguish radiologically and histologically.
Typical CT findings are spherical,
well-defined cystic lesions with water attenuation,
thin or imperceptible wall and no rim enhancement.
In case of haemorrhage,
increased protein content,
or infection within the cyst,
a spontaneous hyperdense lesion can be seen. Fig. 10
5.
SPLENIC INFARCTION
The most common cause of splenic infarction is embolic,
occurring in cardiovascular disease.
Less frequent causes include local thromboses,
especially in hematologic diseases (eg,
myelofibrosis,
sickle cell disease,
leukemia,
and lymphoma) and vasculitis.
Fig. 11
Pancreatitis causing splenic artery aneurysm may also result in splenic vascular compromise and splenic infarction.
Areas of splenic infarction predispose an individual to splenic rupture and superimposed infection.
Classic CT findings are wedge-shaped,
peripheral,
hypoattenuating lesions,
best seen after contrast injection.
Areas of splenic infarction may also appear as heterogeneous,
poorly marginated,
hypoattenuating lesions that are indistinguishable from other splenic lesions,
including abscesses or tumors.
In the hyperacute phase,
a hemorrhagic infarct can reveal itself as an area of mottled increased attenuation.
In the acute and subacute phases,
infarcts tend to become focal and progressively better demarcated.
In the chronic phase,
infarcts may disappear completely,
but more commonly,
they reveal progressive volume loss caused by fibrotic contraction and occasionally calcification. Fig. 12
6. TRAUMA
The spleen is the most commonly affected organ in blunt injury to the abdomen.
On CT images,
lacerations appear as linear or branching hypodensity and there are usually subcapsular haematomas.
Active haemorrhage can be demonstrated as intra-splenic high-density material due to the extravasation of contrast media.
The 2018 revision of the American Association for the Surgery of Trauma (AAST) splenic injury scale is currently the most widely used grading system for splenic trauma and is based on CT findings.
Grade I
- Subcapsular hematoma <10% of surface
- Parenchymal laceration <1 cm depth
- Capsular tear
Grade II
- Subcapsular hematoma 10-50% of surface
- Intraparenchymal hematoma <5 cm
- Parenchymal laceration 1-3 cm in depth
Grade III Fig. 13
- Subcapsular hematoma >50% of surface area
- Ruptured subcapsular or intraparenchymal hematoma ≥5 cm
- Parenchymal laceration >3 cm in depth
Grade IV Fig. 14
- Vascular injury or active bleeding confined within splenic capsule
- Parenchymal laceration involving segmental/hilar vessels with >25% devascularisation
Grade V
- Shattered spleen
- Splenic vascular injury with active bleeding extending beyond the spleen into the peritoneum
6.1.
Splenosis
Splenosis is an acquired condition defined as autotransplantation of viable splenic tissue throughout different anatomic compartments of the body.
It occurs after traumatic or iatrogenic rupture of the spleen.
On CT scans,
splenosis nodules can be easily mistaken for neoplasms,
lymphadenopathy or peritoneal implants.
Fig. 15; Fig. 16
They usually enhance in a similar fashion as the normal spleen,
without any visible washout.
If no normal spleen is seen,
splenosis gains weight as the most probable diagnosis.
If in doubt,
a Heat-Denatured Tc-99m Red Blood Cell Scintingraphy may be helpfull.
7. BENIGN NEOPLASTIC DISEASES
7.1.
Hemangioma
Hemangioma is the most common primary benign neoplasm of the spleen,
often found incidentally with radiologic and pathologic examinations.
Splenic hemangiomas may be multiple,
usually as part of a generalized angiomatosis (Klippel-Trenaunay-Weber syndrome).
Fig. 17 If the entire organ is replaced by hemangiomas,
it is called hemangiomatosis.
Although a benign tumor,
hemangioma is associated with life-threatening complications as spontaneous rupture.
Hemangiomas of the spleen may appear either solid or cystic on CT scans and may enhance after administration of contrast material in a similar fashion to that of hepatic hemangioma,
although,
in other cases,
the lesions are relatively avascular in nature or show slow filling of contrast material. Fig. 18 Likewise,
at ultrasound,
hemangiomas are usually hyperechoic nodular masses,
as with hepatic hemangiomas and hiperintense on T2WI in MRI examinations.
7.2.
Hamartoma
Hamartoma of the spleen is a rare benign tumour characteristically composed of anomalous mixtures of normal elements of splenic tissue.
Hamartomas are usually incidental solid lesions that may contain a cystic or necrotic component.
They usually appear iso- to hypoattenuating on nonenhanced CT scans,
being occasionally hyperattenuating due to hemosiderin deposition.
After administration of contrast material,
prolonged enhancement may be appreciated on both CT and MR images. Fig. 19
7.3.
Lymphangioma
Lymphangioma is a vascular lesion filled with lymph.
They can involve the spleen exclusively,
or they may be part of generalized angiomatosis,
and are usually asymptomatic.
Splenomegaly may be present,
with single or multiple areas of low attenuation.
Lymphangiomas are sharply marginated and are not enhanced on postcontrast images.
Small,
marginal,
linear calcifications may be present.
8.
MALIGNANT NEOPLASTIC DISEASE
8.1.
Lymphoma
Splenic lymphoma may be classified as either primary splenic lymphoma or lymphomatous involvement as part of diffuse systemic involvement.
CT and MR imaging only detect splenic involvement in a small percentage of non-primary lymphomas because 45%-70% of splenic lesions manifest with either diffuse tumour infiltration in the spleen or tumour foci well under a centimeter in size.
The CT appearances of splenic lymphoma mirror the variety of pathologic appearances:
- Homogeneous enlargement
- Solitary hypoattenuating hypovascular mass
- Multifocal lesions
- Diffuse infiltration
Infarction of the spleen involved by lymphoma common.
Calcifications in splenic lymphoma before treatment are rarely detected.
On the other hand,
if found after treatment,
they can represent dystrophic calcification secondary to necrosis,
haemorrhage,
and subsequent fibrosis.
The overall accuracy of CT in depicting splenic lymphoma is approximately 58%-65%. Fig. 21
8.2.
Metastasis
Splenic involvement by metastases is seen relatively uncomm but not rarely at autopsy,
occurring in up to 7.1% of patients with malignancy.
Splenic metastases are believed to be mainly a result of hematogenous spread,
most commonly from breast (21%),
lung (18%),
ovary (8%),
stomach (7%),
cutaneous melanoma (6%),
and prostate (6%).
On CT scans,
splenic metastases are typically areas of slightly decreased attenuation in relation to the normal spleen.
Lesions may be well defined,
cystic or solid masses or infiltrative.
Calcification of metastases is rare unless the primary tumor is a mucinous adenocarcinoma.
Fig. 22
8.3.
Primary Angiosarcoma
A very rare malignant splenic neoplasm,
however the most common primary non-hematolymphoid splenic malignancy.
Unlike with primary hepatic angiosarcoma,
there is no known association between splenic angiosarcoma and occupational exposure to chemicals,
such as vinyl chloride or arsenic,
or prior injection with the contrast agent thorium dioxide.
CT may show splenomegaly with solitary or multiple nodular masses of heterogeneous attenuation due to necrosis and hemorrhagic areas,
with poorly defined contours.
Some may show peripheral enhancement similar to that of hepatic hemangiomas with the margins of the lesions often irregular or poorly defined.
Hemoperitoneum may be present.
Fig. 23