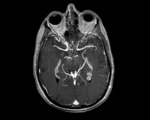
While in the body veins typically accompany arteries,
this does not exist in the brain where intracranial venous system is an articulate network made of veins and sinuses,
lacking of valves with potential bidirectional flow.
Cerebral veins may be subdivided into three subgroups:
1) superficial veins: further subdivided into a superior,
a middle,
and an inferior group draining mainly the upper surfaces of the cerebral hemispheres,
inferior frontal lobes and temporal poles
2) the “deep cerebral” veins: further categorized into medullary,
subependymal and deep paramedian veins collecting blood from the basal ganglia,
deep white matter and from most of the deep brain structures
3) veins of posterior fossa: likewise divided into three groups,
the "galenic",
the anterior and the posterior group responsible of drainage for the midbrain and posterior fossa structures
The cerebral venous drainage territories are both less familiar and more variable than the major arterial distributions.
We can recognize four basic drainage patterns: peripheral,
deep central,
perisylvian and posterolateral pattern and diagnosing venous occlusions depends on understanding these specific territories [1].
Cerebral vein and sinus thrombosis (CVST) first reported by Ribes in 1825,
is a particular form of cerebrovascular disease and accounts for 0.5-1% of all cerebrovascular diseases [2].
It affects mostly adults,
younger than 50 years old,
especially women in childbirth age and children.
CVST can be associated with significant morbidity and mortality [3] and an early diagnosis can make an important difference for patients outcome.
There are many recognized risk factors and causes for cerebral venous thrombosis: venous thromboembolism,
pregnancy,
oestrogen therapy/oral contraceptives,
thrombophilia or other hypercoagulability syndromes (antithrombin III,
protein S and protein C deficiency,
factor V Leiden,
polycythemia),
hypercoagulability associated with inflammatory disease,
head trauma,
local infections,
cancer and paraneoplastic syndromes [4,
5].
A separate chapter might include lumbar puncture and spontaneous intracranial hypotension (SIH) with the crucial role played by cerebrospinal fluid (CSF) pressure in development of vein thrombosis.
In SIH,
with a CSF leakage from the dural sac,
there is a downward displacement of the brain due to loss of CSF buoyancy,
traction on the dura and an increasing intracranial blood volume which causes the stasis of cerebral blood flow and leads to venous thrombosis [6].
In case of lumbar puncture,
low CSF pressure causes a downward shift of the brain,
with traction on the cortical veins and sinuses,
subsequent deformation of the venous walls and possible thrombosis [7].
However,
in 15% cases of CVST,
no direct cause or predisposing factor could be identified [8].
Clinical presentation of cerebral venous thrombosis (CVT) is nonspecific and extremely variable.
Presenting symptoms may include headache,
mostly in a subacute form developing over several days,
nausea,
altered consciousness,
visual disturbances,
neurological focal signs and epileptic seizures occurring in about one-third of affected subjects [9].
Being aware of this heterogeneous clinical presentation might support radiologists in formulating a correct diagnosis.
A prompt detection of CVT can avoid venous stroke,
which can present secondary to dural venous and sinus thrombosis in 1% of all acute strokes.