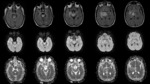
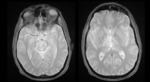
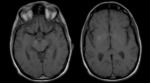
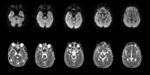
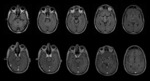
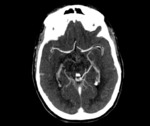
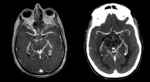
Potentially each cerebral vein and dural sinus might be affected by thrombosis: superior sagittal sinus is the most commonly affected,
followed by transverse and sigmoid sinus,
but both superficial (SCVT) and deep cerebral veins thrombosis (DCVT) can occur associated with it.
Thrombosis of deep cerebral veins,
meaning internal veins,
basal veins of Rosenthal,
vein of Galen and its tributaries has been found in 10% of patients [10],
almost always bilateral [1].
Basal vein of Rosenthal are paried paramedian veins,
closely related to the posterior cerebral artery.
They originate on the medial surface of the temporal lobe and run posteriorly and medially,
passing lateral to midbrain trough the ambient cistern to drain into the vein of Galen.
The anatomy of BVR was classified into three segments according to Huang and Wolf:
1) the first segment extends from the union of the inferior striate vein,
the anterior cerebral vein,
and the deep middle cerebral vein
2) the second segment extends to the union of the BVR and the lateral mesencephalic vein
3) the third segment extends to the point draining into the great vein of Galen or the internal cerebral vein
By using this classification some authors have tried to study different drainage patterns of BVR,
which results particularily complex due to variations of its origin in the longitudinal anastomoses between veins in the early embryonic stages [11].
Brain CT angiography can not reveal vessels of less than 1 mm diameter,
but with Multiplanar reconstruction (MPR) and MIP imaging,
can provide proper venous anatomy assessing their relationship with surrounding structures.
Different drainage patterns for each BVR might explain different lesion extension and eventually asymmetrical involvement of brain structures in case of unilateral or bilateral BVR occlusion.
To our knowledge there are only very few cases in literature describing isolated basal vein of Rosenthal (BVR) thrombosis,
with the first one reported with imaging only in 2004 by Owler et al.
Initial symptoms of BVR thrombosis are nonspecific and variable: most patients suffer from headache followed by rapid neurologic impairment (70%) [1].
Moreover they can present with short history of deteriorating consciousness,
seizures,
aphasia,
hemiparesis,
vomiting,
papilloedema,
visual disturbances,
coma or death.
When compared with patients suffering from sinus dural thrombosis,
subjects affected by deep cerebral vein thrombosis,
present more serious clinical conditions,
symptoms with more sudden onset and rapid progression,
worst outcome with death or long-term sequelae far more likely to occur [12].
Early unenhanced CT findings are subtle,
especially if performed short after symptoms onset,
with hypodense "fading" or "disappearing" thalami with effacement of the border between the deep gray nuclei and internal capsule as nonspecific findings of DCVT [1].
The most sensitive imaging technique for early diagnosis of DCVT is Magnetic Resonance Imaging (MRI) with Magnetic Resonance Venography.
MRI can detect local effects of venous obstruction and intracranial hypertension.
The first mechanism can cause localized brain oedema and venous infarction with enlarged,
swollen veins,
ischemic neuronal damage and petechial hemorrhages at pathological examination; the latter can merge and become large hematomas [7].
MRI can show two different kinds of cerebral oedema occurring in deep cerebral vein thrombosis: cytotoxic and vasogenic.
The first is caused by ischemia,
due to damage of the energy-dependent cellular membrane pumps,
leading to intracellular swelling.
The second type,
reversible if underlying condition is treated successfully,
is provoked by a disruption of the blood–brain barrier and leakage of blood plasma into the interstitial space [7].
In isolated thrombosis of BVR,
MR shows vasogenic oedema of affected side,
ischemic changes in deep white matter of temporal lobe,
thalamus,
hypothalamus,
basal ganglia,
mesencephalon and pons which appear hyperintense on T2-weighted and hypointense on T1-weighted images.
Based on signal intensity on T1 and T2 weighted images,
venous thrombosis can be divided in initial,
intermediate and late stage.
In first stage typical findings are the absence of flow-void and isointense vein signal on T1 and hypointense on T2 weighted images.
Beyond five days there is absence of flow with hyperintensity on both T1 and T2 weighted images.
At late stage (after two weeks),
recanalization occurs with resumption of flow-void in abnormal vessels [13].
In patients suffering from BVR thrombosis several cerebral structures are affected including the thalami,
basal ganglia,
mesencephalon and pons,
therefore vascular lesions,
mainly arterial infarctions,
tumors such as gliomas and tumefactive demyelinating diseases have to be considered in the differential diagnosis [14].
Diffusion-weighted imaging (DWI) can be used to differentiate arterial from venous infarction: brain territory involved in arterial infarction shows restricted diffusion due to cytotoxic oedema.
On the other hand in venous infarction,
cytotoxic and vasogenic oedema coexist and manifest as patchy areas of increased and decreased diffusion [15].
Although very rare in adults,
accounting only for 2% of adult brain tumors,
brainstem low grade gliomas should be considered in differential diagnosis.
In MRI gliomas can present as masses with compression of adjacent structures,
with normal findings in DWI,
a decreased intensity on T1 and increased intensity of T2 weighted images.
Spectroscopy might be useful for differential diagnosis showing an increase in the choline peak and overall in lipid/lactate fraction [16].
Another differential diagnosis hypothesis may include tumefactive demyelinating lesions.
They are characterized as mass-like lesions,
sometimes solitary or a couple of lesions,
greater than 2 cm in size,
affecting mainly women.
On imaging they tend to be large but with relatively little mass effect or surrounding oedema,
contrast enhancement in an open-ring pattern,
high ADC values and sometimes dilated veins have been observed within the lesions [17].
Lastly it is often difficult to differentiate BVR thrombosis,
clinically from other common causes of altered sensorium like metabolic encephalopathy or meningoencephalitis such as rhombencephalitis.
This inflammatory disease has a wide variety of etiologies including infection,
autoimmune disease and paraneoplastic syndrome.
In MRI a decreased intensity on T1 weighted images,
and increased intensity of T2 weighted images and in DWI,
with low values on ADC map might support this diagnosis [18].
The extension of the lesion sometimes might help to exclude this hypothesis from BVR thrombosis without involvement of the cerebellum in the latter.