Fourteen patients with newly diagnosed uterine cervical cancer pathologically confirmed underwent pretreatment MRI at our Institute from August 2017 to August 2018.
MRI was performed in each patient using a 1,5 Tesla magnet.
Prior to image acquisition,
an antiperistaltic medication was administered intramuscularly to limit bowel peristalsis and patients were invited to void their bladder to reduce movement and ghosting artifacts on T2WI.
MR images were acquired with patients lying supine using a five channels surface body coil to optimize image quality and reduce acquisition time.
The image protocol consisted in:
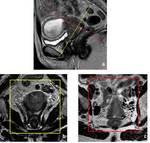
- T2-weighted (T2-w) sequences in the sagittal,
axial oblique and coronal oblique planes that means plans perpendicularly to the short and long axis of the cervical canal ( Fig. 1 );
- T1-weighted (T1-w) axial oblique sequences without fat suppression;
- DWI axial oblique sequence using fat-saturated technique with four b values (b=0 and 1000 s/mm2);
- 3D T1-weighted fat-suppressed isotropic and isovolumetric multiphase dynamic sequences on axial oblique and sagittal planes before and after administration of Gadolinium-chelates i.v.
ADC maps were generated on a voxel-by-voxel basis with the software built into the MR unit.
The main technique parameters used are shown in Table 2
Two radiologysts experts in gynecologic imaging retrospectively reviewed all MRI and assessed the presence or absence of PMI on the bases of T2WI and ADC values.
PMI was estimated in T2WI by disruption of low-signal-intensity cervical stromal ring,
with nodularity and /or soft-tissue extension into the parametrium.
ADC value was measured tracing manually a free-drawn region of interest (ROI) and including as much of the tumor as possible,
excluding cystic or necrotic areas [4].
MRI-based stage was assigned to each patients according to revised FIGO Classification system,
in which stage IIB determines the presence of PMI.
PMI is the crucial determinant whether the appropriate management would be surgical or chemo-radiation theraphy [1]
For patients who underwent surgery,
the histopathological stage was considered the gold standard (GS),
while for patients who needed chemo-radiation therapy the GS was set on a review consensus between expert gynecologists and radiologysts at our institution after correlation with MRI findings and all available data.
All pathological analysis were performed by faculty gynecologic pathologists at out Institute.
MRI-based stage were compared to the GS in each patient classifying them into two subgroups : < IIB or ≥ IIB according to presence or absence of PMI.
MRI stage accuracy in depicting PMI was analyzed and reasons for inaccurate staging were reported.