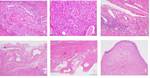
The study group comprised 14 patients, with a mean age of 50.04 years (+/-15.7 y/o).
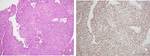
Squamous cell carcinoma was present in 12 patients,
while 1 case was an adenocarcinoma and 1 melanocytic tumor.
Eight\14 patients were suitable for radical hysterectomy,
5\14 underwent chemo-radiation therapy and 1\14 was enrolled into another center for surgery,
so that the final study population consisted of 13 cases.
In each patient the presence or absence of PMI was assessed using T2WI and ADC values as predicting tools.
Patients characteristic are summarized in Table 3.
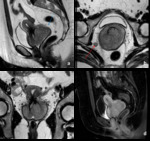
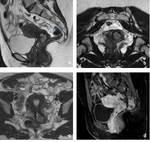
MRI stage was concordant with GS in 11\13 cases: 5\11 patients were correctly staged as IIB (true positive) on the basis of definite parametrium invasion (CASE 1. Fig. 2 ,
Fig. 3 ,
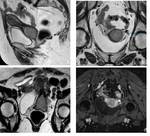
Fig. 4 ); 6\11 patients were classified as < II B (true negative) since the “hypointense rim sign” was clearly intact and it measured about 3 mm (CASE 2.
Fig. 5 ,
Fig. 6 ,
Fig. 7).
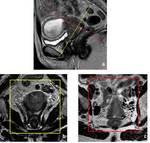
In two\ 13 cases (who had stage IIA),
MRI findings overestimated the presence of PMI (false positive),
probably due to tumor’s large size and to stromal edema; in these patients it was difficult to assess the intactness of the hypointense stromal ring,
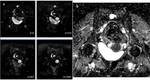
that was focally and irregularly thinned (Case 3.
Fig. 8,
Fig. 9 ,
Fig. 10).
The staging results of all patients are depicted in Table 4.
Sensitivity,
specificity,
positive predictive value,
negative predictive value and accuracy of MRI in detecting PMI were respectively 71.4%,
100%,
100%,
75% and 84.6%,
according to results reported in literature Table 5 .
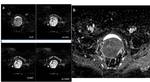
The results of our study demonstrated that ADC mean values (x10-3mm2/s) were significantly lower in patients with PMI (0.729,38+/-0.95,66) respect to ones without PMI (mean 1.013,80+/-0.192,21); p=0,001.
Furthermore,
the ADC values obtained in the presente study were comparable to those observed in a recent study by Woo S.
et al [4].
The two false positive patients had ADC mean values higher than those without PMI (0.853,80+/-0.163,55) Table 6 .