Type:
Educational Exhibit
Keywords:
Varices, Haemorrhage, Arteriovenous malformations, Diagnostic procedure, Contrast agent-intravenous, CT-Angiography, CT, Gastrointestinal tract, Abdomen
Authors:
A. Aguado, J. Elejondo Oddo, F. J. Barba Tamargo, K. Biurrun Mancisidor, A. Serdio, M. LETURIA ETXEBERRIA, M. Gredilla, L. calvo apraiz; Donostia - San Sebastián/ES
DOI:
10.26044/ecr2019/C-2448
Findings and procedure details
GI vascular lesions can be classified based on common morphology and enhancement patterns:
Angioectasias (Angiodysplasias): one of the most common causes of occult gastrointestinal bleeding.
Angioectasias consist of a proliferation of tortuous venules and capillaries within the submucosa.
They can appear anywhere in the GI tract,
but are most common in the colon,
particularly in the cecum and ascending colon.
The incidence of angiodysplasia increases with age,
but they can also be associated with other conditions such as aortic stenosis,
renal failure or hereditary hemorrhagic telangiectasia.
On multiphase CECT angioectasias appear as focal areas of enhancement (< 5mm in size) or bulbous swelling of the intramural vessels.
The enhancement is maximum on portal phase and they rarely enhance during the arterial phase.
Bleeding is usually low grade and stops spontaneously in more than 90% of cases,
but it can be chronic,
recurrent,
or even acute and life-threatening.
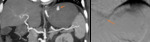
Arterial lesions:
- Dieulafoy lesions: consist in histologically normal arteries that maintain an abnormally large caliber despite their peripheral and submucosal location.
The lesion generally protrudes through a small mucosal defect.
These lesions are typically located in the stomach and,
when occurring in the small bowel,
most in the duodenum.
They may cause intermittent arterial bleeding and may be difficult to identify endoscopically.
- Arteriovenous fistulas (AVFs): formed by a direct connection between an artery and a vein.
They are most often acquired (iatrogenic or traumatic penetrating injury).
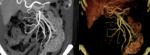
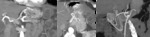
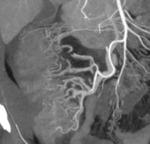
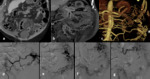
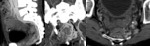
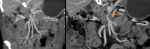
- Arteriovenous malformations (AVMs): consist of feeding arteries,
draining veins and a nidus of multiple dysplastic vascular channels connected by one or more fistulas.
AVMs are typically located in the colon,
congenital,
and are usually solitary and large.
In the small bowel,
AVMs most commonly affect the jejunum.
The small AVMs seen in elderly patients may have different pathogenesis,
probably acquired,
evolving from the more frequent angioectasias.
Arterial lesions present maximum enhancement during the arterial phase and may become invisible on venous and delayed phases.
A tiny nidus of enhancement on the arterial phase usually indicates the site of the lesion.
When associated with an early draining vein on the arterial phase,
the lesion most likely represents an AVM.
In the absence of an early vein,
Dieulafoy lesions cannot be distinguished from AVFs or AVMs.
Because these arterial lesions are exposed to high pressure,
they can cause life-threatening bleeding.
Venous lesions (angiomas and varices).
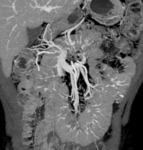
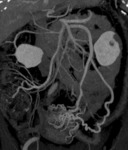
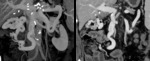
- Varices are abnormally dilated and tortuous veins,
formed in the setting of mesenteric venous hypertension.
On multiphase CECT,
varices appear as well-defined,
tubular or serpentine collateral vessels with same enhancement as adjacent veins.
- Venous angiomas are rare lesions of the GI tract that may occur in isolation or may be associated with Klippel-Trenaunay or blue rubber nevus syndrome.
On multiphase CECT angiomas may show a progressive globular enhancement,
similar to that of hepatic cavernous hemangiomas.
Endoscopic therapy is the first-line treatment in easily accessible lesions.
However,
in some cases endoscopy is not effective,
such as large AVMs or lesions located in the small bowel.
Surgery or angiographic embolization are other treatment options.
Surgical resection of AVMs is often difficult and carries the risk of complications (hemorrhage,
incomplete removal,
organ injury).
Hence,
endovascular therapy,
alone or combined with surgical resection,
has become a therapeutic option for patients with AVMs.