REVIEW OF THE SUBECT
Uterine anatomy
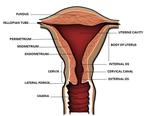
The uterus is anatomically divided into two regions: the body and the cervix,
reaching an approximate length of between 6 and 9 cm in pre-menopausal women.
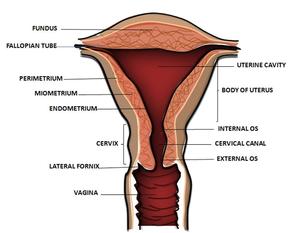
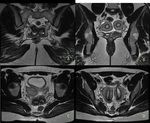
Fig. 1: Uterine anatomy
From the histological point of view,
three layers can be distinguished in the body: serous layer,
myometrium and endometrium.
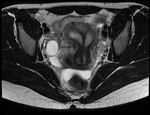
Fig. 2
Variable uterine position: the most frequent one is the anteversion,
but it can also be either in retroversion or anteversion with a displacement to either the left or the right with respect of the middle line.
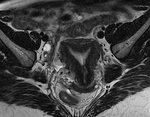
Fig. 3 and Fig. 4
In MRI:
- T1: The uterus is isointense to muscle.
- T2: In pre-menopausal women,
three different areas are differentiated:
- A hyperintense,
central area corresponding to the endometrium and its secretions
- A hypointense,
intermediate layer called the “union area” which corresponds to the most internal layer of the myometrium.
It has more water content and a bigger amount of compact,
smooth muscle.
The normal thickness of the union area fluctuates between 2 and 8 mm and it is a key factor when staging gynecological tumors.
The myometrium presents an intermediate signal.
The cervix in MRI is ( Fig. 5 ):
- Uniformly isointense in T1.
- In T2,
four areas can be differentiated:
- The most hyperintense,
internal area,
which corresponds to the mucous membrane,
endocervical glands and the mucus produced by them.
- The hypointense,
fibrous stroma.
- A more external layer with intermediate intensity signal and poor amounts of stroma.
After the administration of gadolinium,
the endocervical canal is enhanced rapidly,
while the stroma presents a more gradual enhancement.
Benign uterine pathology
The prevalence of uterine congenital pathology oscillates between 3-10% due to the different techniques and classifications used to diagnose them.
In patients with recurrent miscarriage,
its prevalence can increase up to 30%.
Ultrasound has demonstrated a 90-92% diagnostic accuracy in the study of uterine malformations compared to almost 100% of the MRI
The MRI allows to evaluate both the exterior and the inside of the uterine cavity,
providing information on non-communicating endometrial cavities,
muscular and/or fibrous walls...
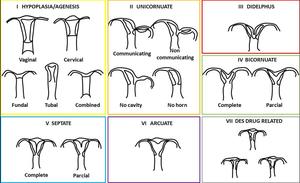
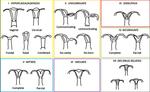
Fig. 6: Classification of the malformations of the Müller and Gibbons ducts modified
Development disorders
TYPE I: HYPOPLASIA / AGENESIS
It is caused by an alteration in the normal development of the Müllerian ducts.
Patients consulted for primary amenorrhea in adolescence.
It is necessary to exclude alterations in the process of sexual differentiation and to demonstrate the existence or absence of uterine body and cervix,
and its presence is a predictive factor of fertility.
However,
the existence of a working body without a cervix requires a hysterectomy to prevent endometriosis.
The Mayer-Rokitansky-Küster-Hauser syndrome is a combined malformation with absence of uterus and the superior part of the vagina.
The ovaries and the fallopian tubes are intact. Fig. 7
TYPE II: UNICORNUATE UTERUS
Asymmetrical anomaly with a single uterine horn which opens to the vagina.
The MRI is characterized by:
- Reduced uterine volume with normal anatomy and a single fallopian tube.
Sometimes a rudimentary contralateral horn that is not communicated with a uterine cavity can be found.
If the hipoplasic horn is non-communicated there is a higher frequency of endometriosis and its surgical resection is necessary.
Of all the congenital uterine alterations,
it is the one with the lowest fetal survival rate and most related to congenital renal alterations (usually renal agenesis)
TYPE III: DIDELPHYS UTERUS
It is presented as two normally divergent uteri and necks.
The vaginal septum may be associated with any uterine malformation but is more often associated with didelphys uterus.
Sometimes septum can be obstructive and condition hematocolpos.
Fig. 8
Fusion disorders
TYPE IV: UTERUS BICORNIS
It is the result of a partial fusion of the Müllerian ducts (of the uterine horns).
It can be partial or complete.
The diagnostic criteria in the MRI are:
- Presence of a fibrous and muscular septum that separates the uterine horns.
- Presence of an indentation in the fundus bigger than 1 cm of depth,
better seen in coronal shot sequences.
Fig. 9
Non-degenerative defects
They condition the existence of a septum,
a septate uterus (type V) or a small indentation,
arcuate uterus (type VI).
TYPE V: SEPTATE UTERUS
It is the most frequent uterine malformation and presents a high rate of infertility.
It is due to a failure in the reabsorption of a septum after the complete fusion of both Müllerian ducts.
This septum can have a mixed fibrous and muscular component.
The external uterine perimeter is usually convex,
flat or minimally concave,
but the depth of this concavity is less than 1 cm,
unlike in bicornuate uterus.
Metroplasty is a surgical procedure used to treat this anomaly in order to increase fetal survival.
Fig. 10
TYPE VI: ARCHED / ARCUATE UTERUS
It is considered a variant of normality.
It consists in a small indentation of the fundus and the endometrial canal with a normal external perimeter.
It has no implications in female fertility.
Fig. 11
Related to diethylstilbestrol
TYPE VII: RELATED TO DIETHYLESTIBESTROL
Diethylstilbestrol (DES) is a synthetic estrogen which was used as a medication to prevent and reduce the risk of miscarriage between the 1940’s and the 1970’s.
The fetal exposition to this medication causes uterine malformations,
including T-shaped uterus,
irregular stenosis and hypoplasia.
In the images developed in T2,
a focal thickening of the union area can be observed in the stenosis area.
It is a rare pathology nowadays.

Fig. 33: Acquired bening uterine pathology
1.- Benign pathology of the uterine body
Endometrial disease
Endometrial hyperplasia: excessive proliferation of the endometrium.
Endometrial polypus: endometrial excrescence.
Fig. 12
Myometrial disease
LEIOMYOMAS
The most frequent benign gynecological tumor.
It appears in up to 20-30% of women in fertile age.
They formed mainly of flat muscular cells,
separated by a variable amount of fibrous connective tissue.
Most of the patients have no symptoms and,
when they first appear,
they usually are metrorrhagia,
pressure on adjacent organs,
pain,
sterility or palpable abdominal mass.
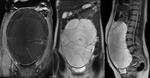
Fig. 13
According to their location,
they are classified as:
- Intramural: the most frequent,
have well-differentiated margins and can present a hyperintense ring due to the dilatation of lymphatic vessels,
veins and edemas.
- Submucous: the most symptomatic.
They can rarely get attached to an adjacent structure and have their vascular supply become independent from the uterus (“parasitic leiomyoma”).
Fig. 14
Leiomyomas can also present degeneration and the most frequent type is hyaline degeneration.
Up to 4% of them show cystic degeneration,
which consists of the formation of cystic spaces.
Myxoid degeneration presents itself as masses filled with gelatinous material.
Sometimes,
a massive failure of a leiomyoma takes place due to the obstruction of the draining veins arou nd the wound causing a red degeneration.
nd the wound causing a red degeneration.
There also exists a greasy degeneration.
It is rare,
and it usually happens in a myoma with advance hyaline degeneration.
Degenerated leiomyomas can have different aspects in images developed in T2 and post-contrast images.
Fig. 15 y Fig. 16
The differential diagnosis of the leiomyomas includes adenomyosis,
adnexal solid masses,
focal myometrial contraction and uterine leiomyosarcoma.
MRIs have also played an important role in the treatment of symptomatic leiomyomas for surgical planning and the monitoring of the response to the medical,
surgical or interventionist (embolization) treatment.
ADENOMYOSIS / ADENOMYOMA
Adenomyosis is a benign disease characterized by the presence of ectopic endometrial tissue in the myometrium,
present in 25% of all the hysterectomies.
The most frequent symptoms are: metrorrhagia,
dysmenorrhea and dyspareunia,
being asymptomatic in up to 35% of the cases.
In MRIs,
adenomyosis is defined as a thickening of the union are equal to or bigger than 12mm,
often with hyperintense,
dot-shaped focuses,
a finding considered pathognomonic.
These tiny focuses represent small deposits of dilated ectopic endometrium (cystic aspect) or hemorrhagic liquid.
It can be either DIFUSE or FOCAL.
It affects the whole uterus and produces a generalized increase of its thickness with a distribution pattern which is more irregular than homogenous.
The diagnostic criterium is a thickening of more than 12mm (normal < 8 mm).
Fig. 18
It is a thickening of a specific zone of the union area that looks like a mass.
Adenomyomas usually have vague borders,
elliptical shape and,
occasionally,
lineal striations which emerge from the endometrium.
Adenomyomas cause less distortion of the endometrium than leiomyomas of the same size.
The myometrium contractions may look like adenomyosis.
Fig. 19
2.
Benign pathology of the cervix
Nabothian cysts are the most frequent mass found in cervix.
They are caused by the distention of endocervical glands or crypts full of mucus,
which are rarely symptomatic,
even if their size can reach 4 cm.
In MRi, they have well-defined margins,
in T1 the intensity of the signal may be variable and present high intensity of the signal in T2. Fig. 20
Leiomyomas can also appear in the cervix and they can be easily distinguished from other cervical masses due to their well-defined margins and their hypointense aspect in sequences developed in T2.
Fig. 21 and Fig. 22
Endocervical polyps are benign cervical masses which cause frequent abnormal vaginal bleeding.
MRIs can show a cystic or solid polypoid mass in the endocervical canal or the vagina.
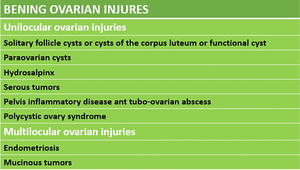
Fig. 34: Bening ovarian injures
1.
Unilocular ovarian injuries.
They are well-delimited cystic masses.
When there are no complications,
they are hypointense in sequences developed in T1 and hyperintense in sequences developed in T2.
Solitary follicle cyst or cyst of the corpus luteum or functional cysts
They are more common in women in reproductive age.
They are unilocular,
with smooth margins and they contain serous or bloody liquid.
Their diameter is between 3 and 8 cm long and they almost always come back approximately every 2 months,
so they require monitoring during several months.
Sometimes these cysts get complicated by ruptures,
abdominal pain and hemoperitoneum.
Fig. 23
Paraoavarian cysts
They are not ovarian masses,
but they emerge from mesonephric (Wolffian ducts),
paramesonephric (Müllerian ducts) or mesothelial structures.
They normally appear in the mesosalpinx,
between the ovary and the Fallopian tube,
so they be cystic masses near the round ligament,
with a thin wall and serous content. Fig. 24
Hydrosalpinx
When the hydrosalpinx is big,
it can even look like a cystic ovarian tumor.
Dilatated Fallopian tubes typically appear as structures full of liquid and with the shape of a “sausage”,
an S or a C,
when looked at in multiple levels.
Salpingitis and endometriosis are frequent causes of hydrosalpinx because they usually obliterate the fimbriae of the Fallopian tube.
Fig. 25
Serous tumors
This type of tumors is frequent (25% of benign ovarian neoplasms and between 12-23% of the bilateral cases).
Serous cystadenomas consist of unilocular or multilocular cysts filled with a light,
watery-like liquid and smooth surface,
even though they can present papillary projections.
The typical aspect in MRI of the serous cystadenoma is an unilocular cyst with a thin wall.
Pelvic inflammatory disease and tubo-ovarian abscess
It is an infection and posterior inflammation of the upper genital tract and,
sometimes,
the infection spreads to adjacent pelvic structures.
It becomes apparent as a clinical picture characterized by high fever and abdominal-pelvic pain in patients in fertile ages.
It is an infection by ascending infection and women wearing a IUD present a higher risk.
Tubo-ovarian abscess: rounded or tubular injury of thick walls.
Fig. 26
Polycycstic ovary syndrome
It is the most frequent endocrine alteration in women in fertile ages with important consequences: infertility,
anovulation,
endometrial hyperplasia,
Hyperandrogenism,
diabetes and cardiovascular diseases.
There is an unbalance between the LH and the FSH levels,
favoring the synthesis of androgens,
which cause the ovarian dysfunction.
The transvaginal ultrasound is still the chosen technique for its diagnose and the MRI is not appropriate for its study,
except for specific cases in which the ovaries cannot be visualized in the ultrasound.
Ovaries are considered polycystic when one of both present 12 or more follicle of between 2 and 9 mm in the surface or when the volume of the ovaries exceeds 10 cc.
Fig. 27
2.
Multilocular ovarian injuries
This group includes endometrial cysts and mucinous cystadenomas.
Endometriosis
Endometriosis is characterized by the presence of tissue like that of the endometrium outside the uterus.
Ovaries are the most frequent location and endometrial cysts normally present a thick fibrotic wall with hemorrhagic content whose color is like chocolate (“chocolate cysts”).
It is divided into three groups:
- Ovarian endometriosis
- Superficial pelvic endometriosis
- Deep or infiltrative pelvic endometriosis
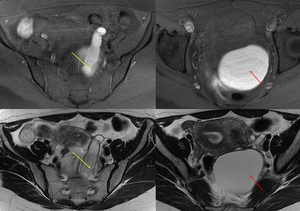
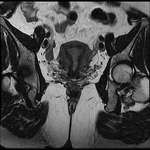
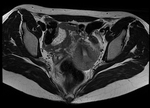
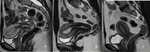
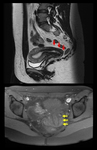
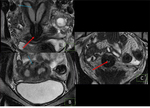
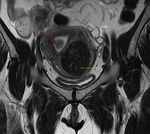
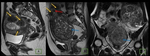
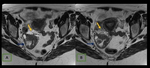
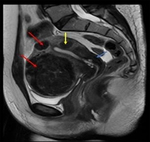
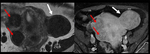
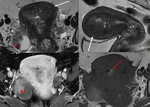
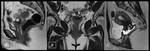
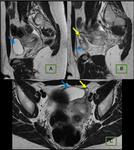
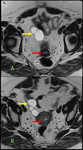
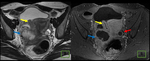
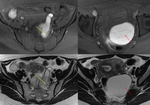
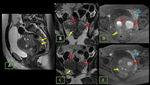
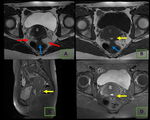
Fig. 28: Endometrioma (red arrow) and left Hydrosalpinx (yellow arrow) in sequence T1 saturation coronal fat (A) and axial (B) and T2 coronal (C) and axial (D), where endometrial polyp is also displayed.
Regarding its extension,
it can be:
- Located: endometriosis or chocolate cyst (ovary),
frequently multiple.
- Diffuse: more frequent.
It consists in small implants that affect the pelvic viscera and their internal fixations.
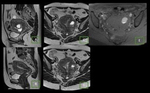
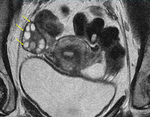
Diagnostic findings in MRI of ovarian endometriosic cysts Fig. 29
- Hyperintense injuries in T1 and T2 or hyperintense in T1 but hypointense in T2 (phenomenon known as shading).
A hypointense T2 and hypointense T1 entail stromal fibrosis.
This behavior is due to characteristic cyclical bleedings.
- The content of methemoglobin is what causes the shortening of T1 (hyperintensity in T1).
- The chronical cyclical hemorrhage and the high viscosity of the content of the cyst is what causes the shortening of T1 (shading).
These cysts present a multicentral growth and develop fibrous adherences.
Septa are signs of active endometriosis and thick walls are associated with stable,
old injuries.
T1 images with fat suppression improve the diagnosis of endometrial cysts and small peritoneal implants,
so it should be included in the routine and follow-up protocol in patients with endometriosis.
Fig. 30
Mucinous tumors
They are benign epithelial neoplasms,
usually bigger than serous cystadenomas,
characteristically multilocular with liquid of different intensity of signal inside and rarely bilateral.
If papillary projections are identified,
border line or low-level malign injuries must be ruled out.
Fig. 31