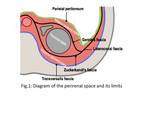
The perirenal space is a retroperitoneal space anteriorly delimited by the anterior renal or Gerota´s fascia and posteriorly by the posterior renal or Zuckerandl´s fascia (Fig.1).
The perirrenal space is the largest of three divisions of the retroperitoneum,
and is additionally divided into multiple compartments that contain the kidneys,
renal vessels and proximal collecting systems,
adrenal glands,
lymphatic and blood vessels and an adequate amount of fat.
The complexity of this space and the numerous structures we find in it,
make it susceptible to a wide variety of conditions,
both neoplastic and non-neoplastic.
Radiologists play an important role not only in diagnosis,
but also in differentiating some benign lesions from malignant ones,
and therefore,
lesions that will need surgery from others that will not.
Moreover,
they are also a key element in follow-up,
in detecting reappearances and in distinguishing them from normal alterations that arise as a consequence of treatments performed in this area.
The understanding of the normal anatomical,
clinical and imaging characteristics is essential in order to discriminate among the wide variety of entities happening in this space.
Diagnosis is generally possible with the use of non-invasive imaging techniques; computed tomography (CT) and/or magnetic resonance (MR),
which will allow,
on occasions,
diagnostic confirmation.
Ultrasonography (US) may suggest the presence of a lesion with fat echogenicity; however,
confirmation with another imaging technic is usually necessary.
Fat is easily recognised thanks to its characteristic appearance:
US usually shows a hyper-echoic lesion which may present rear acoustic shadow,
however,
there are exceptions and fat may present a different appearance.
US is rarely used for retroperitoneal masses characterisation and proper diagnosis,
although a large mass can be identified with US,
and sometimes be the first detected finding.
The attenuation parameters on CT depend on the physic properties of each tissue.
This together with the high spatial resolution CT provides an accurate measure of the attenuation values.
Fat on CT appears to have low attenuation values,
with quantitative measures ranging from -10 to -100 Hounsfield Units (UH).
These properties make CT the imaging study of choice.
Nevertheless,
lesions with small amounts of macroscopic fat may be difficult to identify,
as well as microscopic fat containing lesions,
which will not be detected on CT.
In the event of these two cases,
MR will be of assistance to resolve the presence or absence of fat.
On MR fat will exhibit hyper-intensity signals at both T1- and T2-weighted sequences.
This high signal intensity can,
at some occasions,
hide the intensity characteristics of surrounding tissues,
such as enhancement after Gadolinium injection or oedematous related hyper-intensities.
Other tissues or tissue components may also present high T1 and T2 hyper-intensity signals,
making differentiation between them and fat difficult.
Furthermore,
fat is also responsible for some artifacts that can cause diagnostic confusions.
Thus,
the use of specific sequences that suppress fat-tissue signal may be of use:
Fat-Saturation sequences: the most widely spread method to saturate and eliminate the signal of the fat.
It is based on saturation and change of the phase of fat protons causing them to lose their signal.
Therefore,
when using this sequence fat will no longer appear with high signal intensity.
Fat-Saturation sequences are the ones usually reserved for those situations in which CT is unable to typify macroscopic fat,
due to insufficient amount.
In-Phase and Out-Phase imaging: not an actual fat-suppression technique.
It uses the differences between signals of fat and water to emphasise the transition between them and subsequently characterise the tissues.
Normally used to asses for microscopic fat.