Cases of suspected IPF of the author’s clinical practice were collected.
The HRCT examinations were reviewed to look for the different radiological features of IPF according to the diagnostic criteria of the Fleischner Society.
Examples of the different HRCT patterns and findings are presented.
HRCT features frequently seen in UIP include honeycombing,
traction bronchiectasis and bronchiolectasis.
A fine reticular pattern and,
sometimes,
ground-glass opacification in the context of fibrosis may be present as well.
Honeycombing is a key characteristic of the UIP pattern.
It is defined as clustered,
thick walled cystic airspaces of typically consistent diameter (3–10 mm,
but occasionally larger).
It often presents as multiple layers of subpleural cysts on top of each other,
but it may also present as a single layer. The much smaller cysts seen in histopathological specimens - microscopic honeycombing - are beyond the spatial resolution of HRCT and often do not correlate with honeycombing on HRCT.
Traction bronchiectasis and bronchiolectasis are a hallmark of lung fibrosis on imaging and an important prognostic marker in UIP.
This feature represents irregular bronchial and bronchiolar dilatation caused by retractile fibrosis in the surrounding lung parenchyma.
It ranges from subtle irregularity and nontapering of the bronchial/bronchiolar wall,
to marked airway distortion and varicosity.
Distinguishing honeycombing from traction bronchiectasis can be challenging,
but it is diagnostically important,
since honeycombing increases the likelihood of UIP.
The reticular pattern is characterized by a network of fine lines.
On CT scans from patients with UIP,
reticulation is often irregularly spaced,
with a mixture of thick and thin lines.
Ground-glass opacification is defined as hazy increased opacity of lung with preservation of the bronchial and vascular margins.
Subtle ground-glass opacification superimposed on a fine reticular pattern represents fibrosis and may be seen in patients with IPF.
UIP is unlikely when pure ground glass opacity is present as an isolated finding of diffuse ILD.
The presence of abundant pure ground glass opacity in a patient with fibrotic ILD,
particularly in non-fibrotic areas of the lung,
suggests acute exacerbation or infection.
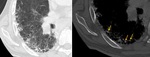
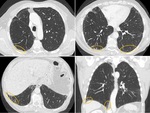
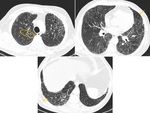
Occasionally,
fine linear or small nodular foci of calcification are observed within areas of fibrosis,
being more common in patients with UIP than in other fibrotic ILD (Fig. 1).
Typical UIP CT pattern
UIP is the hallmark radiological pattern of IPF.
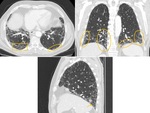
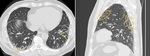
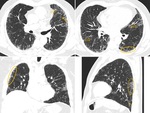
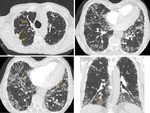
Typical UIP pattern is characterized by reticular opacities with obligatory honeycombing (Fig. 2 and Fig. 3).
It can be seen with or without peripheral traction bronchiectasis or bronchiolectasis (Fig. 2 and Fig. 3).
Groundglass opacification may be present,
but it is not a dominant feature and is usually mixed with reticular abnormality and honeycombing,
representing fibrotic changes (Fig. 2).
The characteristic distribution of UIP is subpleural with basal predominance (Fig. 2).
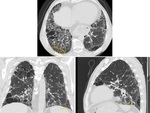
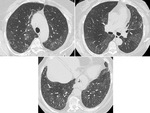
It is common to find some upper lobe involvement,
and in some cases,
the craniocaudal distribution of UIP may be relatively uniform (Fig. 3).
Asymmetric disease may occur in up to 25% of cases (Fig. 3).
Probable UIP CT pattern
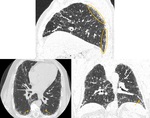
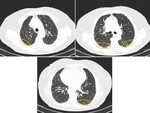
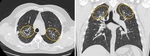
A probable UIP pattern is characterized by subpleural,
basal-predominant reticular abnormalities with associated peripheral traction bronchiectasis/bronchiolectasis,
but without honeycombing (Fig. 4 and Fig. 5).
As with a UIP pattern,
ground-glass opacification may be present,
but it is not a dominant feature.
Many patients with an HRCT pattern of probable UIP will be determined to have IPF since other factors such as histopathology are considered.
CT pattern indeterminate for UIP
Atypical HRCT features frequently accompany a histopathological pattern of UIP/IPF.
Therefore,
the category “indeterminate pattern” should be assigned when HRCT demonstrates features of fibrosis but does not meet UIP or probable UIP criteria and does not explicitly suggest an alternative diagnosis.
This category includes a subset of patients with evidence of fibrosis in a variable or diffuse distribution (Fig. 6, Fig. 7 and Fig. 8),
with some features that suggest a non-UIP pattern,
even though without ancillary findings of other pathologies.
CT features most consistent with non-IPF diagnosis
In some cases of fibrotic lung disease,
there is clinical suspicion of IPF,
but the HRCT imaging clearly suggests a pattern other than that of UIP.
Specifically,
a clear upper-lung or mid-lung predominance of fibrotic changes (Fig. 9); subpleural sparing with peribronchovascular fibrosis (Fig. 9); extensive consolidation (Fig. 10); predominant pure ground glass opacity (in a clinically stable setting) (Fig. 11); widespread mosaic attenuation with marked air trapping on expiration; diffuse nodules (Fig. 12) and cysts that are only very rarely observed in patients with UIP.