Overview:
Neurological complications developing in hemodialysis patients are multifactorial.
Neurological examination alone is usually not adequate to determine the underlying pathologies.
Imaging i.e.
MRI and CT scan of the brain is the most valuable tool frequently required for evaluation of neurological complications in symptomatic patients.
It is of great importance in not only evaluating the cause of neurological complains when the clinical assessment is inconclusive but also used for treatment response assessment. The imaging spectrum of this particular group of patients is infrequently studied.
We will address cause/ risk factors,
clinical manifestations and imaging findings in this particular group of patients.
- CEREBRAL ISCHEMIA AND INFARCTION:
Risk Factors:
- The occurrence of stroke is considerably higher among hemodialysis patients.
CKD greatly affects severity and outcome of both ischemic and hemorrhagic stroke.
- Traditional risk factors include hypertension,
diabetes,
hypercholesterolemia,anemia, atherosclerosis,
thromboembolic disease and intradialytic hypotension.
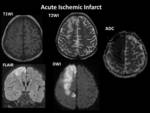
Imaging Findings:
- Conventional MRI i.e.
T2WI and FLAIR are usually normal for the first six hours of acute infarct.
Afterwards an increase in intensity,
swelling of gyri and effacement of sulci are noticed.
DWI shows restriction with low value on ADC.
- CT may be normal for many days in small infarcts.
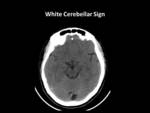
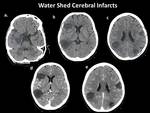
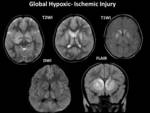
- Cerebral changes include acute infarction Fig. 1 Fig. 2 Fig. 3 Fig. 4 ,
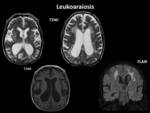
white matter changes Fig. 5 ,
and lacunar ischemic lesions.
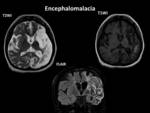
Chronic changes of infarction represented by encephalomalacia are often seen.
Fig. 6
- NON-TRAUMATIC INTRACRANIAL HEMORRHAGE:
Cause /Risk factors:
- ESRD patients are at increased risk of spontaneous intracerebral hemorrhage.
The pathophysiology of bleeding diathesis is complex that ranges from intrinsic platelet defects to uremic toxins,
infections and anticoagulant therapy during dialysis.
Imaging Manifestation:
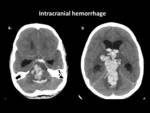
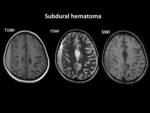
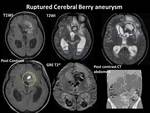
- Non traumatic cerebral hemorrhage may be intraparenchymal,
intraventricular Fig. 7 ,
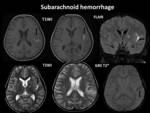
subarachnoid Fig. 8 and subdural Fig. 9 in nature. Fig. 10
- On CT scan,
acute blood appears hyperdense with gradual decrease in its attenuation towards resolution.
- MRI can very well demonstrate location,
evaluation and extension of intracerebral hemorrhage.
It also helps in assessing its cause.
- NON-TRAUMATIC CEREBRAL MICROBLEEDS (CMBs):
Cause/ Risk factors:
- Chronic Kidney disease is considerably linked to the presence and number of CMB,
as well as presence of CMB in deep locations.
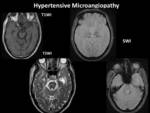
- Hypertensive microangiopathy also plays an important role as a causative factor of CMBs in hemodialysis patients.
Clinical Manifestations:
CMB are clinically silent in general,
but considered as a risk factor for future intracranial hemorrhage.
Imaging findings:
- Cerebral microbleeds are defined as small,
round or oval homogeneous low signal intensity lesions in T2-weighted gradient-echo (GRE) MRI and susceptibility-weighted imaging (SWI).
- They are not commonly seen on conventional MRI or CT
- CMBs secondary to hypertensive microangiopathy are characteristically present in deeper locations i.e.
pons,
basal ganglia,
cerebellar hemispheres. Fig. 11
- This is the same distribution as hypertensive intracerebral hemorrhages.
Cause /Risk factors:
- Dialysis techniques also introduce additional risk factors for infection.
Patients having central venous access catheters are at the highest risk of access-related infection.
- Systemic opportunistic and non-opportunistic infections are also identified.
Organisms:
Opportunistic bacterial infections include pathogens as Nocardia,
and Listeria monocytogenes.
Fungi often constitute Aspergillus,
Cryptococcus,
Candida,
Pneumocystis and Mucor species.
Mycobacterium tuberculosis is a principal cause in endemic areas.
Clinical manifestation:
The usual signs of infection in immunosuppressed patients are often attenuated soearly diagnosis is sometimes challenging.
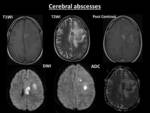
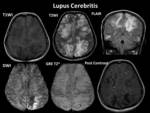
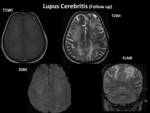
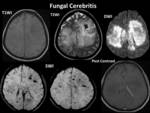
Imaging Manifestations:
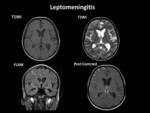
- Plain and contrast-enhanced MRI helps to illustrate the cerebral infections better than CT scan.
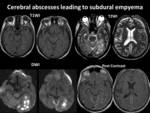
Such complications include meningitis Fig. 12 ,
subdural empyema,
cerebritis/abscess,
ventriculitis Fig. 13 ,
Fig. 14 Fig. 15 Fig. 16 Fig. 17 venous and arterial infarcts,
venous thrombosis,
hydrocephalus,
and cerebral edema.
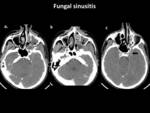
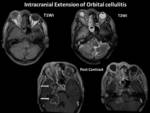
- Secondary cerebral infections from the contiguous extension of orbital and sinus infections are also well depicted on imaging.
Fig. 18 Fig. 19
- CEREBRAL VENOUS SINUS THROMBOSIS (CVST):
Cause / risk factors:
- Hypercoagulable events are also not uncommon among ESRD patients.
- Infections are traditionally recognized as common cause of CVST.
- In addition nontraditional risk factors for thrombosis,
such as hyperhomocysteinemia,
malnutrition,
inflammation and endothelial dysfunction are present in a significant number of chronic dialysis patients.
Clinical manifestation:
Initial symptoms include a headache,
raised intracranial pressure and seizures.
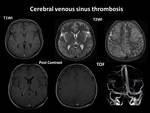
Imaging findings:
- A non- contrast CT scan of head is usually the first diagnostic imaging assessment performed in an emergency setting.
Hyperdense thrombosed sinus can be easily demonstrated.
- On conventional MR sequences Thrombus may manifest as absence of normal flow void.
- Secondary Intraparenchymal hemorrhages evolve through its traditional stages.
- Post Contrast imaging can show classic “Empty Delta Sign” Fig. 20
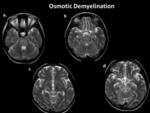
- OSMOTIC DEMYELINATION SYNDROME(ODS):
Cause/ Risk factors:
- Rapid correction of chronic hyponatremia is a well-recognized cause.
- Most patients with ESRD are subject to rapid osmotic fluctuations after hemodialysis which also attributes to ODS.
Clinical presentation:
Acute progressive quadriplegia,
dysarthria,
dysphagia followed by alteration of consciousness.
Distribution:
- Central Pons is the most common location.
- Extrapontine regions including the midbrain,
thalamus,
basal nuclei and cerebellum can be affected as well.
Imaging findings:
- On MRI brain classic “Trident shape appearance” is found in central pons. Fig. 21
- Extrapontine regions also demonstrate similar bilateral symmetric edema and demyelination.
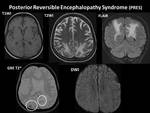
- PROGRESSIVE REVERSIBLE ENCEPHAOPATHY SYNDROME (PRES):
Cause/ Risk factors:
- PRES is often associated with an abrupt rise in blood pressure and it is a frequent finding in ESRD patients.
- The uremic environment of ESRD has also been suggested as an independent precipitating agent.
- The reversibility of this syndrome is well established.
Clinical presentation:
It includes severe headaches,
nausea,
vomiting,
seizures and visual and mental changes attribute to increase blood pressure.
Imaging findings:
- It is characterized by distinctive radiological findings in the cortical and/or subcortical part of the brain supplied by posterior circulation,
which may spread to basal ganglia,
brain stem,
and cerebellum.
- CT shows hypoattenuation in posterior brain while signals on MRI represent vasogenic edema. Fig. 22
- Frank Intracranial hemorrhage and microhemorrhages is known to occur in PRES in approximately 15- 64%.
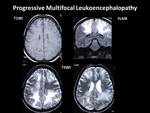
- PROGRESSIVE MULTIFOCAL LEUKOENCEPHALOPATHY (PML):
Cause/ Risk factors:
PML is a demyelinating disease caused by the reactivation of JCV Polyomavirus and infection of oligodendrocytes.
PML had been reported with the HIV patients with CD4 count less than < 200/uL.
However profound immunosuppression is a notable cause and it has also been reported in few cases with ESRD patients on hemodialysis.
Clinical manifestation:
Insidious onset and steady progression of focal symptoms that include cognitive,
motor,
speech,
behavioral,
and visual impairment.
Imaging findings:
- There are white matter abnormalities that are multifocal,
confluent,
involve cortex and subcortical areas with invariable involvement of Sub-cortical U-fibers in bilateral asymmetrical distribution.
Basal ganglia and cerebellum involvement has also been reported.
Frontal and parieto occipital lobes are frequently involved.
Absence of mass effect.
Enhancement is not commonly observed.
- CT brain reveals hypodense lesions of the affected white matter.
- MRI is far more sensitive to the presence of the white matter lesions.
MRI shows hyperintense lesions on T2-weighted images and FLAIR images in the affected regions.
Hypointensity is seen on T1WI.
Fig. 23
- METABOLIC ENCEPHALOPATHIES:
Encephalopathy is a common problem in ESRD patients that may be caused by variable factors.
Cerebral imaging is not necessarily required; but it can exclude other structural causes of neurologic symptoms.
Some of these having typical imaging appearances are considered here.
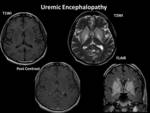
Uremic Encephalopathy:
Clinical manifestation:
It is characterized by,
instability of gait,
dysarthria,
action tremor,
asterixis,
multifocal myoclonus and unconsciousness.
Variation of clinical signs from day to day is typical.
Cause/ Risk factors:
The cause has been linked to uremic neurotoxins and it is improved by hemodialysis.
Distribution:
It typically shows basal ganglia,
thalami and midbrain involvement with uncommon involvement of cortical subcortical areas of parieto-occipital region.
Imaging findings:
- Lentiform Fork sign is its characteristic feature . Fig. 24
- On CT scan confluent hypodensity seen in these particular regions.
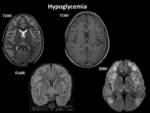
Hypoglycemic Encephalopathy
Cause / Risk factors:
CKD is an independent risk factor for hypoglycemia,
and exacerbate the risk already present in diabetics.
Clinical manifestation:
Typical symptoms of hypoglycemia are associated by measured plasma glucose concentration ≤70 mg/dL.
There are focal neurologic symptoms including,
aphasia,
hemiplegia and convulsion.
Hypoglycemic encephalopathy occurs in prolong and sever hypoglycemia.
Distribution:
- The characteristic findings occur in cortex of the bilateral cerebral hemispheres.
It can also be seen in hippocampus,
basal ganglia and corpus callosum.
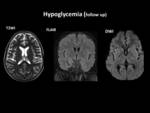
Fig. 25 Fig. 26
- Cerebellum,
thalami and brain stem are usually spared in adults.
Imaging findings:
Earliest findings are shown by DWI which shows restriction.
High signal intensity is seen on T2WI and Flair and low signals on T1WI.
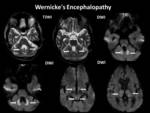
Wernicke’s encephalopathy
Cause/ Risk factors:
- It is not common in uremic patients,
but hemodialysis increases the risk because not only low thiamine intake but apparently also promoted loss of thiamine.
- Early identification is paramount because timely thiamine administration can reverse the clinical features.
Clinical manifestation:
It typically presents with the triad of ophthalmoplegia,
ataxia and cognitive symptoms.
It often remains obscured with high mortality.
Distribution:
Typically abnormal signals are seen in thalami,
mammillary bodies,
tectal plate,
and periaqueductal area in symmetric distribution.
Imaging findings:
CT is usually normal.
On MRI reversible vasogenic edema is seen.
Restricted diffusion may be seen.
Fig. 27
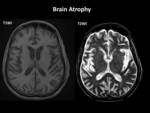
Cause / Risk Factors:
- Patients on hemodialysis show significant cerebral atrophy.
This corresponds to longer hemodialysis duration and cognitive deficits.
- The causes can be assigned to aluminium containing dialysate,
small vessel disease,
uremic intoxication,
malnutrition and anemia.
Imaging findings:
CT and MRI are equally able to demonstrate generalized cortical atrophy,
but MRI is more sensitive.
Prominent sulci and ventriculomegaly without bulging of the third ventricular recesses are seen.
Fig. 28
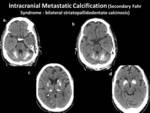
- CEREBRAL METASTATIC CALCIFICATIONS:
Cause/ Risk factors:
The most common causes of these calcifications with a striatum-pallidus-dentate distribution are the calcium– phosphorus metabolism disorders due to secondary hyperparathyroidism as a consequence of CKD.
Clinical manifestations:
- Symptoms can range from delirium,
dementia to seizures and focal neurological complains.
- Occurrence of extraskeletal metastatic calcifications increases with hemodialysis.
Imaging findings:
- There is symmetric involvement of basal ganglia,
thalami,
basal ganglia and dentate nuclei.
Subcortical white matter can also be involved.
- Areas of calcifications are best seen on non-contrast CT scan.
Fig. 29
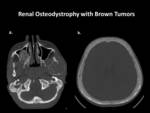
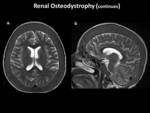
- RENAL OSTEODYSTROPHY (RO):
Cause/Risk factors:
The musculoskeletal disease associated with CKD is complex and multifactorial and are frequently seen.
Clinical Manifestations:
Varying neurological complains have been documented,
mainly related to the cranial nerves compression.
Imaging findings:
- Involvement of the cranial bones causes calvarial hypertrophy and narrowing of the neural foramina.
Widening of the diploic space is a common radiological finding.
- Brown tumors are also not uncommon.
Fig. 30 Fig. 31
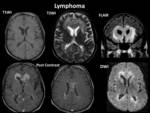
The immunosuppressive condition of patients with CKD is invariably associated with an increased incidence of neoplasia.
Although incidence of intracranial neoplasms is uncommon.
primary CNS lymphoma Fig. 32 have been described in ESRD patients.