Keywords:
Paediatric, Neuroradiology brain, MR, Diagnostic procedure, Cerebral palsy, Developmental disease
Authors:
M. Alonso, C. Sales Fernandez, M. Hernandez Herrero, M. Fajardo Puentes, V. Alvarez-Guisasola Blanco, T. Escudero Caro, S. G. Rizzo, M. Diez Blanco; Valladolid/ES
DOI:
10.26044/ecr2019/C-2636
Aims and objectives
Neonatal hypoxic-ischemic encephalopathy (HIE) in full term infants has been associated with a high risk for morbidity and mortality.
HIE is one of the most common causes of cerebral palsy (approximately 20%) and other severe neurological deficits in children.
Neonatal encephalopathy due to hipoxia-ischemia occurs in 1 to 1.5 per 1000 full term birth,
although the incidence decrease in the last years.
Prior to introduction of neuroprotection therapies,
the management of neonates with HIE was limited to supportive intensive care.
Since 2005,
large randomized clinical trials indicate that therapeutic hypothermia,
using either selective head cooling or sistemic cooling,
is an effective therapy for neonatal encephalopathy.
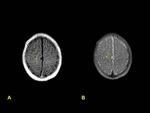
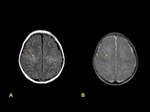
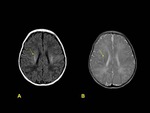
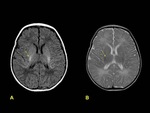
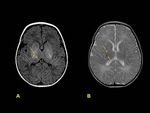
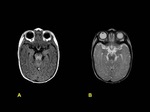
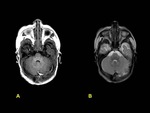
An appreciation of the abnormal MRI findings can only be gained by comparison with the normal appearance of the neonatal brain on MRI.
Two main points are important in order to conduct a correct interpretation: gestational age and myelination of the brain.
On T1-weighted images,
hyperintensity corresponding to myelination is observed in the posterior half of the posterior limb of the internal capsule in neonates after 37 weeks of gestation age,
being hypointense in T2-weighted images.
Myelinated structures are more metabolically active and the most vulnerable to the injurious effects of hypoxia.
Our objective was to describe the MRI findings in infants with moderate-severe hypoxic-ischaemic encephalopathy (HIE) treated with whole body hypothermia in our center.