PRENATAL DIAGNOSIS
Congenital pulmonary malformations are increasingly detected with the prenatal ultrasound (US) because of its routine use in prenatal care.
Advances in fetal MRI in recent years also played a role in detecting and understanding these malformations in utero.
Understanding these fetal chest masses is essential for appropriate monitoring during pregnancy,
treatment recommendations,
and management.
Fetal chest abnormalities are evaluated with US,
but MRI is an important adjunct technique for the assessment of these affections,
as it can provide excellent tissue contrast with a more accurate analysis of the fetal anatomy.
| ADVANTAGES |
ULTRASOUND (US) |
MAGNETIC RESONANCE (MR) |
| |
Increased availability |
No physical limitations like maternal obesity or oligohydramnios |
| |
Low cost |
Better fluid/solid distinction (contrast tissue) |
| |
Security |
Panoramic view |
| |
Good sensitivity |
Demonstration of cortical plate in the third trimester |
| |
The capacity of analysis in real time |
Functional studies |
| |
No ionizing radiation |
No ionizing radiation |
FETAL MR IMAGING TECHNIQUE
MR imaging sequences to evaluate fetal chest include fast sequences such as half-Fourier single-shot turbo spin-echo,
fast single-shot echo,
and free induction steady-state precession sequences.
T2 weighted images are the most useful for evaluating the lung anatomy.
PRENATAL LUNG LESIONS
a) Congenital Pulmonary Airway Malformation (CPAM)
CPAM is the most common congenital lung malformation and consists of an intrapulmonary mass of disorganized pulmonary tissue that may or may not have macroscopic cysts.
When present,
the cysts communicate with the airways and their vascular supply comes from the pulmonary circulation.
The most recent CPAM classification by Stocker consist of five types (Fig 3):
-Type 0: acinar dysgenesis or dysplasia of the trachea or bronchus involving all lung lobes- incompatible with life.
-Type 1: large cysts.
-Type 2: numerous small cysts less than 2 cm.
-Type 3: pulmonary hyperplasia.
-Type 4: large air-filled cysts resembling distal acinar.

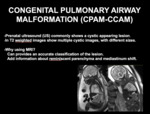
Fig. 3: INTRODUCTION CONGENITAL PULMONARY AIRWAY MALFORMATION
Prenatal US commonly shows a cystic appearing lesion.
In T2 weighted images multiple cystic images, with different sizes are observed.
The use of MRI in CPAM can be helpful to provide an accurate classification and to add information about reminiscent parenchyma and mediastinum shift (Fig 4 and 5).
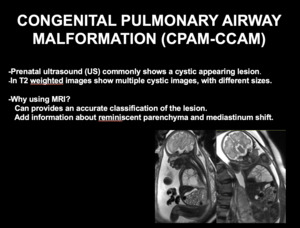
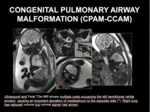
Fig. 4: US AND MRI IN CONGENITAL PULMONARY AIRWAY MALFORMATION.
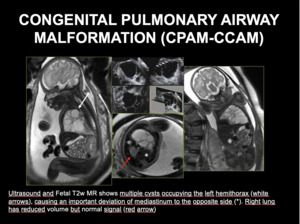
Fig. 5: CONGENITAL PULMONARY AIRWAY MALFORMATION (CPAM-CCAM). Ultrasound and Fetal T2w MR shows multiple cysts occupying the left hemithorax (white arrows), causing an important deviation of mediastinum to the opposite side (*). Right lung has reduced volume but normal signal (red arrow)
The natural history of and prognosis for a CPAM diagnosed in utero are variable and depend on the size of the malformation,
presence of pulmonary hypoplasia,
mediastinal shift,
and fetal hemodynamic alterations.
The presence of fetal hydrops is the main mark of a poor outcome.
In numerous cases of CPAM,
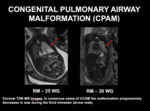
the malformation progressively decreases in size during the third trimester and mediastinal shift is solved so that the newborn is asymptomatic at birth (Fig 6).
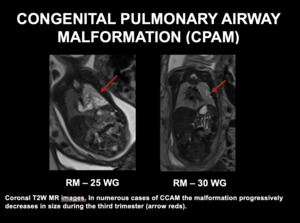
Fig. 6: CONGENITAL PULMONARY AIRWAY MALFORMATION (CPAM-CCAM). Coronal T2W MR images. In numerous cases of CCAM the malformation progressively decreases in size during the third trimester (arrow reds).
CPAM and malignancy:
CPAM probably does not degenerate into a malignant tumor.
No imaging method can differentiate cystic pleuropulmonary blastoma of such other cystic lesions
b) Bronchogenic Cyst
Bronchogenic cysts are developmental anomalies,
typically are unilocular,
fluid-filled,
or mucus-filled cysts lined by respiratory epithelium and are attached to but do not communicate with the tracheobronchial tree.
The lesions are more common in the mediastinum and near to the carina,
but can also be seen in the lung,
particularly in the lower lobes (Fig 7).
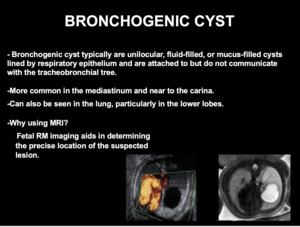
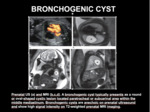
Fig. 7: BRONCHOGENIC CYST
Bronchogenic cysts are anechoic on prenatal ultrasound and show high signal intensity on T2 weighted prenatal MRI imaging (Fig 8).
Fetal MR imaging aids in determining the precise location of the suspected lesion.
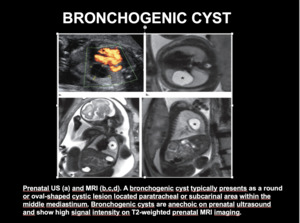
Fig. 8: BRONCHOGENIC CYST. A bronchogenic cyst typically presents as a round or oval-shaped cystic lesion located paratracheal or subcarinal area within the middle mediastinum. Bronchogenic cysts are anechoic on prenatal ultrasound and show high signal intensity on T2-weighted prenatal MRI imaging.
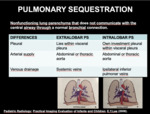
c) Pulmonary Sequestration (PS)
Pulmonary sequestration is a mass of pulmonary tissue that does not communicate with the central airway through a normal bronchial connection,
and that receives blood supply from an anomalous systemic artery.
Anatomically can be classified as intralobar (more common) and extralobar (Fig 9).
The differential diagnosis of extralobar pulmonary sequestration includes neuroblastoma and adrenal hemorrhage (Fig 13).
In cases of intralobar sequestration,
the differential diagnosis is CCAM type III.
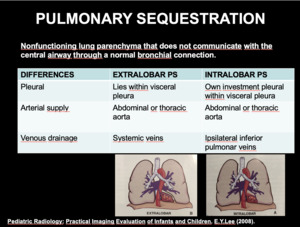
Fig. 9: EXTRALOBAR AND INTRALOBAR PULMONARY SEQUESTRATION
| DIFFERENCES |
EXTRALOBAR PS |
INTRALOBAR PS |
| Pleural |
Lies within visceral pleura |
Own investment pleural within visceral pleura |
| Arterial supply |
Abdominal or thoracic aorta |
Abdominal or thoracic aorta |
| Venous drainage |
Systemic veins |
Ipsilateral inferior pulmonary veins |
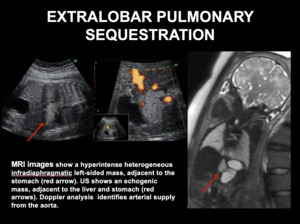
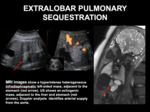
Fig. 13: EXTRALOBAR PULMONARY SEQUESTRATION
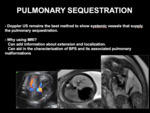
Doppler US remains the best method to show systemic vessels that supply the pulmonary sequestration,
although fetal MR imaging can add information about extension and localization (Fig 10 and 11).
MR imaging findings of PS usually include a solid,
well defined,
uniform,
hyperintense mass on T2 weighted images (Fig 12).
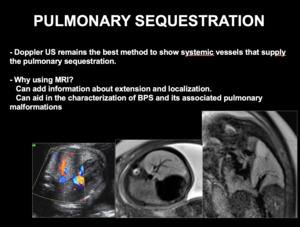
Fig. 10: PULMONARY SEQUESTRATION
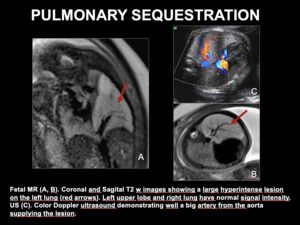
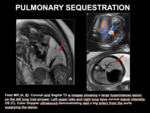
Fig. 11: PULMONARY SEQUESTRATION. Fetal MR (A, B). Coronal and Sagital T2 w images showing a large hyperintense lesion on the left lung (red arrows). Left upper lobe and right lung have normal signal intensity.
US (C). Color Doppler ultrasound demonstrating well a big artery from the aorta supplying the lesion.
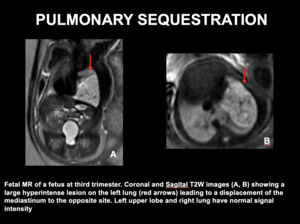
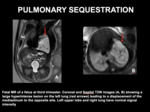
Fig. 12: PULMONARY SEQUESTRATION - Fetal MR of a fetus at third trimester. Coronal and Sagital T2W images showing a large hyperintense lesion on the left lung (red arrows) leading to a displacement of the mediastinum to the opposite site. Left upper lobe and right lung have normal signal intensity
Both types of PS may be associated with polyhydramnios and in utero hydrops,
due to compression of the esophagus and thoracic venous structures by a large lesion.
Pulmonary sequestration (PS) may also involute during gestation.
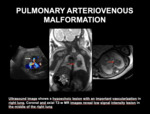
d) Pulmonary Arteriovenous Malformation (PAVM)
Almost 60% of Pulmonary Arteriovenous Malformations (PAVMs) result in abnormal communication between the pulmonary arteries and veins and most commonly occurs in the lower lobes.
Approximately two-thirds of patients have multiple lesions (Fig 14).

Fig. 14: PULMONARY ARTERIOVENOUS MALFORMATION
Fetal MR imaging can help in identifying multiples lesions at different sites and may show a hypointense irregular lesion on T2-weighted images,
usually adjacent to the hilum (Fig 15).
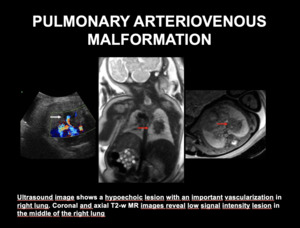
Fig. 15: PULMONARY ARTERIOVENOUS MALFORMATION - Ultrasound image shows a hypoechoic lesion with an important vascularization in right lung. Coronal and axial T2-w MR images reveal low signal intensity lesion in the middle of the right lung