Out of 46 noncommunicating hydrocephalus diagnosed by conventional sequences,
direct obstruction was seen in 21 patients and indirect signs of obstruction were seen in 25 patients.
Direct obstruction included aqueductal membranes in two patients,
tectal glioma in one patient,
pineal tumor in two patients,
Arnold Chiari malformation in four patients,
and achondroplasia in one patient.
Lilliquist membrane was seen in one patient but was only partially visualized and could not be traced to its full extent.
Colloid cyst causing obstruction of foramen of Monro was seen in one patient.
One patient of Dandy Walker variant and one patient of Blake pouch cyst were also seen.
Arachnoid cyst causing obstruction of fourth ventricle was detected in two patients.
Medulloblastoma causing obstruction of fourth ventricle was seen in one patient.
Metastasis was seen in four patients out of which two patients showed hemorrhage.
Out of 63 communicating hydrocephalus diagnosed,
14 patients were diagnosed as tuberculous meningitis,
3 patients as encephalitis,
and 1 patient as leptomeningeal carcinomatosa.
Subarachnoid hemorrhage was seen in two patients and choroid plexus tumor was seen in two patients.
The cause of hydrocephalus could not be found in 41 patients with conventional imaging and also we could not find any obstruction in these cases.
In three patients,
incomplete membranes were seen in grossly
dilated lateral ventricles.
In two patients,
hemorrhage was seen in germinal matrix region,
but we could not find its complete extension.
In all 88 noncommunicating hydrocephalus detected by 3D SPACE sequence,
the causes of obstruction was seen directly.
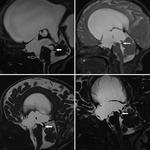
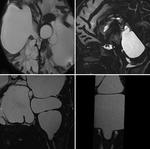
Overall 49 patients showed membranous obstruction (32 at the level of aqueduct [Figure 1],
7 at the foramen of Magendie,
2 at the level of Lushka,
1 at the level of foramen of Monro,
and Lilliquist membrane was seen in 7 patients [Table 5]),
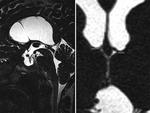
1 patient showed severe narrowing without membrane in bilateral foramen of Monro [Figure 2],
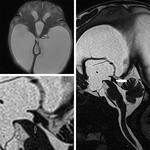
1 patient showed a tiny tumor at the level of aqueduct [Figure 3],
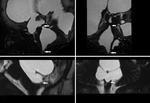
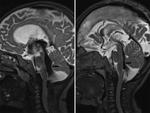
3 patients showed multiple levels of obstruction seen in both aqueduct and outlet of fourth ventricle giving the appearance of trapped ventricle [Figure 4],
and in another patient of postmeningitis hydrocephalus,
there were multiple septations and synechia causing multicompartmental obstructive hydrocephalus [Figure 5].
Other patients of obstructive hydrocephalus showed the similar findings as in conventional sequences.
In addition to the above said findings,
37 patients of chronic hydrocephalus showed multiple membranes in grossly dilated lateral ventricles,
which did not seem to be causing obstruction to the flow.
Similar membranes were seen in dilated third ventricle in 13 patients,
in fourth ventricle in 2 patients,
and in prepontine cistern in 1 patient.
These membranes were seen in both communicating as well as noncommunicating hydrocephalus,
significance,
and pathology of which are uncertain.
Thus,
in total,
we detected 102 membranes by using 3D SPACE sequence.
In cases of turbulent flow of CSF in cerebral aqueduct and outlet of fourth ventricle,
3D SPACE demonstrated flow void in 21 patients [Figure 6],
but in conventional sequences,
it was seen merely in 2 patients.
All the above findings were confirmed during surgery.
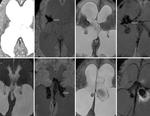
SWI detected hemorrhage in 27 patients (hemorrhage at the level of aqueduct in 2 patients,
foramen of Magendie in 1 patient,
chronic subarachnoid hemorrhage in 8 patients,
germinal matrix hemorrhage with intraventricular extension in 6 patients [Figure 7],
isolated lateral ventricular hemorrhage in 3 patients,
multiple hemorrhagic foci throughout cerebral hemisphere and brainstem in 1 patient of hemorrhagic encephalitis [Figure 8],
hemorrhage in 2 primary tumors (1 glioma and 1 medulloblastoma),
and hemorrhage in 4 patients of metastasis.
SWI detected 27 patients (24.7%) of hemorrhage in contrast to conventional sequence,
which detected only 6 patients (5.5%).