Type:
Educational Exhibit
Keywords:
Radiographers, Genital / Reproductive system male, MR physics, MR, MR-Diffusion/Perfusion, MR-Functional imaging, Education, Technical aspects, Physics, Cancer, Education and training, Pathology
Authors:
C. Tsiotsios, M. Eleftheriou, S. Kutsniashvili; Limassol/CY
DOI:
10.26044/ecr2019/C-2758
Background
Prostate cancer is the most common form of cancer and it ranks second in mortality rate among the male population worldwide.
Early diagnosis is the most effective method in dealing with and curing it.
Magnetic Resonance Imaging (MRI) of the prostate gland was first described in the 1980s,
with early publications describing the structure visualization using anatomical T2-weighted images.
Nowadays,
multiparametric MRI (mpMRI) of the prostate,
with exciting developments in hardware and software,
plays a prominent role in detection,
characterization and staging of prostate cancer.
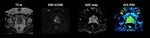
Multiparametric MRI of the prostate essentially combines anatomical and functional data for a detailed imaging assessment of the prostate gland (fig.
1).
Diffusion-Weighted Imaging (DWI) and Dynamic Contrast-Enhanced Perfusion-Weighted Imaging (DCE PWI) techniques are commonly used to supplement the standard anatomical imaging techniques (typically T2-w and T1-w).
Sometimes other functional techniques,
such as in-vivo Magnetic Resonance Spectroscopy (MRS),
are included.

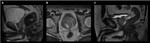
Fig. 1: Figure 1 shows an example of an mpMRI protocol of the prostate gland. Multiparametric MRI combines anatomical (T2-w) and functional (DWI, DCE PWI) sequences to increase the sensitivity, specificity and accuracy of the method.
The MRI Radiographer/Technologist plays a key role in the resultant examination quality,
as preparation,
positioning and communication with the patient,
protocol set up and selection of the acquisition parameters are crucial for obtaining high quality,
high resolution images of the prostate gland (fig.
2).
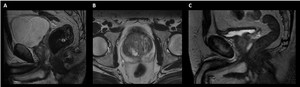
Fig. 2: Figure 2 demonstrates how insufficient patient preparation (A) and incorrect parameter choice (B, C) by the MRI Radiographer/Technologist, result to images with artifacts and blurring, which produce an overall poor quality examination.