• Anatomy of the sellar and parasellar region.
• MRI sellar protocol.
• WHO classification of pituitary tumors.
• MRI features: Tumor shape,
extension,
characteristics and enhancement patterns.
• Knosp’s and Hardys radiological classification.
• MRI evidence of macroscopic invasion of surrounding tissues and structures.
Introduction:
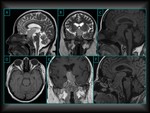
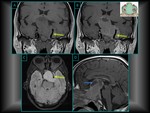
The sellar region is a central nervous system complex anatomical area composed by relevant anatomical structures.
The region is surrounded by suprasellar and parasellar structures.
This makes it essential to became familiar with all anatomical components.
(Fig.
1).
The pituitary gland develops by day 24 of gestation from the primitive oral stomodeus involving the diencephalon and it is later composed by two lobes (neuro and adenohypophysis).
Although the embryological development is complex,
the spectrum of most common pathologies that affect the region can be grouped into adenomas,
craniopharyngiomas,
meningiomas and less common entities such as hypothalamic gliomas or vascular anomalies.
A very useful mnemonic tool is often used: SATCHMO,
in order to remember most common pathologies in this area.
When studying the region it is important to include high resolution sequences and intravenous contrast protocols in order to achieve an accurate diagnosis.
We pretend with this review to give diagnostic tools that will help radiologist to achieve a correct diagnosis with subsequent treatment and follow-up.
PITUITARY MACROADENOMA:
It is the most frequent suprasellar mass in adults,
it arises from the pituitary gland and later it can extend to the suprasellar region,
invade parasellar structures and less frequently invade other anatomical regions.
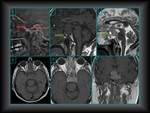
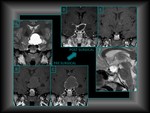
Usually,
it presents as an isointense solid mass compared with gray matter in T1 and T2 sequences,
although hyperintense cystic / necrotic areas,
as well as the hemorrhagic foci,
are relatively frequent. (Fig.
2).
After gadolinium injection these lesions usually enhace but with less intensity than normal glandular parenchyma.
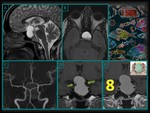
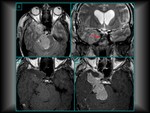
Cranial extension can compress the optic chiasma and gland suprasellar growth is responsible for the typical “snowman” morphology or the "eight shape" look,
due to the diaphragm membrane effect. (Fig.
3).
The so-called "invasive" pituitary adenomas may show invasion signs of the dural membrane,
bone and / or surrounding anatomical structures but truly malignant pituitary tumors (pituitary carcinomas) are only defined by the presence of metastases and are extremely rare,
with more aggressive clinical behavior,
resistance tendency to conventional treatments and early postoperative recurrence.
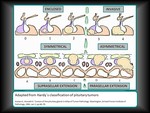
If we assess Hardy's classification (Fig.
4),
only grade III (focal bone erosion) and grade IV tumors (extensive bone erosion,
including the skull base) are considered invasive.
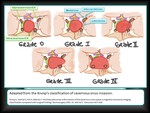
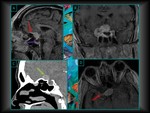
If we analyze Knosp’s classification (Fig.
5),
only III and IV grade adenomas are considered truly invasive (as they invade cavernous sinuses).
A sellar tumor should be defined as an aggressive type when it has macroscopic characteristics,
an unusually rapid tumor growth rate,
or clinically relevant tumor growth despite optimal standard therapies (surgery,
radiotherapy,
and conventional medical treatments).
(Fig.
6-7).
For tumor dimensions,
invasion and growth quantification,
MRI represents the best imaging method as it provides tools that help the radiologist to differentiate benign (typical) pituitary tumors from aggressive and potentially malignant pituitary tumors.
Some reports indicate that cavernous or sphenoid sinus invasion imaging findings may be more sensitive in invasive tumors identification compared to histology.
The most common aggressive pituitary tumors clinical presentation is early recurrence after initial pituitary surgery and rapid local growth as well as tumor extension.
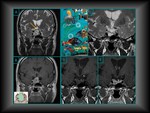
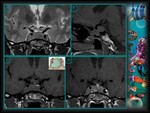
Cavernous sinus invasion MRI signs:
· Loss of normal boundaries between sellar parenchyma and cavernous sinus
· Venous compartments status in cavernous sinus.
· Cavernous sinus size.
· Cavernous sinus medial wall bulging
· Intracavernous internal carotid artery displacement.
· Knosp-Steiner parasellar extension degree.
· ICA enclosure percentage (Greater than 25%).
(Fig.
8-9).
NON-ADENOMATOUS SELLAR LESIONS
Craniopharyngioma:
Location: Sella Turcica and suprasellar cistern.
Along the pituitary stalk.
Age range: Childhood / adolescence (adamantinomatous type).
Elderly,
sixth decade (papillary type).
Although benign,
craniopharyngiomas tend to recur and invade adjacent structures.
Tumor adherence to surrounding vascular structures represent the most common cause of incomplete resection.
Adamantinomatous type: Shows solid and cystic components.
There is extensive surrounding inflammation and fibrosis.
MRI findings: Heterogeneous appearance,
hyperintense cystic components in T1W and T2W sequences.
The solid component shows moderate enhancement and calcifications may be present.
Papillary type: Occurs in adult patients.
They are solid,
without calcifications.
(Fig.
10).
Meningioma:
Location: Sella Turcica,
clinoid process,
lesser wing of sphenoid bone,
cavernous sinus.
MR image: T1W sequence - isointense.
T2W Sequence - 50% isointense,
40% hyperintense.
Intense homogeneous contrast enhancement.
Other diagnostic clues:
-Dural thickening (Dural tail sign).
-Identification of normal pituitary gland.
-Peripheric vasogenic edema.
-Associated hyperostosis.
-Vascular encapsulation pattern.
(Fig.
11-12-13).
Germinoma:
Location: Suprasellar cistern or pituitary fossa,
pineal gland,
posterior third ventricle.
Age group: Children and young adults,
with a higher prevalence in females.
They are infiltrating lesions.
MR image: Loss of normal signal intensity of the posterior pituitary gland.
Homogeneous and rarely cystic.
Sequence T1W- midly hypointense.
T2W sequence – isointense to grey matter.
Marked contrast enhancement present.
MR spectroscopy - prominent lipid peaks.
Teratomas - Heterogeneous signal,
with fat or calcifications.
Epidermoid and Dermoid Cysts:
Benign lesions,
slow expansive growth is characteristic,
they tend to insinuate within and around adjacent neural structures,
usually they don’t invade adjacent spaces.
They become symptomatic due to compression of adjacent neurovascular structures.
Epidermoid - Age group - Adulthood (2-4 decade).
Location - Basal cisterns and lateral situation.
MR Imaging: Slightly Hyperintense to CSF on T1W and T2W sequences.
DP and FLAIR - Epidermoid are hyperintense to brain and CSF whereas arachnoid cysts remain isointense to CSF.
DWI – epidermoid cysts show restricted diffusion,
whereas arachnoid cysts show facilitated diffusion.
Usually do not show any contrast enhancement,
calcifications rare.
Dermoids - Age group –Pedriatic age.
MR Imaging - Fatty components -Hyperintense on T1W sequence.
Areas of dense calcifications.
Chiasmatic and Hypothalamic Gliomas:
Age group - childhood,
(first decade).
Association with neurofibromatosis.
MR imaging findings: isointense on T1W sequence and hyperintense on T2W sequence.
Calcification and hemorrhage are uncommon,
contrast enhancement is variable.
They invade the brain along the path of the optic radiations.
Condrosarcoma:
Chondrosarcomas are cartilaginous,
off midline skull base tumors that occur in the middle cranial fossa.
Chondrosarcomas affect the cavernous sinuses because of their preponderance for petro occipital synchondrosis.
The tumor may displace the cavernous sinuses superiorly,
narrow them,
or invade them directly because of the inferiosuperior vector of growth.
On imaging,
chondrosarcoma is seen as a lytic-appearing lesion on CT,
which demonstrates rings and arcs of calcification.
On MR,
the tumor appears markedly hyperintense on T2WI,
shows chondroid matrix,
is locally aggressive,
and demonstrates variable enhancement.
(Fig.
14).
Chordomas:
Derived from remnants of the primitive notochord.
Age group: commonly third decade.
More frequent in men.
Location: In relation to clivus.
They are locally invasive and destructive.
MR Imaging: T1W sequence iso-hypointense.
T2W sequence extremely hyperintense.
(Fig.
15).
Metastasis:
Metastasis in pituitary gland are extremely rare,
seen in disseminated malignancies of breast and bronchogenic carcinomas.
They present with pituitary gland enlargement,
but without enlargement of the pituitary fossa.
Aneurysms:
Origin: cavernous portion of the internal carotid artery or its supra-clinoid segment,
occasionally anterior and posterior communicating arteries,
basilar artery tip aneurysm.
MR Imaging: usually well-defined lesions with signal void in T2 sequences.
If there is a clot inside the aneurysm it appears multilamellated high signal on T1W sequences.
MR Angiography can be done for accurate characterization.
Pitfall: Clinoid process pneumatization. (Fig.
16).