1.
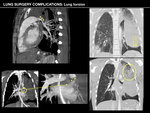
LUNG SURGERY COMPLICATIONS
Lung resection is considered the treatment of choice for bronchogenic carcinoma as well as for intractable end-stage lung diseases,
such as tuberculosis and bronchiectasis.
Thoracic surgical procedures can be divided into:
- Anatomic resections: pneumonectomy,
lobectomy and segmentectomy.
In these,
airways and pulmonary arteries and veins supplying the area of resection are carefully ifentified and ligated,
followed by regional parenchymal lymph node dissection.
- Non-anatomic resections: wedge resections,
bullectomy and lung-volume reduction surgery.
Surgical procedure differs in each of them and so do the expected postoperative changes as well as the potential complications.
Expected postsurgical appearance of the main techniques include:
- Pneumonectomy. Postpneumonectomy space is filled with air and fluid immediately,
gradually filling with more fluid than air.
Mediastinal shift to pneumonectomy space,
chest wall retraction and elevation of hemidiaghragm are progresively observed.
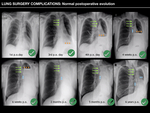
Radiologists should be familiarized with the usual evolution of pneumonectomy,
as an abnormal evolution (absence of signs of volume loss) should be suggestive of an underlying complication.
- Lobectomy.
Hyperexpanded remaining lung with mediastinal shift to operated side should be noted.
Other expected findings include intercostal space narrowing,
bronchial stump and ligated pulmonary vein.
- Segmentectomy.
In this case,
segmental bronchus resection with the patent main lobar bronchus constitute the usual postsurgical findings.
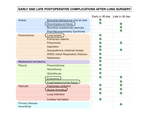
Postoperative complications are classified as early (onset < 30 days postoperative,
p.o.) and late (onset > 30 p.o.
day).
We will focus on:
- Bronchopleural fistula
- Empyema
- Lung torsion
- Stump thrombosis
- Esophagobronchial fistula
|
Bronchopleural fistula
Bronchopleural fistula (BP) refers to a direct communication between a bronchus and the pleural space,
but is often more generally used to indicate a persistent air leak form either the bronchi or the lung parenchyma.
It constitutes a potentially fatal complication,
being the most common cause of death following pneumonectomy when associated with aspiration pneumonia and subsequent Adult Respiratory Distress Syndrome (ARDS).
BP fistula is more likely to occur after right pneumonectomy due to the shorter length and less effective concealment of the bronchial stump,
as well as the greater vulnerability to ischemia (single bronchial artery on the right side).
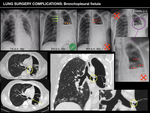
Imaging features on radiographies: because increased air and decreased fluid are cardinal sings of bronchopleural fistula,
it is important to monitor changes in the air-fluid level with sequential chest radiographies.
- Failure of postneumonectomy space to fill or persistent pneumothorax (despite correct tube drainage).
- Lack of mediastinal shift toward the operated lung to compensate for volume loss.
- Drop in the air-fluid level (increase in air-content).
- Reapparance of air in a previously opaque postneumonectomy space.
CT: It usually demonstrates an air-fluid collection in the pleural space and may also demonstrate direct communication from an airway to the pleural space.
Precise localization of the air leak,
its relative size and any associated complications could also be assessed.
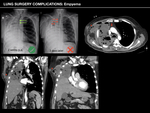
Empyema
Although advanced surgical techniques and potent antibiotics have rendered empyema an uncommon complication,
it remains a dangerous complication.
Sequential radiographs will show a rapid filling of postneumonectomy space or a new air-fluid level.
The main findings observed in CT include:
- Expansion of the postneumonectomy space with mass effect.
- Irregularly increased thickening and enhancement of the residual parietal pleura.
Lung torsion
This rare adverse event occurs when a lobe,
or the complete lung,
rotates around its bronchovascular pedicle.
It is more common after lobectomy,
but whole lung torsion may occur particularly in lung-transplantations (due to size discrepancies and anastomoses complexity).
The torsed lung compromises the airways,
the arterial blood supply and the lymphatic and venous drainage,
resulting in hemorrhagic infarction or necrosis in the affected lobes.
Imaging features
- Twisting of airways & vessels with a inappropiately directed hilar displacement.
- Abnormal orientation of fissures.
- Abrupt airway and vascular occlusion.
- Venous congestion results in increased volume,
with secondary bulging fissures.
- Obstructed venous outflow may also result in hemorrhagic infarction,
which will be represented with ground-glass opacities first and consolidations lately.
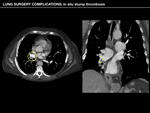
In situ stump thrombosis
Stasis of blood within the stump of a main pulmonary artery after pneumonectomy can lead to in situ thrombus formation.
Although generally considered to have a benign natural history with low propensity to cause embolic events,
in certain instances stump thrombus should necessitate anticoagulation (when a rapid size increase is seen or it presents as a late-onset complication).
In CT images,
it is observed as a hypodense filling defect adjacent to the artery ligation,
that might have convex margins (meaning acute thrombus) or concave ones (more commonly seen in chronic thrombosis).
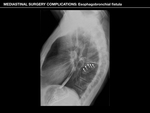
Esophagobronchial (EB) fistula
This devastating condition represents a heterogeneous group,
as it can result from at least three different mechanisms: surgical injury,
mediastinal cancer recurrence and chronic infection.
EB fistula can be difficult to diagnose.
- Its most common signs are postneumonectomy empyema and presence of previously ingested food particles in the operated space.
- Esophagography can aid in diagnosis by demonstrating an opacified fistulous tract towards the bronquial tree.
- CT can directly depict the fistua as well as the precipitating causes.
2.
POST-ESOPHAGECTOMY COMPLICATIONS
Esophageal resection is most commonly performed for the treatment of esophageal carcinoma.
Its surgical management includes esophageal resection,
regional lymph node dissection,
conduit isolation and anastomosis of the conduit to the residual esophagus.
A variety of surgical procedures are available as treatment modality for early-stage esophageal cancer.
The most common techniques are transthoracic esophagectomies (Ivor-Lewis and McKeown techniques) and transhiatal esophagectomy.
Variations of these techniques include different choices of conduit (i.e.
stomach,
colon or jejunum) to serve as a lieu of the resected esophagus.
Regardless of the performed surgical technique,
esophagectomy is a high-risk procedure associated with considerable morbidity and mortality.
Among the postoperative complications,
the following ones are widely described in the literature:
- Pulmonary complications (most important cause of early postperative mortality).
- Anastomotic leak or stricture
- Thoracic duct injury or Chylothorax
- Redundancy and delayed emptying
- Herniation of the abdominal viscera through the hiatus
- Reflux esophagitis
|
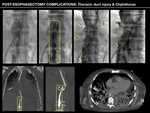
Thoracic duct injury and secondary Chylothorax
The thoracic duct is a posterior mediastinal structure originating at the Cisterna Chyli (usually located at level L2).
The duct ascends on the right and crosses to the left at approximately D4,
eventually emptying to the left subclavian vein.
Its injury is most often caused by penetrating trauma,
with surgical injury being the 2nd most common cause.
Thoracic duct injury impairs lymphatic drainage and predisposes to lymphatic leak,
with a resultant localized lymphocele or diffuse chylothorax.
Persistent loss of chyle causes a decrease in lymphocytes,
nutritional deficiencies and reduced immunity,
eventually leading to systemic infections.
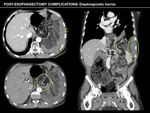
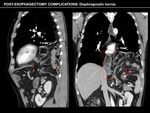
Diaphragmatic hernia
Diaphragmatic hernia is an uncommon but important complication of esophagectomy,
which can manifestate both in the immediate or late postoperative period.
Loosening of the diaphragmatic hiatus during surgery for transposing the conduit into the thorax predisposes to herniation of the abdominal contents into the chest.
Patients may present with progressive symptoms (such as delayed-emptying) or with hernia-related complications,
such as bowel obstruction.
3.
BREAST SURGERY COMPLICATIONS
Breast implantation surgery is increasingly performed worldwide.
Its main medical indication is breast reconstruction following mastectomy,
although it is also performed for aesthetic reasons The most important complications of this procedure include:
|
Common complications
|
Rare complications |
|
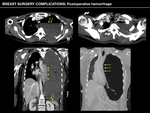
Early complications:
- Peri-implant fluid collection or hematoma
- Infection
Late complications:
- Capsular calcification
- Capsular contraction
- Foreign body reactions (siliconomas)
- Intra/Extra-capsular rupture
- Fat necrosis
|
- Retained foreign body (gossypiboma)
- Fibromatosis
- Pericapsular lymphoma & other uncommon neoplasms
|
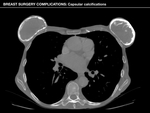
Capsular calcifications
Capsular calcifications,
which arise from the inner capsular surface,
are commonly observed with silicone implants because of increased likelihood of foreign body reactions.
They have a benign clinical course,
being most likely asymptomatic.
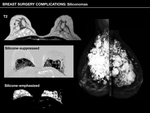
Siliconomas
Subcutaneous injection of free silicone for body contouring used to be performed mainly on the 50's and 60's,
although there has been a resurgence of this practice,
particularly in Asia and South America,
as it is much cheaper and faster than a prompt surgical procedure.
When free silicone is injected,
a foreign body reaction occurs,
leading to the formation of granulomas,
which are called siliconomas.
Patients that have undergone this unsafe procedure can develop silicone mastopathy,
that manifests with painful lumps and may mimick malignancy (nodular fibrosis & architecural distorsion) on imaging.
The main imaging features of siliconomas are:
- Mammography: disorganized high-density globular masses (± rim calcification).
- US: mixed echogenity.
The classic appearance is a highly echogenic pattern of scattered and reverberating echoes with a well-defined anterior margin and loss of detail posteriorly.
This pattern has been described as "echogenic noise" with an appearance similar to a "snowstorm".
- CT: Isodense nodulations with subcutaneous (infiltrative,
nodular or confluent pattern) and lymphatic involvement.
- MR: imaging modality of choice,
owing to specific silicone-emphasised and silicone-suppresed inversion-recovery sequences.
Siliconomas present high signal intensity in T2-weighted sequences.
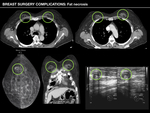
Fat necrosis
Fat necrosis is a benign non-suppurative inflammatory process of adipose tissue,
which usually results after surgical procedures.
Its diagnosis may result challenging due to its wide variety clinical and imaging presentations,
sometimes overlapping with breast carcinoma's way of presentation.
CT appearance is based on the main components found in this condition:
liquefied fat (low-attenuation HU),
fibrosis and inflammation.
Calcifications may be present,
which mean long-time evolution.
US will show hyperechogenic ill-defined nodules.
Fat necrosis presents no internal enhancement.
If it does,
malignancy should be ruled out.
4.
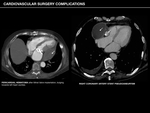
CARDIOVASCULAR SURGERY COMPLICATIONS
4.1.
CORONARY ARTERY BYPASS GRAFTING (CABG)
CABG for myocardial revascularization is the preferred procedure for high-grade and obstructive coronary atherosclerotic disease.
It is performed via median sternotomy to gain access to the heart.
The bypass is usually prepared with either internal mammary or saphenous vein grafts,
although radial and gastroepiploic artery grafts may also be used.
Its main complications are:
- Anastomotic leak/dehiscence
- Anastomotic stenosis
- Aneurysm or Pseudoaneurysm
- Graft dissection,
thrombosis with occlusion or kinking
- Aortic dissection
- Infection (mediastinitis,
empyema)
- Hemothorax / Hemomediastinum
- Lung injury
- Nerve damage
|
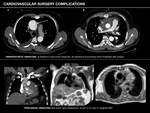
Saphenous vein graft (SVG) aneurysm
It is an uncommon but potentially life-threatening complication that may eventually lead to myocardial ischemia if aneurysmal-sac thrombosis occurs.
Because the therapeutic management is different,
it is important to differentiate between:
- True aneurysms.
They are primarily attributable to atherosclerotic disease,
thus being a late complication.
True aneurysms tend to be fusiform and can occur at any location along the graft.
Surgery is the standard of care.
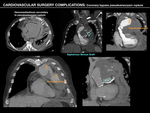
- Pseudoaneurysms.
These typically occur in the postoperative period as an iatrogenic complication and present eccentric and saccular morpholgy,
usually located at proximal anastomosis.
They are secondary to weakness of the venous wall,
injury during implantation,
dissection and anastomotic defcts.
Infections can also be contributory,
forming "micotic" pseudoaneurysms.
Pseudoaneurysms can be treated with minimally invasive techniques,
such as coil embolization.
4.2.
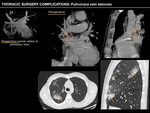
THORACIC AORTA GRAFTS
Thoracic aortic diseases such as aneurysms,
dissections, penetrating ulcers,
and rupture are treated with a variety of thoracic aortic reconstructive
procedures,
using tissue or synthetic aortic grafts.
During the follow-up of patients who have undergone this type of surgery, it is common to see small to moderate amounts of low-attenuation perigraft material within the first months.
This material probably represents a combination of seroma,
liquefying chronic hematoma,
fibrosis and granulation tissue.
However,
when the amount of low-attenuation perigraft material is abnormally large or it is increasing in amount,
infection with perigraft abscess should be excluded first.
Graft anastomotic dehiscence with blood leakage may also cause this appearance if there is no active leak at the time of the scanning,
the leak is too slow to detect or the timing of the CT is not optimal.