On T1-weighted sequences,
the signal intensity of the striated muscle is generally higher than that of water and much lower than that of the fat.
On inversion-recovery and fat-suppressed T2-weighted images,
normal muscle signal intensity is much lower than that of water but higher than that of fat.
Changes related to T2 prolongation due to muscle edema (intracellular or extracellular free water) are best appreciated in the sequence inversion-recovery and fat-suppressed T2-weighted images. Muscle edema is present in virtually all conditions that influence increased signal intensity.
The list of conditions that cause muscle edema is not extensive.
Therefore, it is important to know the main conditions that affect the muscles.
For that,
a simple acronym method would guide on that approach (Table 1).
TRAUMATIC / OVERLOAD INJURIES
Delayed-Onset Muscle Soreness
Definition: Delayed-onset muscle soreness (DOMS) is a stretching injury caused by unaccustomed,
prolonged,
or overly vigorous eccentric exercise.
Clinical findings: While strain injuries develop acutely during activity,
patients with DOMS report a gradual onset of muscle pain,
stiffness,
and swelling several hours or days after activity,
followed by spontaneous resolution within 1-2 weeks.
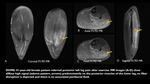
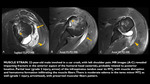
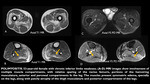
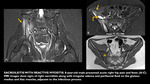
Imaging findings: Muscle enlargement and high fluid signal intensity on T2-weighted images (edema pattern) with preservation of muscle architecture,
affecting either a single muscle or a small group of functionally similar muscles,
without the MTJ localization typical of muscle strain or any architectural distortion.
MR imaging findings peak 3-5 days after injury,
but subtle residual alterations can persist for up to 80 days.
Inflammation and necrosis are not consistent features (Figs 1 & 2).
Compartment syndrome
Definition: Increased pressure in a relatively noncompliant fascial compartment,
resulting in ischemia of muscles and nerves.
Clinical findings: Generally,
the etiology is secondary to trauma (acute,
which is a life-threatening surgical emergency) or brought on by exercise (exertional,
on which pain persists despite rests and can become severe within hours). Patients with acute compartment syndrome often report pain in which the severity is out of proportion to the apparent injury,
sometimes along with paraesthesia,
pallor and pulselessness.
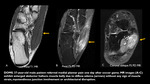
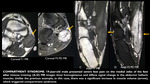
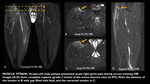
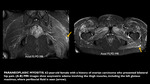
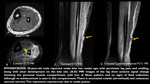
Imaging findings: muscular hyperintensity on T2-weighted or fast STIR images with muscular swelling.
No signal changes on T1-weighted images are noted (Fig 3).
Muscle Strain or Tear
Definition: Muscle strain is the most common muscle injury,
typically related to excessive stretching during eccentric muscle contraction in exercises or sports that emphasize speed and power.
Clinical findings: Symptoms occur acutely during or right after exercise.
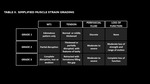
Traditionally there are three grades based on clinical severity (Table 2). Grade 1 is a mild injury resulting in pain without loss of range of motion and function.
Grade 2 is a moderate injury with loss of muscle strength and range of motion.
Grade 3 is a severe injury,
typically related to a complete tear,
with loss of function and a palpable gap.
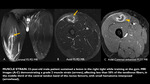
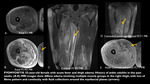
Imaging findings: The majority of strain injuries take place at the MTJ,
where interstitial edema and hemorrhage may be seen,
often extending along the adjacent muscle fibers and fascicles.
The presence of an edematous pattern only,
without the disruption of muscle architecture,
is commonly referred to as a grade 1 injury (Fig 4). The tendon at the MTJ may be completely normal or mildly thickened with abnormal signal intensity,
but without disruption or laxity.
Mild perifascial fluid may accompany grade 1 injuries.
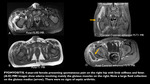
In addition to grade 1 features,
the presence of a partial disruption of muscle with hematoma formation around the MTJ is referred to as a grade 2 injury (Figs 4 & 5), with local distortion of muscle architecture depicted as a focal area of well-defined high signal intensity.
The tendon adjacent to the MTJ may be thickened and exhibit features of laxity.
Partial disruption may be depicted as well.
Moderate to severe perifascial fluid is often present in grade 2 injuries.
Complete disruption of the MTJ with a local hematoma filling the gap created by the tear is the main feature that represents grade 3 injuries (Fig 6). Complete avulsion injuries of the MTJ or tendons from the bony attachment are also considered to represent grade 3 injuries.
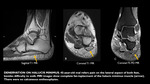
In peripheral myofascial junction injuries,
the edema pattern is depicted at the periphery of muscles and focal fascial or adjacent muscle fibers disruption may occur.
This pattern of injury is common at the distal gastrocnemius and soleus as their aponeuroses converge to form the Achilles tendon,
demonstrating fluid accumulation between them in up to 50% of cases,
because aponeuroses lack adherence proximally due to the presence of an interposed plantaris tendon (Fig 7). A prominent amount of fluid in such injuries can lead to overgrading the strain,
as it is often disproportionate to the degree of underlying tissue damage.
Sometimes,
it can be difficult to differentiate muscular strains from DOMS.
In that case,
some radiological patterns,
as well as the patient's history,
can be of assistance (Table 3).
INFLAMMATORY MYOPATHIES (Table 4)
Dermatomyositis and Polymyositis
Definition: Autoimmune inflammatory conditions of skeletal muscle characterized by gradual onset of muscle weakness in the thighs and pelvic girdle.
Dermatomyositis also involves the skin.
Topography: Firstly,
they involve the proximal lower limb,
especially the hamstrings,
vastus lateralis e vastus intermedius muscles.
Then,
they ascend to involve the buttocks,
proximal upper limbs,
neck flexors and pharyngeal muscles.
Imaging findings: symmetric edema with preserved muscle architecture (Fig 8), usually associated with subcutaneous e perifascial thickening.
In dermatomyositis,
amorphous muscle or fascial calcification may be evident.
At chronic stage,
MR can show symmetric muscle atrophy,
and sheet-like calcifications may develop in dermatomyositis.
Other myopathies have similar findings like those mentioned above.
Muscular edema and preservation of the architecture with adjacent soft tissues edema are common to all.
However,
soft tissue calcifications are not seen.
They also preferably affect the proximal muscles of the lower limbs.
Some clinical aspects should be mentioned to strengthen the diagnostic suspicion of other inflammatory myopathies.
Myositis associated with cancer: probably related to an autoimmune response against neoplastic cells.
Usually found in malignant conditions such as lung,
genitourinary,
gastrointestinal carcinomas,
ovarian carcinomas (Fig 9) and non-Hodgkin lymphomas.
Myositis associated with connective tissue disease: Inflammatory myopathy may be found in patients with autoimmune connective tissue disorders,
for example,
rheumatoid arthritis,
scleroderma,
Sjögren syndrome,
systemic lupus erythematosus (SLE) and mixed connective tissue disease.
HIV-related myopathy: It encompasses the diagnoses of polymyositis,
drug-related myopathy e pyomyositis.
Polymyositis is more common than pyomyositis,
frequently observed in immunosuppressed patients.
Other HIV-related myopathies include rhabdomyolysis,
necrotizing non-inflammatory myopathy,
subclinical myopathy,
and denervation caused by HIV-related peripheral neuropathy.
Drug-related myopathy: It generally affects buttocks,
quadriceps,
adductors,
and deep calf muscles.
It is characterized by symmetrical muscular edema.
The temporal correlation between the drug and the onset of symptoms is important.
Commonly related drugs:
- HMG-CoA reductase inhibitors (statins)
- Antiretroviral drugs (Azidothymidine)
- Corticoids
- Anabolic agents
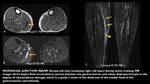
Pyomyositis
Topography: Thigh muscles are commonly involved,
specially the quadriceps,
followed by the gluteal and psoas muscles.
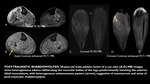
Imaging findings: Muscle edema and perimuscular fluid.
Also,
muscle architecture may be affected,
due to coarse fluid collections (Fig 10 & 11). Other important features are abscesses,
described as areas of nonenhancement with high signal on T2-weighted images.
Intralesional gas may be evident.
There is also extensive edema of nearby soft tissues.
A condition that must be differentiated from pyomyositis is myositis reactive to an infection of adjacent structures,
represented by non-uniform edema of muscle fibers that are in proximity to the infectious agent (Fig 12).
Myonecrosis
Definition: Muscle necrosis,
caused by sickle cell crisis,
diabetes,
compartment syndrome,
crush injury,
severe ischemia,
intraarterial chemotherapy,
and rhabdomyolysis.
Any condition that cause myonecrosis can simulate an abscess at both clinical evaluation and MR imaging.
Diabetic myonecrosis,
a distinctive myopathy,
presents with severe pain,
most frequently in the thigh muscles,
and mild fever.
Topography: Affects the anterior thigh or calf.
However,
can be multifocal.
Imaging findings: Muscle architecture is compromised due to necrotic areas.
T2-weighted images show heterogeneous and hyperintense signal,
owing to the combination of hemorrhage,
edema and necrosis (Fig 13). T1-weighted images may show mid hyperintensity,
due to hemorrhage.
Perifascial edema is often seen.
Gadolinium contrast may show homogeneous nonenhancement,
before the stage of liquefaction.
Rhabdomyolysis
Definition: Loss of integrity of muscle cell membranes with the release of intracellular contents.
Clinical findings: trauma,
severe exercise,
ischemia,
burns,
toxins,
intravenous heparin therapy,
and autoimmune inflammation are the main etiologies. Rhabdomyolysis is potentially life-threatening although recovery is excellent with early treatment.
Muscle pain,
weakness,
and dark urine are described,
along with increased serum creatinine kinase (CK) values.
Imaging findings: coarse and heterogeneous edema throughout the involved muscles,
which may progress to findings of myonecrosis (Fig 14).
DENERVATION MYOPATHY
Topography: Muscles that share a common innervation,
which can be due to abnormalities of the central nervous system,
spinal cord,
peripheral motor nerve (entrapment neuropathy by coursing through a fibro-osseous or fibromuscular tunnel,
as well as mass impingement) or neuromuscular junctions.
Imaging findings: Depends on its duration.
Acute – Signal alterations precede changes at electromyography.
T1-weighted images are normal.
T2-weighted images show diffusely and uniformly increased muscle signal intensity.
There is no perimuscular fluid around the affected muscle.
Subacute – T1-weighted images begin to show atrophy.
High signal intensity remains on T2-weighted images.
Chronic – No more signal intensity changes are seen.
However,
the muscle is fat-replaced,
which means it has irreversible damage (Fig 16).
An important role of MR of a surgically correctable cause of nerve compressions such as a bone spur or ganglion cyst.