Endometriosis is defined as the presence of endometrial tissue outside the uterus.
This condition manifests in as many as 10% of women of reproductive age (1).
It manifests as dyspareunia,
dysmenorrhea and
infertility,
although it may be asymptomatic.
Three different forms of endometriosis exist: ovarian endometriosis (endometrioma),
peritoneal endometriosis and adhesions,
and deep endometriosis [2].
ETIOLOGY AND PATHOGENESIS:
The etiology is multifactorial,
several theories exist.
-Retrograde menstruation is the most accepted,
with transportion of endometrial tissue from the uterine cavity into the peritoneum through the tubes.
-A second theory suggests that the Mesenchymal cells present on the serosal surfaces (coelomic epithelium) or remnant Müllerian tissue can be differentiated into endometrial cells.
-A third theory is the induction,
which is a combination of the other two theories.
It suggests that the endometrium secretes substances that induce undifferentiated mesenchyme to form endometrial tissue[3,4].
SYMPTOMS ,
DIAGNOSIS AND EVALUATION TECHNIQUES:
Pelvic pain and infertility are the major symptoms of endometriosis and the results of the clinical examination vary according to the localization of endometriosis.
There are also non-specific signs such as adnexal mass non mobilizable uterus and ovaries and Infiltration of Douglas-pouch and recto-vaginal septum.
The correct diagnosis is fundamental in defining the best treatment strategy for endometriosis.
Therefore,
non-invasive methods are required to obtain accurate diagnoses of the location and extent of endometriotic lesions.
Transvaginal sonography and magnetic resonance imaging are used most frequently to identify and characterise lesions in endometriosis.
Diagnosis is difficult when ovarian endometriomas are absent and endometriosis causes adhesions and deep infiltrating nodules in the pelvic organs.
Magnetic resonance imaging seems to be useful in diagnosing all locations of endometriosis,
and its diagnostic accuracy is similar to those obtained using ultrasound[2].
The MRI is an excellent method for identifying old hemorrhagic content that characterizes the endometriomas ) and allows the identification of the sub-peritoneal implants and implants hidden by adhesions because of its large field of vision,
multiplanar capability and high spatial resolution [5].
ECHOGRAPHY:
The most frequent locations of endometriosis are the ovaries in 42% of cases.
* In its typical form,
the endometrioma is seen as an oval formation presenteing a regular shape with finely echogenic and homogeneous content,
unlike non-endometriotic hemorrhagic cysts where echoes are more rugged.
There is no Doppler signal within the endometrioma.
* In its atypical form the endometrioma is seen as a thick-walled cyst,
containing hyperechoic areas similar to dermoid cysts or cysts with very little echogenic content.
MRI TECHNIQUE:
It is recommended to perform MRI study in the first half of the menstrual cycle to increase the sensitivity of the detection of small hemorrhagic foci of endometriosis.
In order to decrease the angle of uterine anteversion,
a moderately filled bladder is required,
resulting in better evaluation of the pelvic structures.
A half-filled bladder displaces the bowel superiorly leading to bowel movement artefacts reduction.
An antiperistaltic drug such as glucagon (1mg) should be administered intravenously or intramuscularly.
To achieve better extension of vaginal and bowel walls,
vaginal opacification (50 mL) and rectal opacification (150 mL) with ultrasound gel are recommended by some authors [6].
The mostly used standard imaging protocol included T2-weighted fast spin echo sequence performed in sagittal,
coronal and axial planes and T1-weighted fast spin echo sequence performed in axial plane.The protocol also includes T1-weighted fast spin echo fat saturation sequence performed in axial and sagittal planes.
For lesions smaller than 1 cm,
T1-weighted sequences with fat saturation appear to be the most sensitive in detecting these lesions.Aspectrally selective fat suppression sequence allows the differentiation between hemorrhagic or fatty content of cystic lesions (endometriomas or dermoid cysts) and the increased detection of small implants.
Some authors avoid contrast-enhanced imaging due to the lack of a definite consensus concerning its indications [7].
Recent technical advances in diffusion-weighted imaging(DWI) significantly enhanced the value of abdomen and pelvic MRI.
The degree of restricted diffusion in biological tissues has been shown to inversely correlate with tissue cellularity and the integrity of cell membranes.
DWI should
be performed in axial plane using a single-shot echo planner imaging (EPI) sequence with SPIR technique and with b value of 500,
800,
and 1000 [8].
In our institution we use 1.5 T (Siemens Medical Solutions) magnetic resonators,
using multiplane axial,
sagittal and coronal T2-FSE weighted sequences and T1 SE weighted axial sequences with or without pre contrast fat suppression.
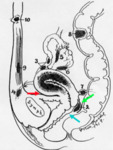
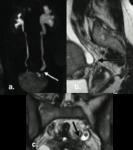
Axial and /or sagittal images are also obtained after intravenous injection of gadolinium based contrast (Figure 1).
IMAGING CHARACTERISTICS OF ENDOMETRIOSIS:
MRI signs are highly polymorphic but can be characterised by the presence of lesions with haemorrhagic content of variable intensity,
depending on the production of haemoglobin degradation products and their age,
which may appear hyperintense with T1-weighting if recent or reasonably recent,
hypointense with T1-weighting if old lesions,
and be very variably intense in T2-weighting but generally hypointense [9].
More or less retractile fibrous lesions that are usually hypointense in T1 and T2-weighting are the second type of typical occurrence seen in MRI.
1.
ENDOMETRIOMAS
Ovarian and peri-ovarian endometriosis:Endometriomas (> 1 cm) or micro- endometriomas (< 1 cm) are characterised by intra-ovarian lesions of variable signal intensity,
generally persistently hyperintense in T1-weighting on fat suppression sequences which are almost pathognomonic,
and usually hypointense with T2-weighting[9].
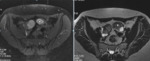
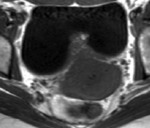
The lower T2 signal intensity of endometriomas compared with that of functional,
or simple,
ovarian cysts has been described as "T2 shading" [10] (Figure 2).
Bilaterality and multifocality of adnexal lesions,
along with the other characteristics discussed and illustrated in the following sections,
can help establish a diagnosis of endometrioma with even greater specificity than T1 signal hyperintensity alone[11].
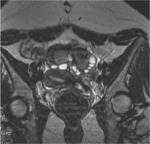
There may be associated retractile peri-ovarian adhesions with a star-like appearance and variable intensity in the ovarian fossae which may in some cases bring the ovaries towards the midline area producing ''kissing ovaries''[9] (Figure 3).
Endometriomas,
and solid endometrial implants ,
also demonstrate restricted diffusion .
Endometriomas have low ADC values in part because of "T2 blackout effects".
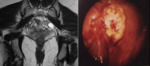
On a diffusion-weighted image obtained with a low b value (which is a type of T2-weighted fat-suppressed image),
an endometrioma exhibits low signal intensity resembling the T2 shading .This,
endometriomas have less signal intensity to lose on images obtained with higher b values than adnexal masses with higher T2 signal intensity do[11] (Figure 4).
2.
TUBAL ENDOMETRIOSIS:
Unilateral or bilateral dilatation of the fallopian tubes very often with a heterogeneous signal,
unlike true hydrosalpinx,
may indicate an endometriotic origin.
In the majority of cases,
these haematosalpinx are associated with other ectopic locations and are rarely isolated.
The presence of T1-weighted hyperintensity within a dilated fallopian tube is suggestive of endometriosis and may be the only finding at MR imaging in some women[12].
T2 shading may be absent in these cases because women with endometriosis develop dilated fallopian tubes secondary to endometrial implants on the serosal surface of the tubes,
as opposed to implants within the tubes [13].
3.
DEEP PERITONEAL ENDOMETRIOSIS:
Deep endometriosis corresponds to implants at a depth of more than 5 mm.
Unlike endometriomas,
deep endometriosis implants may have different characteristics on the MR image.
Most of these are hypointense on T2-weighted sequences as well as on T1.
This hypointensity is due to a desmoplastic reaction with fibromuscular proliferation.
They have poorly defined borders with infiltrative appearance,causing retraction of organs or surrounding structure.The presence of hemorrhagic foci,
hyperintense on T1 sequences with and without fat suppression,
is a very characteristic MRI finding for endometriotic implants,
but is seen less often in deep implants than in adnexal lesions[14].
Implants can be enhanced with gadolinium; however this feature is neither sensitive nor specific.
Coutinho and colleagues[15] divided the anatomic locations of solid endometriosis lesions into anterior,
middle,
and posterior compartments of the pelvis,
placing the anterior rectosigmoid colon and the uterosacral ligaments in the posterior compartment and the round ligaments and bladder in the anterior compartment.
Uterosacral Ligaments:The uterosacral ligaments are considered the most common location of solid endometriosis (63).
Affected women may present with pelvic pain,
including dyspareunia.
Anterior Rectosigmoid Colon:Deep infiltrating endometriosis (DIE) infiltrating the bowel is estimated to be found in 31%.Most common sites of bowel involvement are the rectum and rectosigmoid (65.7%)
The MR imaging features of solid rectosigmoid endometriosis have been well described and include a "mushroom cap" sign,
which is considered a specific finding of solid invasive endometriosis of the rectosigmoid colon on T2-weighted MR images .
The low-signal-intensity base of the mushroom is attributed to hypertrophy and fibrosis of the muscularis propria,
whereas the high-signal-intensity cap represents the mucosa and submucosa,
which are displaced into the bowel lumen [16].
Bladder:Endometriosis of the urinary tract occurs in approximately 20% of cases and the bladder is the organ most frequently affected,
followed by ureters [17].
MR imaging,
solid endometriosis of the bladder appears ,
as infiltrative or nodular lesions with low T2 signal intensity,
centered within the vesicouterine pouch,
and including internal foci with variable T1 and high T2 signal intensity representing ectopic glandular tissue [18].
Round Ligaments:The prevalence of disease in the intrapelvic segment of the round ligament:was 15%.
Similar to solid endometriosis located elsewhere,
a mass involving the round ligament is depicted as T2-hypointense thickening or nodularity with enhancement on contrast-enhanced T1-weighted MR images [20].
Others location of endometriosis:Virtual space located between the posterior wall of the cervix-vagina and anterior rectal wall,
including the rectovaginal septum,
uterine torus,
pouch of Douglas.
4.
EXTRAPERITONEAL ENDOMETRIOSIS:
Corresponds to all implants located outside the peritoneal cavity.
Implants have been described in the thoracic cavity; the abdominal and pelvic walls.The abdominal wall is the most common site of extraperitoneal endometriosis.
The majority of implants are located near scars of previous cesarean sections .Detection of ectopic endometrial glands should help establish the diagnosis of solid endometriosis and exclude the diagnosis of a desmoid tumor [21].