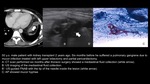
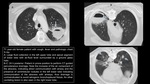
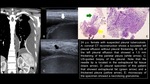
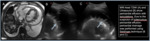
Bacterial infections
- FNAB can change treatment plan in cases of non-responsive pulmonary infections
- Determination of fungal or bacterial DNA/RNA in the sample obtained by percutaneous FNAB can be helpful in immunocompromised patients
Fig. 1 Fig. 2
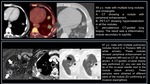
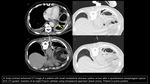
Nodular lung infections
- In some cases,
pulmonary infections can manifest as solitary or multiple nodules
- Percutaneous image-guided biopsy can be helpful in these cases
- It is indicated to perform more than one sample to increase the accuracy of the procedure
Fig. 3
Pyogenic pulmonary abscess
- In the modern medical era is a less frequent entity and most cases are successfully treated with antibiotics.
- When resistant to conservative treatment surgical resection was the primary election.
- Percutaneous transthoracic tube drainage became the treatment of choice in cases of conservative treatment failure.
- Success rate above 83.9%.
- Complication rate 16,1 %
- Mortality rate: 4%.
Less than with surgical treatment.
- Previously rule out central endobronchial obstructive tumour (bronchoscopy should be performed)
Drainage
- Size itself: greater than 4 cm,
- Ineffective antibiotic therapy (after 10-14 days),
- No delay in debilitated patients with poorly effective cough (e.g.
in intensive care setting) – mechanical ventilation is not a contraindication
- It is important to distinguish between lung abscess and necrotizing pneumonia,
as the drainage of a pneumonia could lead to a bronchopleural fistula
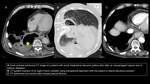
Drainage technique
- US or CT guidance with Seldinger technique
- Puncture of normal lung should be avoided if possible
- Tube size: 6-12 F (optimal: 8F)
- After catheter placement and fluid evacuation,
irrigation with normal saline until fluid clearance and periodic irrigation with saline (5-15 ml) should be performed daily
- The effectiveness of intracavitary fibrinolytic agents in context of pulmonary abscess has not been confirmed yet.
- Single percutaneous aspiration and cultures of abscess content can be diagnostic and informative.
Fig. 4 , Fig. 5
Removal:
- Reduction in abscess size with cessation of purulent drainage for at least 3 days
- Absence of clinical signs of sepsis
Complications and their management:
- Clogging of the catheter – catheter exchange
- Pneumothorax – chest tube insertion
- Haemoptysis / haemothorax – embolization
- Bronchopleural fistula – bronchoscopy / surgery after resolution of the infection (avoid the drainage of necrotizing pneumonia or rapidly increasing air component)
Fig. 6
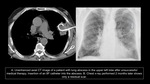
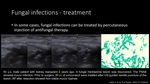
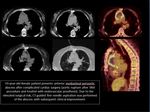
Fungal infections
- During the post-chemotherapeutic aplastic period of hematologic malignancies
- After bone marrow or solid organ transplants
- Cultures results are often negative or late
- BAL (bronchoalveolar lavage) sensitivity to detect aspergillosis is 50%
The role is to:
- confirm fungal infection
- differentiate between Aspergillus spp.
and Mucorales
- rule out other aetiology (tuberculosis,
septic emboli,
primary tumour…)
Prior to biopsy a high resolution CT should be performed in order to
- detect findings of probable fungal infection
- locate target lesion for percutaneous biopsy
- guide fibroscopy and transbronchial biopsy in case of central lesions
- detect GGO consolidations – higher sensitivity of BAL
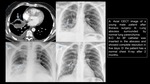
Fungal infections – Biopsy
Indication:
- Prolonged febrile neutropenia with negative BAL and cultures
- No response to antifungal therapy
Sensitivity of FNAB or lung biopsy: 70,6% with 100% PPV.
Technique:
- Biopsy needle of 18 G if possible to obtain sufficient material
- Obtain at least 3 samples (culture,
specific histological study of fungal infection and general HE stain)
– fresh sample in dry tube for culture
– fixed in 10% formaldehyde for histological and immunhistochemical study
- Fixed in AFA for HES stain to rule out lesion of other aetiology.
Complications of FNAB of fungal infections
- Pneumothorax: 17-60%,
0,5-5 % require thoracic drain insertion: ↑number of passes through the pleural cavity
- Bleeding: 5,3 – 30 %,
haemoptysis:1,25-5%,
to minimize risk:
– correct INR if exceeds 1,5 (0,8-1,2)
– correct platelet level with transfusion below 50 000/microl
– suspend acetylsalicylic acid and clopidogrel 5 days before intervention if possible
– stop LMWH 24h before intervention
Fig. 2 , Fig. 7
Pleural infections
- Pleural infections are increasing despite of modern medical therapy
- Increased morbidity and mortality associated with pulmonary infections
- Sampling of parapneumonic effusion with thickness greater than 10 mm (20 mm) is recommended
- Chest X-Ray may miss 10 % of effusions with recommendation of sampling
- Fluid pH can vary in cases of loculated effusions
Fig. 8
Indication
|
Pleural space anatomy
|
|
Pleural fluid bacteriology
|
|
Pleural fluid chemistry
|
Category
|
Risk of
poor
outcome
|
Drainage
|
|
A0: Minimal,
free-flowing effusion (<10 mm on lateral decubitus)
|
and
|
Bx: culture Gram stain results unknown
|
and
|
Cx: pH unknown
|
1
|
Very low
|
NO
|
|
A1:Small to moderate free-flowing effusion (>10 mm and < one-half hemithorax)
|
and
|
B0: negative culture and Gram stain
|
and
|
C0: pH ≥ 7.20
|
2
|
Low
|
NO
|
|
A2: Large,
free-flowing effusion (≥ one-half hemithorax),
loculated effusion,
or effusion with thickened parietal pleura
|
or
|
B1: positive culture and Gram stain
|
or
|
C1: pH < 7.20
|
3
|
Moderate
|
YES
|
| |
|
B2: pus
|
|
|
4
|
High
|
YES
|
Fig. 9
Fig. 10
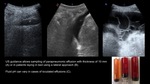
- If possible,
initial thoracentesis should be therapeutic as well.•Always image guided drainage: CT or US? •US guidance permits comparison with initial findings and evaluate prognosis according to US appearance:
- Anechoic: success rate (92,3 %),
Exudative stage
- Complex non-septated: (80-81,54%),
Probably exudative stage
- Complex septated: (50,6- 62,5%) fibrinopurulent (fibrinous adhesions and septae)
- organizational stages (fibrin clots,
multiple septations with thick pleural peel): higher ICU admission rate and increased mortality rate
- Drainage is recommended before worsening of US findings.
Fig. 11
Small bore tube (6-14 F) or Large ( >20 F)?
- Small tubes (SBCT) are as effective as large ones with the exception of acute haemothorax (or complex empyema)
- Less complication rate with SBCT
- Insert multiple tubes in loculated pleural effusion
- Always with image guidance to avoid malposition (preferably US)
- Point of insertion should be anterior to the anterior superior iliac spine line
- LBCT in the fifth intercostal space mid axillary line with tube thoracostomy
- SBCT typically in second intercostal space along the anterior axillary line,
especially in pneumothorax
- Place tube in dependent position for fluid drainage
Intrapleural fibrinolytic agents:
- The aim is to improve the drainage of loculated pleural effusions based on observational studies.
- Not recommended for all patients,
needs to be studied in larger series.
- Various options: Urokinase,
t-PA (tissue plasminogen activator),
DNase,
streptokinase
- Recent trial shows effectivity of the use of intrapleural t-PA in combination with DNase (x3 daily) but not alone:
- improves drainage with reduction of hospital stay and minor surgical rate.
Pleural biopsy
- Specially indicated in suspected pleural tuberculosis
- Definite diagnosis of pleural tuberculosis depends on the demonstration of Mycobacterium tuberculosis in the sputum,
pleural fluid,
or pleural biopsy specimens.
- Image-guided pleural needle biopsy can be used as the primary method of diagnosis in patients with pleural thickening.
Fig. 12
Fig. 13
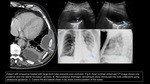
Mediastinal infection
- Head and neck descendent infections,
trauma,
foreign body,
pancreatic pseudocyst,
and post-operative abscess (gastro-oesophageal anastomotic leaks,
cardiac surgery,
thoracotomy…)
- High rate of morbidity and mortality (20-40%),
risk of re-operation
- Few cases published,
no clear guidelines for heterogeneous patient group and aetiology
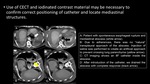
- CT guided drainage can be vital in cases of abscess formation to avoid re-operation due to its high mortality
- Patient positioning and route planning prior to intervention is essential.
If there is no pathway without passing through pulmonary parenchyma,
artificial hydrothorax or pneumothorax can be useful.
- Seldinger-technique,
tandem trocar technique,
fluoroscopically- guided tube drainage of the abscess
Fig. 14 , Fig. 15 , Fig. 16 Fig. 19
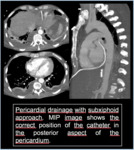
Pericardial drainage
- Only with image guidance (pericardiocentesis or tube pericardiostomy)
- Indication:
- Purulent effusion
- Tuberculosis
Approach according to the distribution of pericardial effusion:
- Anterior
- Subxyphoid
- Parasternal
- Left lateral
Complications:
- Arrhythmias: need for patient monitoring and catheter removal
- Pneumothorax / pneumomediastinum
- Atrial and ventricular wall puncture ∗
- Epicardial laceration∗
- Coronary artery injury∗
∗minimize risk with continuous image guidance
Fig. 17 , Fig. 18