Technically,
CT angiography for TAVI planning must be carried out using a CT multidetector device (CTMD) with at least 64 detectors,
a minimum spatial resolution between 0.6 and 0.5 mm and a dedicated workstation.
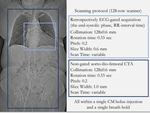
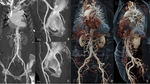
The scanning protocol is based on two acquisitions:
- a retrospectively "ECG-gated" acquisition in meso/tele-systolic cardiac phase,
focused on studying the aortic annulus and the aortic root;
- a second acquisition,
performed without cardio-synchronization,
aimed to evaluate the thoraco-abdominal aorta,
from the pulmonary apexes to the femoral bifurcations (Figure 1).
A single bolus injection of iodinated contrast medium and single breath-hold is necessary and sufficient for both acquisitions [4].
Meso-systolic acquisition (20-40%) is one of the crucial elements of this protocol: in this phase of the cardiac cycle it is possible to acquire images representative of the highest tension exerted on the aortic bulb walls,
but also representative of the highest pressure and volumetric stress on left ventricular outflow tract (LVOT).
This phase corresponds to the moment of the cardiac cycle when the prosthesis,
once implanted,
will be subjected to the greatest stress and when greater efficiency,
effectiveness and durability will be required [5-7].
Premedication with β-blockers is not necessary in these patients in order to avoid any type of hemodynamic complication related to the negative inotropic action of these drugs: in severe aortic stenosis,
the cardiac outflow is chronically reduced due to the reduced residual aortic valve area; a reduction in cardiac contractility would favor an important decrease of the cardiac outflow,
which could result in severe symptoms of hypoperfusion of the arterial intracranial district.
[8]
The contrast medium infusion protocol,
which establishes a variable CM dose between 80 and 120 ml with a concentration of 400 mg/ml,
provides the detection of antecubital venous access on the arm (the right one is preferred to avoid hardening beam artifacts at the level of the aortic arch); the needle used must have a diameter of 18-20 Gauge at least in order to support an infusion flow of 5 ml/sec (considered the gold standard in CT angiographic studies).
The injection of the contrast medium is preceded and followed by a single bolus of 20 ml saline solution at 5 ml/sec.
Before the scan,
the ROI (Region Of Interest) is positioned in the descending thoracic aorta,
precisely at the middle third,
with a minimum threshold value of 140 HU (Hounsfield Unit),
calculated using the semi-automatic bolus tracking technique [9].
After images acquisition,
according to the established protocols,
MPR (Multi-Planar Reformation) reconstructions in the axial,
coronal and sagittal planes can be performed to evaluate the necessary measurements for a correct choice of the device that has to be implanted.
These measures are:
- Perimeter and area of the aortic annulus;
- Minimum and maximum diameter of the aortic annulus;
- Distance between the aortic annulus and coronary ostia;
- Average width of the valvular cusps;
- Minimum and maximum diameters of the sino-tubular junction;
- Minimum and maximum diameters of Left Ventricular Outflow Tract (LVOT);
- Aorto-ventricular angle.
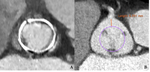
A fundamental and preliminary element in this evaluation is the identification of the so-called Virtual Basal Ring (VBR),
one of the main prosthesis anchorage sites during implantation.
It corresponds to the narrowest point of the aortic root and it is defined by three anatomical anchor points corresponding to the lower portion of every aortic valve leaflet [10,
11].
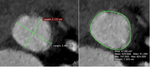
Once the VBR has been identified,
the perimeter,
area and transverse diameters of the aortic annulus are assessed (Figure 2).
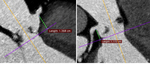
To establish the prosthesis extension in the aortic root,
it is important to evaluate the distance between the VBR and the inferior wall of both coronary ostia (Figure 3); if the origin of one coronary artery at least is excessively low (< 8 mm between VBR and coronary artery) it may represent an important risk factor or even an absolute contraindication to the procedure for potential coronary occlusion.
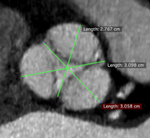
Equal importance is given to the transverse diameters measured at the point of maximum width of the valvular cusps; each diameter is calculated by tracing a segment passing through two reference points: one is the point of maximum width of the cusp and the other one is the opposite valve commissure.
It is useful,
for the prosthetic choice,
to obtain an arithmetic average value of these three diameters: the result will correspond approximately to the prosthesis diameter that will be implanted (Figure 4).
A non-secondary element is to estimate the presence and the grade of calcifications which could eventually affect the cusps; a semi-quantitative classification of the aortic valve has been introduced [12]:
- Grade 1: no calcifications;
- Grade 2: mildly calcified,
represented by isolated calcified areas;
- Grade 3: moderately calcified,
represented by large and multiple calcification areas;
- Grade 4: heavily calcified,
represented by extensive calcifications involving all three valve cusps (Figure 5).
The assessment of the transverse diameters at the level of the sino-tubular junction is also an important element: it constitutes another anchor point of the valvular prosthesis.
The study proceeds with the LVOT estimation,
assessing the minimum and maximum diameter,
about 4 mm below the VBR,
and the semiquantitative evaluation of the calcifications [13,
14].
Based on the presence,
quantity and extension of calcifications,
we can distinguish [12]:
- Mild calcifications,
when there is only one calcification extended longitudinally < 5 mm and that occupies < 10% of the perimeter of the LVOT;
- Moderate calcifications,
when there are at least two calcifications or only one calcification extended longitudinally > 5 mm but < 10 mm and that occupies > 10% of the perimeter of the LVOT;
- Severe calcifications,
if there are multiple calcific nodules or a single calcification extended longitudinally > 10 mm and that occupies > 20% of the LVOT perimeter.
Finally,
it is important to assess the aorto-ventricular angle: it constitutes approximately the angle of angiographic projection which has to be used during the procedure for the positioning of the prosthesis in the most correct and accurate way [13].
The TAVI procedure can be performed in patients already treated with surgical aortic valve replacement (defined as the Valve-in-Valve procedure,
ViV) that shows prosthetic dysfunction and the subsequent recurrence of clinical symptoms [15].
The main problem related to ViV is the risk of coronary occlusion: it could occur due to the prosthetic valvular flaps that obstruct coronary ostia,
increasing dramatically the risk of mortality [16].
From the point of view of the pre-procedural planning,
it is necessary to assess if the ViV procedure will be performed on a stented or stentless prosthetic valve (Figure 6).
In the case of a stented prosthesis,
the points to assess the VBR plane will be the stent brackets; in the case of a stentless prosthesis,
it is necessary to identify the heights of the coronary arteries and the transverse dimensions of the Valsalva sinuses.
When the coronary ostia are above the reference points,
there is no risk of occlusion,
but if they are located below them,
then it will be necessary to derive the minimum distance between the coronary ostium and the VBR,
the so-called VTC (Virtual Transcatheter valve to Coronary ostium distance).
Scientific evidence has shown:
- low risk of coronary occlusion with a distance > 6 mm;
- a moderate risk of coronary occlusion with a distance between 6 mm and 3 mm;
- a high risk of coronary occlusion with a distance < 3 mm [14,
17-19].
Concerning the study of the peripheral vascular district,
it is important to evaluate the thoraco-abdominal aorta,
in terms of size and distribution of parietal lesions,
and the assessment of the main peripheral arterial vessels,
in particular the common and external iliac arteries and the common femoral arteries (figure 7).
It is necessary to evaluate the minimum diameters of these vessels and the distribution of possible calcifications must be provided,
as well as the projective reference plane of the femoral bifurcations in respect to the femoral heads,
useful for transfemoral puncture under fluoroscopy [4].