Keywords:
Tissue characterisation, Comparative studies, Ultrasound, MR, Musculoskeletal soft tissue
Authors:
E. cannizzaro, F. Bruno, C. Gianneramo, S. Iafrate, F. Arrigoni, S. Mariani, L. Zugaro, A. Barile, C. Masciocchi; L'aquila/IT
DOI:
10.26044/ecr2019/C-3189
Methods and materials
We evaluated 17 patients (9 males,
8 females,
mean age 34.6 years,
range 26-52) with clinical and instrumental (US/MRI) evidence of degenerative tendon disease: 8 patients with Achilles tendinopathy and 9 patients with sopraspinatus tendinopathy.
Patients with recent trauma or previous surgery were excluded.
All patients were submitted to 3T MRI examination using standard morphological and T2 mapping sequences,
and ultrasound examination using compression elastography.
For T2 mapping evaluation,
we used a multiecho sequence.
Using a dedicated software, T2 color-scale rapresentation for qualitative analysis was generated.Elastosonography was performed by applying light repetitive compression with the hand-held transducer over the area of interest (three compression-relaxation cycles in each planes).
During the compressions,
the B-mode and the elastogram were displayed side-by-side on the screen.
This compressions generate a change in the structural shape of tendon that the probe detects as elastographics information.
The relative stiffness of the tissues is indicated by a colour code with a range from soft to stiff.
Manual segmentation of tendons was performed either on MR images and in US examinations in order to divide tendons into clinically relevant subregions.
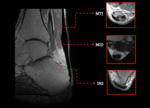
Achilles tendon was divided in to 3 subregions: insertional (INS),
midportion (MID),
and musculotendinous junction (MTJ) (Fig.5).
All regions were evaluated in the axial plane for MRI evaluation and short axis view for sonoelastography.
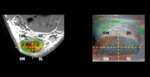
Every subregion was furtherly divided into 4 anatomic sides: superficial medial,
superficial lateral,
deep medial,
deep lateral side (Fig.6).
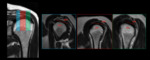
Sovraspinatus tendon was divided in to 3 clinically subregions:insertional(INS),preinsertional/creascent area ,and musculotendinous junction (MTJ).
All regions were evaluated in the coronal and sagital plane for MRI evaluation and short and long axis view for sonoelastography.
Every subregion was furtherly divided into 2 anatomic sides: bursal side and articular side (Fig.7).
Two musculoskeletal radiologists independently reviewed each examination in order to assess the degree and the localization of tendinosis on the basis of the qualitative colorimetric maps of T2 mapping and sonoelastography and were repeated after a minimum of four weeks interval to assess intra-rater and inter-rater reliability.
To assess the degree of degenerative involvement,
each reader assigned a tendinopathy score (normal,
mild,
moderate,
severe),
on the basis of a qualitative assessment of color maps from T2 mapping and sonoelastography.
Intra- and interobserver measurement reliability were assessed using k Cohen coefficient.
The k values were interpreted as follows: k <0.20 was defined as poor agreement; 0.21- 0.40= fair agreement,
k 0.41-0.60=moderate agreement,
k 0.61-0.80=good agreement,
k 0.81-1=excellent agreement.