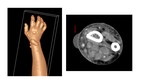
Soft-tissue infections are frequent in clinical practice,
among which stand a less frequent subtype,
the necrotizing soft tissue infections.
These affect superficial,
deep tissues and adjacent fascias,
and are characterized by rapid progression,
tissue destruction and signs of systemic toxicity.
Early recognition remains one of the most important prognostic factors; nevertheless,
this disease is frequently misdiagnosed in initial stages as clinical manifestation is not usually straightforward,
therefore imaging plays an important role in achieving a prompt diagnosis.
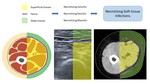
Anatomy
The most superficial structures of the soft-tissues are the skin layers of epidermis and dermis,
which are not visible with imaging.
Below them is the hypodermis or subcutaneous tissue,
and deeper the fascia.
Terminology at this level may be confusing [1].
Classically anatomists delimitate a superficial fascia embedded in the subcutaneous cellular tissue and then a deep,
thicker fibrous fascia.
It spreads fibers of connective tissue between muscles,
delimiting the so-called intermuscular septa.
On the other side,
for some surgeons the term “superficial” fascia refers to deep fascia described by anatomist, therefore it is convenient to discuss with the referring physician the proper terminology to avoid mistakes.
Finally,
in the deepest layer are located the muscles and the bones. Fig. 1
Depending on the layer affected,
there are several pathologies among the necrotizing infections spectrum.
Taking into account the aggressivity of these entities,
their close relationship and the similar etiopathology that makes them often coexist and be managed similarly,
the term “Necrotizing Soft-tissue Infections” was coined to group them. Fig. 2
Necrotizing fasciitis
The necrotizing fasciitis (NF) remains one of the most recognized pathologies among necrotizing infections,
describing a process which primarily affects and spreads through the deep fascia,
as well as the adjacent tissues,
with necrosis.
Infection typically begins in the superficial fascial planes,
and then rapidly progresses into the deep fascial layers.
Typically shows rapid and aggressive evolution: the overall morbidity and mortality rate is 70-80% [2].
These values have been corroborated in our hospital center over the last two years,
evaluating the totality of the cases diagnosed of NF,
with a mortality rate of 75% (9/12),
caused directly by the infection or indirectly due to complications derived from it.
There are no true risk factors for NF,
as it affects healthy patients or with known chronic comorbidities.
However,
there are associations between its development and conditions related to the breakage of skin layers:
-Trauma,
intravenous drugs use.
-Recent surgery (within the past 90 days) at the affected site.
Classification:
Two main types are distinguished according to their etiology,
nevertheless they cannot be differentiated with imaging:
-Type 1 (70-80%) Polymicrobial.
Located more frequently in trunk and perineum.
-Type 2 (20-30%) Monomicrobial.
Extremities.
It can affect any part of the body,
being the trunk and the inferior limbs the more frequently involved regions,
due to a natural lack of fibrous boundaries between subcutaneous tissues and fascia that enables widespread infection.
There are two specific subtypes with their own characteristics and prognosis based on the location: Ludwig angina for the submandibular region or Fournier gangrene for the perineum,
which have not been included in our revision.
Clinical manifestations:
Diagnosis depends strongly on clinical suspicion,
which is challenging since NF presents with non-specific symptoms and signs in early disease stages:
Initially,
the overlying tissue and skin may appear unaffected or with low involvement,
with erythema,
edema,
swelling,
and pain,
which may be minimal relative to systemic findings.
This fact explains why the majority of cases are initially misdiagnosed.
Lately,
other “red flag” clinical findings more representative of NF are developed,
which must alert of its progression.
The “red flags” are pain out of proportion to the degree of skin involvement,
crepitus,
vesicles,
bullae,
necrosis and toxic shock-like symptoms.
Fig. 3
Diagnosis is mainly clinical,
supported in selected cases by imaging tests and being confirmed via surgical exploration of the soft-tissues in the operating room.
Prognosis:
The most important predictor of mortality is a delay in diagnosis.
Considering the lack of specificity and sensitivity of clinical and laboratory findings,
imaging becomes crucial to reach the diagnosis and determine the extension.

![Fig. 1: Different anatomy terminology of the fascia. References: own edition, based on [4]](https://epos.myesr.org/posterimage/esr/ecr2019/149706/media/829770?maxheight=150&maxwidth=150)