Neurobehçet disease (NBD) could be categorized into three main categories; parenchymal,
extraparenchymal and mixed parenchymal and non-parenchymal disease.
Atypical parenchymal CNS involvement forms are also reported.
Parenchymal NBD:
it is the most common form of CNS involvement in NBD in adults,also known as the intra- axial NBD,
it represents an inflammatory meningo-encephalitic process,
that usually involves the telencephalic-diencephalic junction,
brain stem and spinal cord.
These patients present with a subacute (or rarely acute) onset of severe headache,
dysarthria,
hemiparesis,
ataxia and cranial nerve palsy.
The acute form is mainly characterized by acute meningo encephalitis with or without focal lesions.
The progressive form consists of slowly progressive neuro behavioral changes such as dysarthria and ataxia.
Acute form seems to have a good response to corticosteroids treatment.
The chronic progressive form is characterized by a poor response to conventional treatment.
Non- parenchymal NBD:
It is also called vascular or extra-axial NBS occurring in up to 20% of patients with NBD.
It occurs due to vascular involvement such as dural sinus thrombosis,
the prominent clinical feature is severe headache which is usually progressive over weeks,
papilledema and sixth nerve palsy are occasionally observed.
This form occurs more commonly in the pediatric population.
The most commonly affected sinuses are the superior and sagittal sinuses.
Diagnosis of neuro-behcet’s disease:
Owing to difficulty in obtaining histopathological studies in such cases,
the diagnosis mainly depends on:
- Clinical presentation.
- CSF analysis.
- MRI findings.
International consensus recommendation criteria for neuro-Behçet’s syndrome diagnosis:
Definite NBS:
Occurrence of neurological symptoms and signs in a patient who fulfills the International Diagnostic Criteria for BS,
these symptoms cannot be explained by any other known systemic or neurological disease or treatment,
with objective abnormalities consistent with NBS are detected either on neurological examination,
neuroimaging studies (MRI),
or abnormal cerebrospinal fluid (CSF) examination.
Probable NBS:
Meeting one of the following two criteria in absence of a better explanation for the neurological findings: a) Neurological syndrome as in definite NBS,
with systemic BD features but not fullfilling the International Diagnostic Criteria for BS; b) A non-characteristic neurological syndrome occurring in the context of International Diagnostic Criteria supported BD.
Radiological MR features:
MRI is the gold-standard neuroimaging tool for the diagnosis of NBS.
Parenchymal- NBD:
·Parenchymal CNS involvement may present as an acute disease or may have a chronic progressive form.
·Parenchymal form may occur with or without meningeal inflammation.
lesions are generally located within the brainstem,
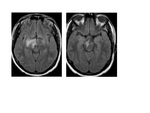
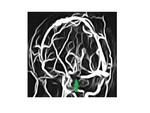
occasionally extending to the diencephalon Fig. 1 ,
and less often are within the periventricular and subcortical white matter.
·MR findings in NBD are usually foci of hyperintense T2 SI on T2 weighted images,
yet they may be of large or even confluent,
the lesions may be circular,
linear,
crescent-shaped,
or irregular.
- Acute or subacute lesions:
- T1 weighted images: lesions are hypointense to isointense,
commonly show heterogeneous enhancement with contrast-enhanced T1-weighted images.
- T2-weighted images: scattered areas of high signal intensity mostly affecting the central structures of the cerebrum,
the cerebral peduncles,
and basilar part of the pons,
these lesions are also hyperintense on fluid-attenuated inversion recovery images Fig. 1.
- Aseptic meningitis is one of the uncommon manifestations of Behçet disease,
with meningeal thickening with enhancement.
- During the recovery phase: few months after the acute attack,
small scattered lesions with high signal intensity in white matter have been reported,
either in periventricular areas or apart from the ventricles.
- In the chronic phase,
smaller lesions might be seen,
usually isointense and non-enhancing,
but might resolve completely.
Nonspecific white matter lesions can be seen,
unlike the acute phase in which solitary lesions are more common,
widespread involvement in the chronic phase is more common with the presence of atrophy of posterior fossa structures and brain stem particularly the midbrain tegmentum and pons with decreased signal intensity and enlargement of the third ventricle.
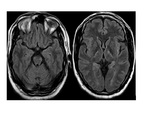
- Follow up MRI may show changes in size,
shape,
or location of involvement,
sometimes manifesting a reversible course Fig. 2 .
- Atypical parenchymal involvement:
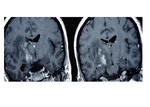
there are number of reported cases in which MRI images have shown mass lesions that mimicked space occupying lesions as brain tumors Fig. 3 and abscesses,
some necessitating histological diagnosis.
Other atypical patterns which may occur with involvement other parenchymal are bilateral cortical–subcortical lesions and Regional or global atrophy.
It is uncommon finding,
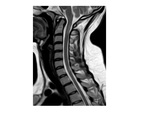
when it occurs it tends to be extensive longitudinally,
the major site of involvement is the cervical spinal cord with the myelitis-like inflammatory lesions continuing for >2 segments and extending to the brainstem in some cases,
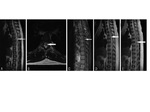
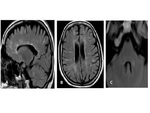
and recently Fig. 4 ,
distinct MRI patterns were identified on T2 weighted images known as Bagel pattern,
which appears a central lesion with hypointense core and hyperintense rim with or without contrast enhancement; and ‘Motor Neuron’ pattern: which is symmetric involvement of the anterior horn cells.
Non- parenchymal forms (extra- axial neuro- behçet):
- Cerebral venous sinuses thrombosis:
It is the second most common form of neurological involvement in NBD,
which may be seen in up to 12–20% of the patients with NBD.
MRI brain: usually reveals occluded dural sinus with otherwise normal parenchymal findings as venous haemorrhagic infarcts are not expected to occur constantly in case of venous sinus thrombosis due to BD,
compared to sinus thrombosis caused by other aetiologies.
But in some cases,
parenchymal lesions occur secondary to the venous thrombosis
MR venography: confirm the diagnosis and reveal the extent of the venous thrombosis.
the superior sagittal sinus is the most common site of thrombosis,
followed by transverse sinuses Fig. 5 ,
deep cerebral veins,
and cavernous sinuses,
respectively.
- Arterial Neuro-Behçet’s Syndrome:
Arterial involvement resulting in CNS vascular disease is rare.
Vessel involvement include: arterial occlusion and arterial aneurysms may be seen.
The incidence of aneurysms formation is rare,
yet the have the tendency towards being multiple,
peripheral and fusiform when they occur.
Arterial involvement affects extra and intra- cranial arteries,
it can affect common carotid,
internal carotid,
anterior and middle cerebral arteries,
superior cerebellar,
anterior communicating,
and vertebral arteries.
Advanced MRI techniques used in Neuro-Behçet’s Syndrome:
MR spectroscopy and diffusion-weighted imaging can detect small changes due to ischemia and/or inflammation; susceptibility weighted image reveal the haemorraghic nature of the lesions.
- Diffusion- weighted imaging and apparent diffusion coefficient (ADC):
Diffusion-weighted imaging may help in differentiating acute,
subacute,
and chronic lesions.
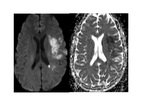
Acute- subacute lesions appear hyper-intense on diffusion-weighted images and show a restricted apparent diffusion coefficient (ADC) on ADC map.
Apparent diffusion coefficient (ADC) values may represent reactive gliosis in chronic disease,
cytotoxic edema following ischemia due to vasculitis in subacute disease Fig. 6 ,
and vasogenic edema in acute disease.
It may be helpful for the assessment of the presence of acute infarction with lactic acid peak,
and nonspecific changes in the ratios and metabolites
Chronic progressive neurobehcet: ADC increase in normal-appearing white matter,
which indicate chronic progressive inflammation,
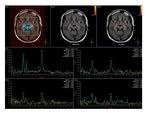
and decreased NAA to creatine (NAA/Cr) ratio in the pons and cerebral white matter in magnetic resonance spectroscopy Fig. 7 ,
which indicate extensive neuronal damage in cerebral white matter.
- Susceptibility- weighted image (SWI):
The number of lesions detected with susceptibility-weighted imaging is larger than the conventional T2* gradient-echo.
Most of the lesions in p-NBS were found to be haemorrhagic.
MR/ CT venography: reveal the evidence of cerebral venous sinus or vein thrombosis in non- parenchymal NBD.
Mimics of Neuro-Behçet’s Syndrome:
MRI is very useful in differentiating NBD from its mimics.
The brainstem–thalamic–basal ganglia (mesocephalo-diancephalic junction) lesions in the MRI with the presence of the matched clinical context can strongly support the diagnosis of acute/subacute parenchymal NBD and can even raise the possibility of the diagnosis when the systemic features of the disease are scarce.
- Multiple sclerosis: Chronic parenchymal NBD lesions are iso-intense,
smaller,
and at times difficult to differentiate from lesions seen in multiple sclerosis.
yet the imaging findings differs between NBS and MS:
(1) Brain stem atrophy in association with subcortical lesions points toward NBD.
In multiple sclerosis; the brainstem lesions are ventrally localized,
in opposition to MS where the floor of the fourth ventricle and the middle cerebellar peduncle are frequently concerned.Cerebellar lesions are uncommon in NBS.
(2) Multiple sclerosis lesions are predominantly periventricular Fig. 8 ,
and juxta- cortical with infrequent involvement of the basal ganglia,
internal capsule,
and the peripheral part of the pons,
while chronic parenchymal NBD lesions are mainly subcortical
(4) Spinal cord involvement in multiple sclerosis rarely extends more than a few vertebral segments Fig. 9 .
- Neuro-Lupus erythematous: we can differentiate between the two entities by the presence of brain stem lesions,
which are rare in case of lupus where the grey matter is more frequently involved and sub-cortical white matter lesions are seen,
another important finding in NBD that help in differentiation is the frequency of the contrast enhancement of the lesions in NBD.
- Neuromyelitis optica: the clinical manifestation of BD eye lesion is very similar to neuromyelitis optica (NMO) in the clinical presentation as both present with decreased visual acuity.
Neuro-Behçet’s disease in children:
It affects about 5%–30% of the children with BD.
It can be the first presentation and also can be the only involvement through the disease course. There are two main manifestations; cerebral vein thrombosis and parenchymal involvement which is usually in the form of meso-diencephalic meningo-encephalitis.
Dural sinus thrombosis is more frequently detected in children whereas,
parenchymal involvement is indeed more common in adults
Dural sinus thrombosis in a child,
should bring BD in mind.
Although less commonly observed in children,
brain stem involvement as meso-diencephalic extension and/or hemorrhagic lesions and/or patchy enhancement should make NBD a strong differential diagnosis.
NBD should also be included in the differential diagnosis of infectious meningo- encephalitis as well as multiple sclerosis,
thrombophilia and other vasculitides due to close imaging patterns.