Phisical principle
US waves are longitudinal mechanical waves which propagate in the medium as alternating zone of compression and rarefaction; thus each wave propagate through the displacement of the single particle in the medium which then return to the equilibrium,
dissipating the wave energy.
US waves can achieve different diagnostic or therapeutic effect depending mainly on different intensity and frequency.
Intensity and frequecy.
Intensity represent the energy of a single wave and it could be expressed as the power delivered per unit area (W/cm2).
Therefore,
the intensity value express the energy focused by the wave on a specific point “x” within the medium,
characterized by a specific depth.
A mathematical correlation exists between US frequency,
penetration depth,
sharpness of the lesion and intensity,
through the expression I=I0e-mx,
I0: intensity of the wave at the origin
m: attenuation value of the medium at x-point.
The mvalue is also a function of frequency through the expression m=afb
“a” and “b”: constant specific for the medium
f: frequency.
The initial equation I=I0e-mxso clearly shows that an absorbing medium,
by which propagate a mechanical wave,
attenuates exponentially the wave itself.
Therefore,
an increasing frequency determines an increasing mvalue,
which means an increasing absorption by the medium; thus,
there is a decrease in depth penetration and a necessity to increase the initial intensity to focused a determining wave intensity on a target point.
Conversely,
a decrease in frequency,
increase the wave penetration,
but with a not-sharply defined thermal focus [1].
Acoustic impedance
Acoustic impedance is given by the product of the medium density and the speed of sound into the medium.
The impedance of two different tissues at the interface predicts the capability of a wave to get through the medium themselves.
The transmission of an acoustic wave is maximized only when the impedance is the same on the both side of interface.
E.g.,
air is characterized by the maximum impedance,
which completely reflects US waves.
Interaction US-wave/energy
Single particles within the medium reacts to the US passage depending on the energy output given by the wave itself.
Indeed,
above a specific threshold,
the single particle is not capable to dissipate the absorbing energy,
which results in energy storage and thus in increasing kinetic energy.
The mechanics involved in transfer of thermal energy are two: 1.
The first is the relaxation absorption due to elastic force between particles,
which return them to the equilibrium position after the displacement; 2.
The second one,
called classical absorption,
due to friction between particles which convert the energy into heat (mainly involved in the FUS treatment).
Application.
FUS therapy generally uses high acoustic intensity.
Currently,
US therapy exploits two different effect; indeed,
US waves,
could determines mechanical/cavitation force or thermal heating.
Cavitation effect results from the capability of US waves to form microbubbles in tissue which violently collapse releasing high energy amount; this focalized energy fragment the tissue ultimately creating a hole.
Mechanical and cavitational tissue effect of US waves are used for extracorporeal shock waves lithotripsy,
with ultrashort pulse (1-2 ms),
high acoustic amplitudes (100MPa) and acoustic intensity exceeding 2000W/cm2.
Thermal heating effect instead,
is mainly a consequence of classical absorption,
as mentioned therefore,
increase of energy storage and friction between particles determine an increase of temperature.
When a value of 56°C is reached for at least one second,
coagulative necrosis occurs due to protein denaturation.
Thermal heating effect is used in the treatment of different tumors as well as in the treatment of essential tremor,
with moderate pressure amplitudes (10MPa),
continuous US waves and Intensity greater then 300W/cm2[2].
Selection criteria
The high efficacy of this technology is strickly related to an accurate selection of the patient and the lesion to treat.
1. Superficial bone lesion and osteolitic lesions.
Bone tissue has an high acoustic impedance and US wave transmission is totally limited by the intact cortex,
with consequent heat accumulation on its surface.
Therefore,
FUS treatment could show an high efficacy only for osteolytic lesion or for bone lesion with a thin sclerotic edge with a cortical or superficial localization.
On the other hand,
a cortical heat accumulation could be exploited to achieve a palliative intention through a periosteal denervation caused by ablative temperatures [3].
2. Skeletal location
The importance of lesion location is well understand by the need of an adequate acoustic window and,
on the other hand,
for the nearness of highly sensitive structure.
E.g.,
epiphyseal lesion showed often limited acoustic windows due to complexity of articular structure; however,
different study has shown the high efficacy and feasibility in the treatment of superficial epiphyseal bone lesion with the respect of cartilaginous or synovial structures and no signs of precocious onset of osteoarthritis [4].
Instead,
for spinal lesion,
HIFU do not find a primary indication for the nearness of spinal cord and spinal root in order to avoid any injurie which could result from an anomalous spread of the US beam.
Moreover,
all highly sensitive structure must be protected from the potential damage due to an erroneous US beam spread,
as also tendon or nerve which could storage thermal energy and be damaged.
It should not be forgotten that transmission of thermic energy could also result for a contiguous transmission or for potential refraction of US waves on perilesional calcification which may form as consequence of the intense inflammatory activity induced by bone lesion.
However,
even the variability of lesion exposure partially could change with the movement of patient or its extremity and with capability to guarantee this “required” position,
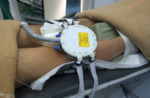
the accessibility of bone lesion has been increased in the last few years thanks also to new HIFU technologies,
which allow rotation and translation of transducers within the electric examination table or also new transducers removable and directly applicable on the treatment site (fig 2).
3. Medium acoustic impedance
An adequate acoustic window is mandatory for the HIFU treatment.
However,
it could be necessary underly that the presence of an high acoustic impedance interface do not represent an absolute contraindication.
Even this asserction could seems obviously,
the suitability of the treatment come through firstly for the confidence of IR with the use of this technology; this certainly emphasize the variability in the definition of the suitability of this procedure,
the complexity of each limit and their specific solution,
and partially explain why the HIFU technique does not find a primary role.
Clinical Results.
MRgFUS can achieve different goals in the treatment of painful bone lesion [5]; indeed,
generally it could be used for a palliative intention or for a curative intention,
depending on how radically can be the thermal ablation and what kind of lesion is treated.
Therefore,
osteolytic lesion mostly treated are benign bone lesion as osteoid osteomas,
osteoblastomas or further symptomatic “do-not touch lesion”,
or malignant lesion as bone metastases.
In the last few years,
since 2012,
we successfully treated 61 patients: 39 osteoid osteomas; 6 intraarticular osteoblastomas; 1 subperiosteal chondroma; 1 chondroblastoma; a GCT recurrence; a symptomatic cortical desmoid; bone cyst; 4 hemangioma; 6 bone metastases (tab 1).
Pain control was obtained in all the bening bone lesions as also in malignant too,
with a fast pain relief (tab 2).
No complication of percutaneous approach were recorded.
Advantage in FUS treatment was also showed by the imaging follow-up,
with a significant bone densification and no pathologic fracture after thermal ablation.
However,
MRgFUS indication widely varied in different painful bone lesion.
Malignant lesion
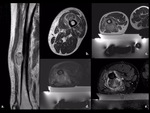
Since the first study by Catale et al [6],
currently MRgFUS has achieved important goal in this field with a comproved efficacy in the pain palliation through both periosteum denervation and direct lesion ablation [7] (fig 3).
In our center we treated 6 bone metastases,
with a complete pain relief in the first week after treatment.
The efficacy of MRgFUS in bone mets pain palliation is comparable to EBRT,
even with a faster pain relief and with the unlimited possibility to repeat the treatment [8].
However,
MRgFUS currently find a limited application in bone mets treatment,
considering: a) the capability of radiofrequency/micro-waves/crio-ablation techniques to achieve excellent results with shorter procedure time; b) possibility to performe consolidation procedure radiofrequency/micro-waves/crio-ablation techniques in the same time of ablation.
Benign lesion
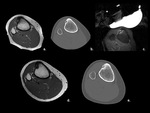
The efficacy of HIFU technique in Osteoid Osteoma ablation is widely described in literature. Even Radiofrequency Ablation (RFA) are still considered the gold standard in the treatment of osteoid osteomas,
the high efficacy of MRgFUS in the treatment of these lesion is widely accepted [9] (fig 4; tab.
3).
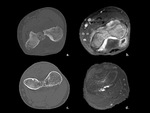
In our center we used to treat also Osteoblastomas,
a bone lesion with histological findings similar to the Osteoid Osteoma,
even it could show a higher biological aggressivity and a tendency in growth (fig.
5).
As shown by our experience,
MRgFUS could be useful also in the treatment of superficial symtomaptic “do not touch lesion” (fig.
6),
pseudotumoral or inflammatory lesion for which no surgical treatment are needed [10].
However,
sometime these lesion could be responsible for severe pain and functional impairment. Indeed,
image guiding treatments are considered of the utmost importance through the well-defined visualization of the lesion,
and therefore by permitting a complete eradication of the painful bone lesion,
which is the cornerstone in the treatment of these lesions.
Conversely,
surgical options are often inadequate due to an high recurrence rate associate with the more conservative approach.
In addition,
high validity of MRgFUS has been shown also in the treatment of intra-articular bening bone lesion,
by sparing sensitive articular structure without precocious onset of osteoarthritis,
as shown in a recent publication from our groups [4].