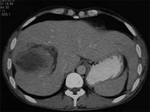
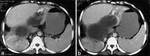
Primarily affects the liver and typically demonstrates characteristic imaging findings.
Imaging findings depend on the stage of cyst growth (unilocular or contains daughter cysts,
partially or is completely calcified).
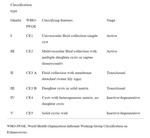
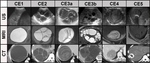
Several classification schemes based on cyst appearance have been proposed.The WHO developed a standardized classification system, originally developed by Gharbi and colleagues in 1981,
was revised by the WHO and is currently the screening method of choice.
( fig.3 and 5)
The diagnostic approach is summarized in figure 4.
Ultrasonography (US) is particularly useful for the detection of cystic membranes,
septa,
and hydatid sand.
Computed tomography (CT) best demonstrates cyst wall calcification and cyst infection.
CT and magnetic resonance (MR) imaging may demonstrate cyst wall defects as well as the passage of contents through a defect.
Chest radiography,
US,
CT,
and MR imaging are all useful in depicting transdiaphragmatic migration of hydatid disease.
CT is the modality of choice in peritoneal seeding.
US and CT demonstrate rupture in most cases that involve wide communication.
Indirect signs of biliary communication include increased echogenicity at US and fluid levels and signal intensity changes at MR imaging.
CT allows precise assessment of osseous lesions,
whereas MR imaging is superior in demonstrating neural involvement.
Familiarity with atypical manifestations of hydatid disease may be helpful in making a prompt,
accurate diagnosis.
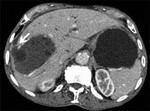
After we know the appearence of HD we need to be aware of the possible intrahepatic complications.
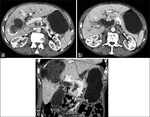
Cyst rupture can be limited and the detached endocyst appears as a floating membrane inside the cyst,
while the defect of the cyst wall can be identified. Or the defect can fistulate ( communicate) into the biliary shaft,
intrahepatic/ subcapsular hepatic,
intraperitoneal (exofitic forms),
abdominal wall,
blood flow ( causing haematogenetic dissemination).
( fig.6,
7,
8)
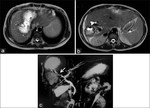
Direct rupture can have important clinical consequences: anaphylaxis,
hydatidic dissemination,
or secondary bacterial infection.
(fig.9)
Infection of hydatid cyst can clinically and radiographically mimick hepatic abscess - defined margins,
perilesional inflammation,
gas or air fluid level.
Compression on hepatic venous structures cand produce thrombosis of portal vein,
hepatic veins or inferior vena cava.
( fig.9)