FINDINGS
The debate about the use of chest radiograph in community acquired-pneumonia (CAP) is still open.
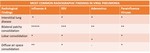
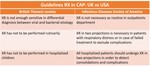
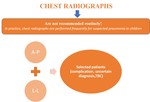
National guidance from the United Kingdom and the United States on community-acquired pneumonia in children (Table 6) states that chest radiographs are not recommended routinely in uncomplicated cases (8).
In practice,
chest radiographs are performed frequently for suspected pneumonia in children (9).
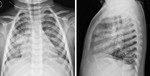
Also the technique is very different (in some hospitals is performed just one projection (anterior-posterior),
in others both (anterior-posterior and lateral).
Also the guide lines are not clear about that: in general we can assert that the second projection should be performed just in selected patients (complication,
uncertain diagnosis,
TBC) (Figure 3,Figure 4).
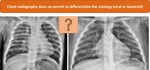
The discrepancy between guide lines and practice occurs mainly because even if the chest radiography doesn't permit to differentiate the etiology (viral or bacterial) (Figure 5) and cannot influence the management and the use of antibiotics.
In particular viral pneumonia can manifest with different aspect on chest radiography (Table 7).
Harris et al.
(10) made the distinction between the developed and developing world regarding the use of chest radiographs in this context,
in that community-acquired pneumonia presenting in the developed world can be verified by the radiologic finding of consolidation while in the developing world there might be difficulties in obtaining a radiograph.
A relative new diagnostic instrument in pulmonary disease in children is ultrasound (Figure 6),
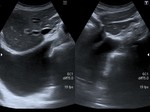
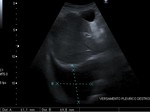
promising especially in detection of pleural effusion and consolidations (Figure 7,
Figure 8).
It has many advantages: is easy,
rapid,
portable and repeatable and his non-ionizing property is especially important in children.
Recent studies refer that ultrasound can be considered to be performed first before radiography in children with suspected CAP,
because it has shown high accuracy and repeatability to diagnose CAP; the routine use of ultrasound for children with suspected CAP can reduce the exposure of radiation to meet the recommendations of the International Atomic Energy Agency (11).
However,
the methods used to perform LUS in children are not precisely standardized,
and the diagnosis of interstitial CAP is inaccurate; further studies are needed before LUS can be routinely used in everyday paediatric practice (12).
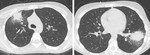
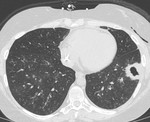
CT should be performed every time a complication is suspected (Figure 9).
It is not currently a first-line imaging tool for children with suspected uncomplicated community-acquired pneumonia and is largely reserved for when complications of pneumonia are suspected or there is difficulty in differentiating pneumonia from other pathology (13) (Figure 10,
Figure 11).
In recent years there was a widespread use of chest CT,
there is a lack standardisation of CT protocols between centre.
Fortunately,
over recent decades,
technical innovations in CT scanner technology and image reconstruction have resulted in a substantial reduction in the radiation dose (14).
Other innovating factors favorable to the diffusion of CT in children were: a powerful postprocessing techniques; a grater awarness on the possible risks related to radiation,
as well as the perception of these risks,
that allowed a better balance of risk and benefit; the development of very fast CT scanners without the need for anaesthesia or sedation.
As a result of these innovations,
chest CT can now be used more safely in children.
CT needs to be performed at acceptable radiation doses in children and is indicated for diagnosing complications associated with pneumonia,
when patients fail to respond to treatment,
when chest radiographs are suggestive,
when empyema is diagnosed on US and in environments where HIV and tuberculosis are likely coinfections.
Even though US is adequate for demonstrating and evaluating effusions,
CT is important for demonstrating the underlying lung in search of associated necrosis or abscess formation.
CT is superior to chest radiographs and the relatively low theoretical cancer risks need to be appropriately considered against the many advantages it affords the clinician,
so as not to deny children the benefits of rapid and accurate diagnosis (13).
Protocols recommended in the literature vary,
but most utilize fast sequences to obtain single or multiple breath-hold imaging without cardiac or respiratory triggering (15,16).
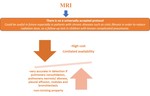
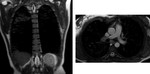
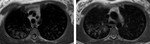
The use of MRI (Figura 12) in CAP is still challanging and there is no a universally accepted protocol.
Several recent studies have shown that lung MRI has a high diagnostic accuracy compared to CT and radiographs,
by the way the field where it has been the greater application still remains the cistic fibrosis (Figure 13,
Figure 14).
In current practice,
MRI is infrequently performed for evaluating pneumonia.
Though CT remains the gold standard,
several studies have shown MRI to be accurate and sensitive for most findings in pneumonia; particularly in children,
in whom there is a greater concern about the effects of ionizing radiation,
MRI should be considered as a viable alternative to CT for the evaluation of pneumonia and its complications (17).
High cost and limitated availability are the main disadvantages and XR still remain the first choice.
first-line imaging test.The value of MRI is its potential to replace CT for evaluating pneumonia and its complications (17).
In particular it is very accurate in detection if pulmonary consolidation,
pulmonary necrosis/ abscess,
pleural effusion and it seems to show a good sensitive in diagnosis of nodules and bronchiectasis.
Pleural changes were easily identified and loculation of pleural fluid was detected (18) and could be useful in future especially in patients with chronic diseases such as cistic fibrosis in order to reduce radiation dose,
as a follow-up test in children with known complicated pneumonia.
Novel chest CT,
MRI and image analysis techniques will improve our understanding of the pathophysiology and treatment of lung diseases in the paediatric population; although,
initially,
many of the developments were primarily focused on cistic fibrosis,
they are now being applied to other diseases such as bronchopulmonary dysplasia,
bronchiectasis,
interstitial lung diseases,
pneumonia,
primary ciliary dyskinesia,
sarcoidosis,
tuberculosis and congenital lung abnormalities (2).