How to identify the patient at risk? Are there any measures to decrease the possibility of adverse reactions in these patients? If so,
which ones?
Identification of patients at risk of immediate hypersensitivity reactions
The incidence of adverse reactions,
especially those of immediate hypersensitivity,
is rather low; with the non-ionic iodinated contrast media the estimated frequency is between 0.2-0.7%; for Gadolinium-based contrast agents the incidence of hypersensitivity reactions is even lower,
around 0.04-0.67%.
[5]
The identification of patients at risk of adverse reaction is a fundamental step to allow the execution of the examinatio safely; although the majority of hypersensitivity reactions occur unexpectedly,
there are some conditions that are classically considered "at risk" for the development of adverse reactions.
In this context,
the Italian Society of Medical and Interventional Radiology (SIRMI) has recently made a statement,
clarifying those that should be univocally considered risk factors for hypersensitivity reactions:
• Prior reaction from hypersensitivity to a class of contrast media (Iodates or Gadolinium-based)
• Bronchial asthma or angioedema not controlled by medical therapy
• Pre-episode of idiopathic anaphylaxis
• Mastocytosis
In particular,
it has been clarified how food allergies and allergies to other classes of drugs are not considered risk factors for the development of hypersensitivity to contrast media.
[5,6] (Table 5) [6]
Prevention of hypersensitivity reactions
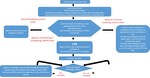
The presence of even just one of the above conditions makes the procedure "at risk of adverse reaction": in this case the radiologist has the duty,
where possible,
to use other diagnostic means to answer the clinical question or to direct the patient to an allergy assessment course before the examination. (Fig.
1)
In the case of an emergency procedure,
the radiologist,
after identifying the patient at risk,
can put in place some useful strategies to reduce the risk of adverse reaction.
(Fig.
2)
Regarding Premedication,
its effectiveness in reducing hypersensitivity reactions to contrast medium remains a controversial topic.
The indications provided by SIRMI itself are to be considered of low scientific evidence since- actually -there are no randomized studies on the reliability of this practice in reducing the risk of adverse reaction.
Finally,
it must be remembered how the multidisciplinary collaboration,
in this case,
is fundamental; in case of "high risk" exams,
it is recommended to alert in advance the Anesthesia and Reanimation unit or,
preferably,
to perform the examination in the presence of an experienced resuscitator.
[6]
Prevention of late reactions
The non-renal delayed reactions to iodinated contrast media are substantially attributable to mechanisms similar to immediate reactions but characterized by a higher latency in relation to biological mechanisms of delayed hypersensitivity; in this case,
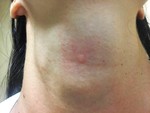
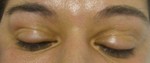
the most frequently affected organ is the skin (rash,
maculopapular,
tumefaction,
itch).
For such delayed manifestations a different and non-cross-reactive contrast agent with the one that caused the first episode must be used - but no premedication is generally recommended.
(Table 6)
No delayed-hypersensitivity reaction phenomenon has been currently described for the Gadolinium-based contrast media.
[6]
Prevention of Ultratardive reactions
For iodinated contrast agents,
the major ultra-late extra-renal adverse event is thyrotoxicosis secondary to the iodic load introduced during the examination.
(Table 7)
To this day,
the main group at risk is represented by patients with Graves' disease not controlled by medical therapy; in such patients an endocrinological evaluation both before and possibly at a distance from the examination is recommended,
if an alternative test is not available.
It is worthy of mention Nephrogenic Systemic Fibrosis,
a serious adverse event due to the lack of renal clearance of gadolinium-based contrast agents.
The onset of this condition can occur from a few days to years after administration,
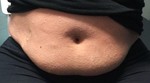
with cutaneous onset (pain,
swelling,
erythema,
thickening of the skin,
often in the lower limbs) and systemic diffusion that can lead to death.
Patients that can be considered at risk for this condition are:
• Chronic kidney disease (CKD) grade IV and V (GFR <30 ml / min)
• Dialysis
• Acute renal failure
The prevention of this condition is based on the careful selection of the patient and the contrast medium,
keeping in mind the risk conditions where the administration must be at the lowest possible dose and the high risk conditions where the administration should be avoided.
(Table 8) [7]
Prevention of renal adverse reactions
The identification of patients at risk of such manifestations is based,
above all,
on the evaluation of Renal Clearance and Glomerular Filtration Rate.
In this context the most important adverse reaction is represented by contrast-induced nephropathy (CIN) which is defined as an increase in serum creatinine> 25% or 0.5mg / dl that occurs within three days of administration in the absence of cause alternative.
Evaluation of creatinine clearance and a careful anamnestic investigation of known renal diseases are fundamental in the prevention of CIN.
The generally accepted cut-offs and the strategies to be implemented are shown in Table 9.
Regarding the intake of oral hypoglycemic agents such as Metformin,
the latest ESUR guidelines recommend suspension 48 hours before the examination only in patients with eGFR = 30-44 ml/min/ 1.73m2 and the subsequent resumption of therapy is recommended after 48 hours from the examination in this case,
if the renal function is not compromised.
[7]
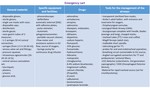
How to treat various acute adverse reactions?
Although the spectrum of adverse reactions to intravenous contrast media is very large,
the radiologist is often called upon to deal with acute reactions such as immediate hypersensitivity and anaphylactic reactions.
For this reason,
it is essential for the radiologist to be able to identify them,
recognize them and treat them early in relation to the specific clinical manifestation.
The execution of the diagnostic procedure in safety foresees,
first of all,
the presence of an emergency trolley,
easily accessible and adequately supplied for emergency rescue.
[8].
(Table 10)
In the case of mild adverse events such as nausea,
vomiting or itching,
only careful observation may be sufficient,
which can be followed by spontaneous resolution of symptoms and possible support treatment.
In the event that the symptoms persist,
it is necessary to implement a rapid therapeutic strategy,
specific in relation to the symptom (Table 11-12-13-14-15; Fig.
3-4-5):
• the presence of widespread and rapidly progressing wheals is suggestive of urticarial reaction and requires a scrupulous exploration of the entire skin surface and antihistamine infusion;
• difficulty in breathing may suggest the presence of an asthmatic attack,
whose therapy is mainly based on the administration of beta 2-agonists and/or adrenaline,
or laryngeal edema that requires the adrenaline infusion; for this reason,
chest auscultation is fundamental in order to make a reliable diagnosis.
In the most serious cases,
with impairment of vital functions,
it is essential to proceed with first-aid maneuvers and apply a univocal and standardized cardiopulmonary resuscitation protocol such as the Basic Life Support (BLS) which must be known to all operators in the sector.
[5,7,8] (Table 16)
The management of the patient who has manifested a hypersensitivity reaction to contrast media requires a series of safety measures as reported in Table 17.