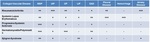
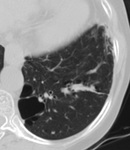
General Considerations and ILD Patterns in HRCT
Pulmonary alterations,
often ILD,
may be the first manifestations of CTD preceding other clinical and laboratorial findings,
sometimes by years.
Other radiologic findings in HRCT that are suggestive of underlying CTD include oesophageal abnormalities,
pleural and pericardial effusions and thickening,
pulmonary arterial enlargement,
and osteoarticular disease (such as glenohumeral joint involvement in RA) and mediastinal lymphadenopathy.
ILD patterns are dependant on the underlying CTD,
varying in frequency and presentation.
The most common histopathologic patterns of ILD are nonspecific interstitial pneumonia (NSIP),
usual interstitial pneumonia (UIP),
organizing pneumonia (OP),
and lymphoid interstitial pneumonia (LIP).
NSIP is the most common ILD pattern in CTD (CTD-related NSIP is also more frequent than idiopathic NSIP).
Histologically,
it is characterized by homogeneous expansion of the alveolar walls by inflammation or fibrosis.
Ground glass often presents with subpleural sparing,
and is more frequent than honeycombing,
but reticulation and traction bronchiectasis can be seen.
UIP is the second most commonly observed pattern,
especially in patients with RA and PSS.
The alterations are similar to the ones present in idiopathic pulmonary fibrosis (IPF),
but the prognosis for UIP in CTD is better than in IPF.
HRCT features include peripheral and lower lobe predominance of reticulation,
traction bronchiectasis,
and honeycombing.
Visualization of these patterns if often better with coronal reformatting.
OP can occur with any CTD,
but is more common in PM-DM.
Ground-glass opacities or consolidation in basal distribution with peripheral and peribronchovascular predominance are typical and the “reverse halo or atoll sign” can be seen.
LIP is a more uncommon presentation,
usually associated with SS (less frequently with SLE and RA).
HRTC shows basal-predominant ground-glass opacities and thin-walled cysts (Table 1).
Rheumatoid Arthritis
RA affects 1 to 2% of the population,
being one of the most common connective tissue diseases.
It is characterized by progressive and symmetric inflammatory polyarthropathy,
usually in the small joints of the hands and feet.
The disease itself is three times more prevalent in women,
however lung disease is more common in men.
In most patients,
clinically relevant articular abnormalities precede pulmonary or pleural disease.
Lung disease is the second most common cause of death (the first being infection).
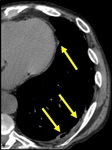
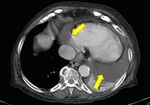
Pleural disease,
namely plural thickening,
is the most common thoracic manifestation,
occurring in about 38%–73% of patients (Fig.
1).
Effusions are rarer (5% of patients),
small and unilateral,
usually resolving spontaneously.
Not related to the presence of pulmonary disease.
Clinically significant ILD is present RA in about 5% patients.
Numerous patterns of interstitial disease (including NSIP,
UIP,
COP or LIP) may be seen in patients with RA.
However,
unlike in other connective tissue diseases,
patients more often present with a pattern of UIP (in more than 50% of cases).
The course of fibrosis in UIP associated with RA is usually milder than IPF and the distribution may be more diffuse or predominantly in the anterior aspect of the upper lobes which is rare but typical for RA.
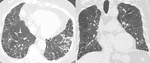
Findings include fine reticulation,
honeycomb cysts (most evident at the periphery of lung bases),
traction bronchiectasis and volume loss in the lower lobes.
Ground glass opacities are also seen in 15% of patients.
The distinction between UIP and other types of interstitial lung disease is important,
as it carries a significant worse prognosis (similar to IFP).
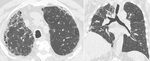
Other findings in RA include bronchiectasis,
present in 20% of patients,
pulmonary hypertension (usually present due to fibrosis) and obliterative bronchiolitis.
(Fig 2.)
Rheumatoid nodules are an uncommon manifestation of RA.
Often asymptomatic,
these nodules are well-defined and peripherally located in the upper and mid lung,
and may cavitate.
They are solitary or multiple and usually measure a few millimetres to five centimetres.
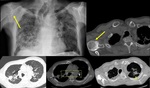
Caplan's Syndrome,
also known as rheumatoid pneumoconiosis syndrome,
this rare condition is an association of RA with coal worker’s pneumoconiosis or silicosis,
characterized by single or multiple lung nodules (Fig.
3).
Systemic Lupus Erythematosus
SLE is multisystemic autoimmune disease,
associated with an increase of serum antinuclear antibodies in 95% cases.
It occurs predominantly in women,
usually in a reproductive age (>90%).
Clinical diagnosis relies on the presence of at least four of the following: rash,
discoid lupus,
photosensitivity,
oral ulcers,
arthritis,
serositis,
renal disorders,
neurologic disorders,
hematologic disorders or immunologic disorders.
Pleural or pulmonary involvement is reported in more than 50% of patients and is the most frequent respiratory manifestation,
and pleuritic chest pain,
cough and dyspnoea are typical symptoms.
Pleural effusions are found in 30%–50% of cases and may be unilateral or bilateral.
Lupus pleuritis may be diagnosed through pleural fluid serology,
as ANA concentration in the pleural fluid will be higher than in the blood stream.
Pericardial effusion and cardiomegaly occur in 35% of patients with SLE.
(Fig.
4)
As the treatment of SLE involves the usage of immunosuppressants drugs,
infections,
especially bacterial pneumonia are the most common pulmonary complication the second most frequent cause of death.
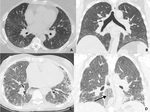
About 5% of present with acute lupic pneumonitis,
appearing as scattered and irregular areas of consolidation or ground-glass opacity,
more predominant of the lower lobes.
Symptomatic interstitial lung disease is uncommon in SLE (only 3% cases),
NSIP being the common histologic pattern,
followed by UIP (Fig 5).
The incidence of lung fibrosis is only apparent in 30% of HRCT,
usually in the periphery and lung bases.
Pulmonary hypertension is rare.
Diffuse pulmonary haemorrhage is a rarer (2,0%–5,4%),
but potentially fatal complication,
that may mimic lupic pneumonitis.
The most common HRCT manifestations include septal thickening in the lower lobe,
architectural distortion,
and ground glass opacities.
Shrinking lung syndrome is a rare,
and underdiagnosed,
cause of respiratory disease in patients with SLE,
characterized by loss of lung volume without fibrosis or pleural disease.
It usually presents with elevation of the hemidiaphragms,
basal atelectasis,
without significant ILD or pleural disease (Fig 6).
Progressive Systemic Sclerosis (Sclerodema)
Progressive Systemic Sclerosis (PSS) is a multisystemic connective tissue disease characterized by fibrosis,
inflammation and vascular damage.
It is three times more frequent in women and has a peak incidence in the range of 45-64 years.
Pulmonary involvement is very common in patients with PSS,
especially ILD and pulmonary artery hypertension and is found in up to 75% of cases.
The most common pattern of ILD is NSIP followed by UIP (with worse prognosis than NSIP but better long-term prognosis than IPF).
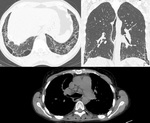
The main HRCT features include ground glass opacities superimposed on coarse or fine reticulation,
honeycombing and traction bronchiectasis.
The manifestations are located in the lower lobe and are predominantly usually concentric subpleural.
Ground-glass opacites are more common than in IPF.
Other findings on HRCT include pleural effusion or thickening evident in 35% of patients,
mediastinal lymph node enlargement in 60% and esophageal dilatation in 40%-80%.
Progressive systemic sclerosis is associated with the highest mortality in patients with CTD,
pulmonary arterial hypertension being its leading cause of death (Fig 6 and Fig 7).
Polymyositis and Dermatomyositis (PM/DM)
PM/DM are autoimmune inflammatory myopathies,
characterized by sudden onset of proximal symmetric muscle weakness.
They are more common in women,
with a peak incidence of 40-50 years.
Clinically,
both diseases are distinguished by cutaneous manifestations in dermatomyositis,
typically a rash on the upper eyelids and knuckles.
Patients with PM/DM may develop respiratory complications,
due to respiratory and pharyngeal muscle weakness.
PM-DM is less commonly associated with pulmonary involvement than other connective tissue diseases,
with ILD occurring in 5%-30% cases.
The most common patterns are NSIP and OP ,
often seen in the same patient.
Polygonal shaped consolidations are commonly seen,
with predominantly subpleural and peribronchial distribution,
most commonly in the lower lung (OP pattern).
These areas may only be few centimetres or fill the entire lobe,
appearing as masses containing air bronchograms.
Crescentic opacities surrounding areas of ground-glass opacity (the “atoll” or “reverse halo” sign) can be seen (Fig.
8).
Treatment may reverse these alterations but reticular opacities and traction bronchiectasis corresponding to fibrosis in NSIP may appear.
Honeycombing is relatively rare (15%) and is associated with UIP.
Extrapulmonary thoracic manifestations of PM-DM are rare.
Some PM-DM patients have antisynthetase syndrome,
characterizes by inflammatory arthritis,
myopathy,
Raynaud,
fever,
oesophageal dysfunction and ILD (present in more than 80% of patients).
Anti–Jo-1 is the most common antisynthetase antibody,
and is present in 50-70% of patients who ILD.
Sjögren Syndrome
SS is an autoimmune disorder that affects primarily the exocrine glands.
It is nine times more prevalent in females,
most frequently in the fourth to fifth decades. Clinically,
it is characterized by xeroftalmia and xerostomia.
Most cases of SS are primaty,
however 33% are associated with other CTD (such as RA,
SLE,
or PSS).
ILD is common in SS,
most often NSIP,
but LIP,
UIP and OP can also be seen.
HRCT findings are nonspecific and include ground glass opacity,
fibrosis,
and bronchiectasis,
located in the lower lobes.
Airway involvement is common,
with bronchiectasis and tree-in-bud pattern.
Thin-walled lung cysts,
usually multiple,
have been described and are typical of LIP (Fig 9).
Patients with this pattern may also present with ground glass opacities,
bronchial and interlobular septal thickening,
and mediastinal adenomegaly.
SS also carries an increased risk of lymphoma and may result in diffuse interstitial infiltration or multiple nodules.