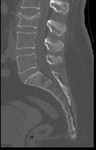
RADIOLOGICAL EXAMINATION IN TRAUMATIC SPINAL CORD INJURY
Radiologic evaluation of an injured spine includes simple x-rays,
computed tomography and magnetic resonance imaging (MRI).
The purpose of radiologic evaluation is:
- Identify the location and extent of the lesion.
- To determine the characteristics of vertebral instability.
- Evaluate the severity of neurological compression and injury.
- Classify patterns of injury.
- Identify multilevel injuries.
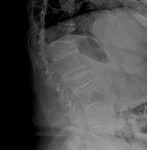
Good quality simple x-rays should be performed in two planes (antero-posterior and lateral) in all patients with suspected spinal trauma.
If x-rays are unsatisfactory or inconclusive,
a CT scan should be performed.
In many centers,
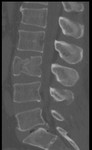
computed tomography is performed routinely because it reveals fractures that are not visible on simple x-rays in more than 20% of patients.
CT scans are part of the evaluation for the AOSpine classification.
They represent bone lesions more accurately and have a sensitivity and specificity > 95%,
also allowing multiplanar reconstructions.
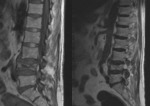
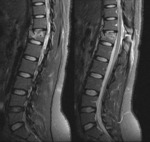
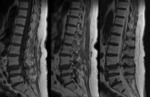
MRI scan provides useful information about the extent of soft tissue injury that has occurred during spinal cord injury.
It is indicated in patients with neurological deficit and suspected posterior ligament complex injury [12].
AOSPINE THORACOLUMBAR SPINE INJURY CLASSIFICATION SYSTEM
To address categorization a clear distinction must be made between classification systems,
severity measures and treatment algorithms [14].
Other medical prognostic factors,
comorbidities and neurological deficits also have an impact on treatment decisions but must be considered separately and are therefore not integrated into the current classification system.
The AOSpineThoracolumbar Spine Injury Classification System is based on the evaluation of 3 basic parameters:
1.
Morphologic classification of the fracture
2.
Neurological status
3.
Clinical modifiers
1.
Morphologic classification of the fracture
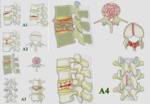
Three main forms of spinal integrity failure were defined and listed in ascending gravity as:
- Type A lesions: failure under axial compression of the anterior elements with posterior restriction elements intact.
- Type B lesions: failure of the posterior restriction elements.
- Type C lesions: failure of the anterior and posterior elements that lead to displacement.
Considerations:
- Multilevel lesions (present in 15% of patients) should be classified separately and listed according to severity.
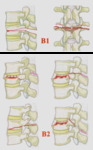
- All type A compression lesions and subtype B1 lesions (transosseous posterior tension band rupture) are at the level of a single vertebra.
Their location is thus designated by the involved vertebra traditionally designated with a letter (T or L) and a number (1 to 12 or 1 to 5) depending on the spinal region involved.
All C-type displacement injuries and subtype B2 (posterior tension band ligament rupture) involve movement segments by definition and are therefore located at the specified level of the movement segments involved.
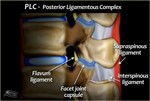
- The posterior restriction elements in the case of toracolumar injuries are the facet joints and the posterior oseo-ligamentary structures (supraspinous ligaments,
interspinous ligaments and ligamenta flava),
also called PLC (posterior ligamentous complex).
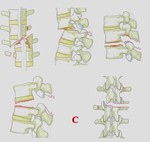
Fig. 1
Type-A injuries: compression injuries of the vertebral body
In the thoracolumar spine,
type A lesions are represented by compression injuries with fractured vertebral body without interruption of posterior constraining elements or signs of displacement or dislocation. They are divided into 4 subtypes:
A0 - Minor or nonstructural fractures.
This code is used to describe negligible fractures that do not significantly affect spinal stability,
such as a fracture isolated from the spinal process,
the transverse process,
or the lamina.
A1 - Wedge compression or impaction fractures.
These are fractures of the vertebral body with one or both end plates involved,
but the fractures do not connect to each other.
Remember,
the posterior wall of the vertebral body remains intact,
indicating that there is no violation of the spinal canal.
Fig 3.
A2 - Split or pincer type fractures.
These are fractures of the vertebral body in which the fracture affects both terminal plates without the involvement of the posterior wall of the vertebral body.
Fig 4.
A3 - Incomplete burst fractures.
This injuries are vertebral fractures affecting a single endplate associated with the involvement of the posterior vertebral wall.
Fig 5.
They are commonly called burst fractures.
The PLC and the facet joints remain intact.
There may be a vertical fracture of the lamina as a result of the increase in the interpedicular distance,
without there being vertebral translation.
A3 fractures of the vertebral body involving a horizontal fracture in the axial plane through the posterior elements interrupt the stability of the spinal column,
and such injury should be classified as a type B injury.
It should be noted that involvement of the posterior wall with retropulsed bone elements may cause invasion of the spinal canal with posterior neurological deficits.
A4 - Complete burst fractures.
These are fractures of the vertebral body involving both terminal plates and the posterior wall of the vertebral body.
As in A3 lesions,
these may be associated with vertical fracture lines of the lamina,
but without interruption of the posterior tension band.
Fig 6.
Split fractures that also involve the posterior vertebral body are included in this.
Type-B injuries: 'tension band' or PLC injuries in the TL spine.
Type B denotes failure of the posterior restraining elements.
They are often combined with type A fractures (to be specified separately) due to a flexion distraction mechanism that causes compression of the vertebral body.
They are divided into two subtypes:
Lesions of subtype "B1 - Transosseous tension band disruption / Chance fracture". It is a failure of the monosegmental transosseous tension band.
These are the classic "Chance" fractures.
There is no substantial compression fracture of the vertebral body.
These injuries are unique due to the presence of a horizontal fracture that extends through the vertebral body and pedicles.
Lesions of the subtype "B2 - Posterior tension band disruption". Include the other types of interruption of the posterior tension band with or without posterior bone involvement Fig. 8
According to AOSCG,
the fracture lines can be seen through posterior bone elements,
for example,
facet joints,
the interarticular portion of the isthmus (spondylolytic injuries),
or the spinous process extending to the interspinous ligaments.
Facet or subluxation fractures may also be seen with the consequent kyphotic deformity of the movement segment(s) involved.
Type-C injuries: displacement injury
Type C are lesions are characterized by an abnormal displacement of the cranial and caudal parts of the spine in any plane Fig. 9 .
They involve a distraction or separation of the anterior and posterior components of the vertebral segments without any anterior or posterior structure remaining intact,
and there may be a complete separation of the vertebral elements.
The interruption of the anterior component can be through the disc or vertebral body.
The rupture of the posterior elements can be through the spinous process,
lamina,
pars interarticularis or posterior ligament complex.
There are no subtypes,
since due to the dissociation between the cranial and caudal segments it is possible to make different configurations in different images,
which are not relevant.
It is combined with subtypes of A to denote the associated fractures of the vertebral body if necessary.
Note: A typical coding sample would be L3/ L4 - type C (L4-B2,
L4-A3) indicating that the translation is at the L3 / L4 level with an associated incomplete burst fracture of L4 and failure of the posterior restraining elements. Fig. 10
2.
Neurological Status
The neurological state is classified according to a system of 5 subsections that are coded with the letter N and a figure according to the type of deficit.
3.
Clinical modifiers
They would be used only when necessary to help the doctor decide on treatment.
M1 is used to designate fractures with an indeterminate lesion in the tension band based on images of the spine,
such as MRI or clinical examination.
This modifier is important in identifying those lesions that appear stable from a bone point of view in which ligament insufficiency can help determine whether operative stabilization is a consideration.
M2 is used to designate a patient-specific comorbidity,
which could argue for or against surgery for those patients with relative indications for surgery.
Examples of an M2 modifier include such disorders,
but are not limited to ankylosing spondylitis,
topical conditions,
diffuse idiopathic skeletal hyperostosis,
osteopenia/porosis or burns affecting the skin covering the injured spine.
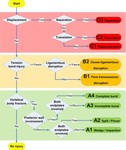
DIAGNOSTIC ALGORITHM AND FINAL CODING
The AOSpine group also published a systematized algorithm specific to the TL region that ensures a comprehensive approach in which no lesions are misdiagnosed [9].
Fig. 11