|
PLEUROPARENCHYMAL FIBROELASTOSIS
|
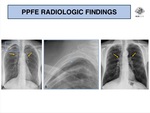
Chest radiographs are nonspecific for the diagnosis of PPFE,
most commonly revealing apical reticulation,
upper lobe volume loss and consequently upward hilar retraction (Fig. 3).
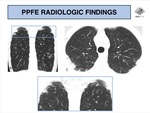
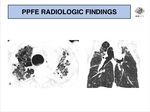
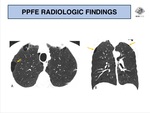
HRCT characteristically shows bilateral pleural thickening and subpleural reticulation,
with upper lung predominance and accompanying volume loss causing upward hilar retraction (Fig. 4 - 9).
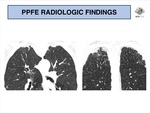
Associated features include architectural distortion,
traction bronchiectasis and honeycombing (Fig. 6 and Fig. 7).
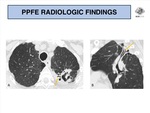
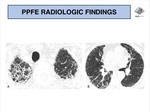
Involvement by large cysts and bullae might be identified (Fig. 8),
possibly explaining the high incidence of pneumothoraces in PPFE patients [8],
with contribution of a reduced resistance pleura to mechanical stress.
Some patients may demonstrate coexistent fibrotic changes in regions distal to the pulmonary apices (frequently UIP or NSIP-like),
but an apical-caudal distribution frequently persists (Fig. 9).
Surgical biopsy or autopsy is essential for the definite diagnosis of PPFE. [5]
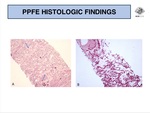
The key histological findings are fibrous thickening of the visceral pleura and prominent,
homogeneous intra-alveolar fibrosis with septal elastosis,
abruptly demarcated from the adjacent “normal” lung parenchyma (Fig. 10).
A scant,
patchy,
lymphoplasmocytic infiltration may be also described,
as well as a limited number of fibroblast foci.
Partial stenosis of pulmonary vasculature (arterial and venous),
can be present.
Elastic fibers in alveoli septa are more readily identified by using specific stains,
such as orcein or van Gieson (Fig. 10).
- Radiologic-pathologic Correlation
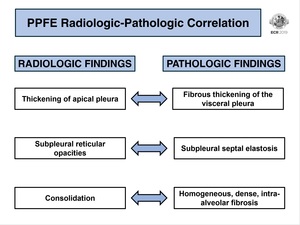
Fig. 11: PPFE radiologic-pathologic correlation.
References: Department of Radiology, Centro Hospitalar de São João - Porto/PT
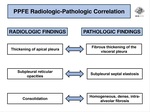
The radiologic features previously described are the imagiological correspondent to the histological findings (Fig. 11):
- Fibrous thickening of the visceral pleura is seen as thickening of apical pleura in radiographs/CT.
- Subpleural reticular opacities correspond to septal elastosis.
- Consolidation usually represents the homogeneous,
dense,
intra-alveolar fibrosis.
- The abrupt transition from abnormal lung to normal tissue in histology is regularly also seen in HRCT.
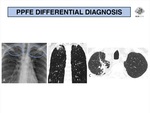
· Asbestos exposure;
· Apical cap;
· Previous pulmonary tuberculosis;
· Chronic hypersensitivity pneumonitis;
· Connective tissue disorders;
· Radiation or drug-induced lung disease;
· Idiopathic pulmonary fibrosis;
· Neoplasms;
· Advanced fibrosing sarcoidosis.
|
LYMPHOID INTERSTITIAL PNEUMONIA
|
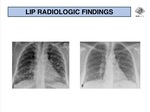
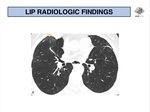
Chest radiography is neither sensitive nor specific for LIP.
Most frequently,
a reticular pattern is seen,
predominantly in the lower lung zones bilaterally (Fig. 13).
While LIP is considered a diffuse interstitial pneumonia,
there is a noticeable propensity to involve the perilympathic interstitium (peribronchovascular regions,
interlobular septa and the pleura).
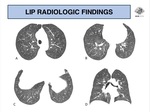
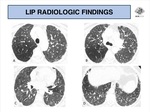
HRCT features vary according to the associated underlying disease.
For example,
in patients with immunodeficiency,
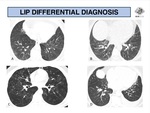
usually diffuse or patchy areas of ground-glass opacity/consolidation are seen (Fig. 14).
Another common presentation is centrilobular ill-defined nodules,
most frequently seen with underlying connective tissue disorders or AIDS.
Conversely,
well-defined nodules with peribronchovascular distribution or septal thickening might also be seen in AIDS (Fig. 15 - Fig. 16).
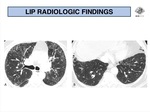
Lastly,
isolated thin-walled cysts of variable shape and size,
are a characteristic abnormality,
and is most commonly seen in Sjögren’s syndrome and other collagen-vascular diseases.
More infrequently,
a diffuse cystic pattern that mimics honeycombing is a possible presentation (Fig. 17).
In most cases,
surgical lung biopsy is necessary for the diagnosis of LIP.
[16]
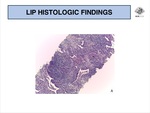
The key histological findings are dense interstitial lymphoid infiltrates that diffusely expand and widen interlobular and alveolar septa (Fig. 19).
These infiltrates are generally polymorphous,
consisting predominantly of lymphocytes (mainly T-cells),
plasma cells,
immunoblasts and histiocytes.
The referred histological pattern is most pronounced in the areas surrounding lymphatic channels (peribronchovascular regions,
interlobular septa,
alveolar septa and subpleural areas).
Lymphoid follicles may be present.
Small airways and capillaries might be affected.
- Radiologic-pathologic Correlation
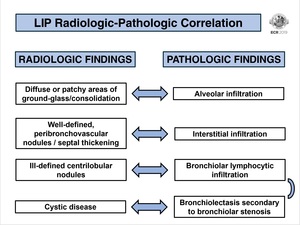
Fig. 20: LIP radiologic-pathologic correlation.
References: Department of Radiology, Centro Hospitalar de São João - Porto/PT
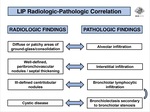
The radiologic features previously described are the imagiological correspondent to the histological findings (Fig. 20):
- Diffuse or patchy areas of ground-glass opacity/consolidation correspond to alveolar infiltration;
- Interstitial infiltration is seen in CT as well-defined,
peribronchovascular nodules or interlobular septal thickening;
- Ill-defined centrilobular nodules represent bronchiolar lymphocytic infiltration.
- If the above mentioned bronchiolar lymphocytic infiltration cause bronchiolar lumen stenosis,
some cysts may be seen (bronchiolectasis).
· Cellular nonspecific interstitial pneumonia;
· Hypersensitivity pneumonia;
· Chronic lymphocytic leukemia and other lymphoproliferative disorders;
· Lymphangitic carcinomatosis;
· Infection (+ P.
carinii);
· Nodular lymphoid hyperplasia;
· Sarcoidosis;
· Desquamative interstitial pneumonia.