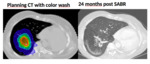
Fifty patients underwent SABR on 64 nodules.
38 patients underwent a single SABR procedure.
11 patients had SABR on two different nodules.
One patient was treated four times with SABR on different lesions.
Of 64 nodules treated with SABR only 36 have a first CT within 6 month from the end of SABR.
Our data about acute lung injury are limited but in line with the literature (6),we identified: 13 diffuse consolidation (36%),
8 patchy consolidation (22%),
2 diffuse GGO (6%),
6 patchy GGO (17%) while 7 nodules didn’t show any change (19%).
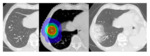
All the 64 nodules have a follow up after 6 months.
As late radiological changes we identified 37 modified conventional pattern of fibrosis (58%),
14 scar-like fibrosis (22%),
10 mass-like fibrosis (16%); 3 nodules didn’t show any change (4%).
Strictly following Nguyen criteria of imaging analysis,
we identified 26 local recurrence (LR) (39%),
while in a further review of these cases with a more critical approach,
combining both morphologic criteria described in the literature and radiological experience in this field,
we identified 15 LR (23%).
This discrepancy has been explained by the radiologist as follow: three patients had HRFs of LR but it was definitely considered as a SABR side effect (radiation induced pneumonia),
confirmed by clinical and imaging follow up; three patients had progression disease from contiguous lesions that spread to the SABR zone which technically shouldn’t be considered as LR; two patients presented three HRFs among which two were infiltration into adjacent organs/structures and airspace obliteration/loss of air bronchogram,
but in these particular cases there was infiltration of a segmental bronchus with consequential loss of air bronchogram,
therefore these features cannot be considered separately; three patients despite presented at least 3HRFs of LR have been considered to have a post actinic fibrosis,
confirmed at follow up.
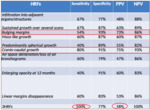
Diagnostic accuracy of each HRFs proposed by Nguyen et al.
has been analyzed,
further more we tested two more criteria with a certain relevance according to literature review,
enlarging opacity at 12 months and linear margins disappearance,
in the end we evaluated a combined accuracy of at least 3 HRFs as proposed by Nguyen et al.,
results of these analysis are listed in table 4.
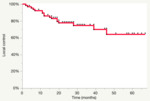
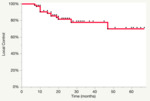
Local control evaluated with the three different methods showed interesting result: at 1 year LC was quite similar with all the three different methods of evaluation,
at two years significant difference can be appreciated,
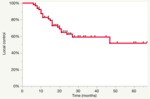
in particular with conventional clinical evaluation (fig.10) LC resulted 78 % vs 62 % according to Nguyen criteria (fig.
11) and 81% according expert radiologist evaluation using Nguyen criteria (fig.12); further difference about LC evaluation is seen at 3rdyear with LC respectively of 74%,
59% and 78% (Table 5).
Discussion
This study derived from the need to overcome the diagnostic difficulties encountered during multidisciplinary lung meetings while discussing SABR patient’s follow up.
SABR is acquiring a pivotal role in the treatment of lung lesions and considering the high number of long term survival patient,
being familiar with acute and late lung injury post SABR is mandatory.
While analyzing lung injury pattern we identified other typical post SABR image to be familiar with: subpleural radiation fibrosis (fig.8) and air bronchograms (fig.9).
In the beginning SABR was only for frail or inoperable patients,
but since now is an option for younger and more fit patients,
being familiar with HRFs of local recurrence is very important therefore several articles focused on this topic (11-15).
In agreement with Puelen et al.
(11) even in our cohort of patient the two most important HRFs are bulging margins and CC growth with the latter being the most performant single HRFs of LR (sensitivity 80%,
specificity 91%,
PPV 75% and NPV 93%); others HRF analyzed independently showed low sensibility (between 40% and 67%).
The only way to increase sensitivity is to use a “high –risk count” cut-off of 3 or more features as proposed by several opinion leaders in SABR imaging (12,5).
However the presence of 3 HRFs implies a low PPV and this is explained mainly by SABR side effects such as radiation induced pneumonia and post SABR atelectasia,
especially in case of central lesions (<2cm from the lung hilum).