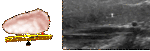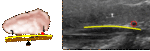A) Position of the patient and technical considerations:
Patients should be placed in supine position with the patient's head reclined (Figure 1).
Broadband transducers with a high frequency,
up to 18MHz were used.
It is advised to use probes with a maximum resolution and sufficient penetration.
Ultrasound has a relatively good view of the different structures of the larynx,
allowing an excellent assessment of cervical soft tissue and of the vocal cords.
A possible exception to this rule involves older men,
whose thyroid cartilage morphology and calcification may block an access to the larynx from an echographic point of view.
To overcome the morphology limitation,
a fluid interface (water bath) can be used (Figure 2).
It is also useful in more superficial structures because allows placement of the object of interest into the focal zone.
To overcome the thyroid cartilage calcifications,
a side or lateral access allows a better assessment of the vocal cords (Figure 9).
B) Anatomy:
Larynx scanning can be initiated at the level of the hyoid bone down to the inferior border of the cricoid cartilage in transverse,
longitudinal and oblique planes.
Particular attention should be given to the assessment of the pre-epiglottic and paraglottic spaces in patients with tumors of the neck since its invasion by oropharyngeal or supraglottic laryngeal carcinomas will imply changes in the treatment course.
B1.
Appearance of different mediums of the airway
The larynx is part of the airway and the phonation organ. The appearance of different cartilages is descripted on Figure 3.
The differences are related to different degrees of calcification of the cartilages.
Bone appears as a bright hyperechoic linear structure with hypoechoic acoustic shadow.
Fat and glandular structures are homogeneous and hyperechoic.
Muscle and connective tissue are hypoechoic,
heterogeneous,
with striated appearance.
Air–mucosa interface is seen as a bright hyperechoic linear.
Intraluminal air produces comet tail and reverberation artefacts.
Vessels are anechoic surrounded by hyperechoic tissue and nerves hypoechoic surrounded by hyperechoic tissue.
B2.
Acoustic windows:
Acoustic windows that are suitable for the penetration of ultrasound beams:
- thyrohyoid membrane;
- cricothyroid membrane;
- thyroid cartilage lamina (if little calcification).
B3.
Evaluation by level:
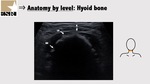
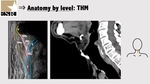
3.1: Hyoid bone and thyrohyoid membrane
The hyoid bone is visible on the transverse view as a hyperechoic inverted U-shaped linear structure with posterior acoustic shadowing (Figure 4).
On the sagittal view the hyoid bone has a narrow hyperechoic curved structure that casts an acoustic shadow (Figure 7).
The thyrohyoid membrane extends from the superior edge of the thyroid cartilage to the body and the interior edge of the mayor apophysis of the hyoid bone.
Also at this level is identified the thyroepiglottic ligament that connects the epiglottis to the angle formed by the two laminae of the thyroid cartilage (Figure 7).
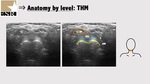
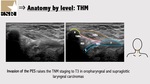
Due to the acoustic window produced by thyrohyoid membrane it is possible to visualize pre-epiglottic space (Figure 5,7 and 8) that is at high risk of involvement in oropharyngeal and supraglottic laryngeal carcinomas,
being important in staging.
Invasion of the PES raises the TNM staging to T3 in oropharyngeal and supraglottic laryngeal carcinomas which will imply more aggressive treatments.
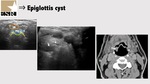
Epiglottis is a leaf shaped fibrocartilage.
Lesions of the epiglottis in which ultrasound is useful include cysts (Figure 6),
epiglottitis,
and pretherapeutic staging of cancer.
Just anteriorly to the thyrohyoid membrane we can identify thyrohyoid muscle,
with its origin on the thyroid cartilage (oblique line) and insertion on the hyoid bone (body and great cornus).
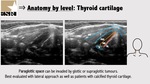
3.2: Thyroid cartilage and vocal cords
The thyroid cartilage can function as an acoustic window to visualize the glottic space of the larynx.
In an important percentage of the patients the cartilage is calcified partial or totally,
and this limitation can be overcome by using a lateral approach (Figure 9).
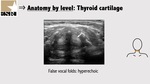
True vocal cords are composed by the vocal ligaments that are attached posteriorly to the arytenoid cartilages and anteriorly to the thyroid cartilage and by the vocalis muscle that appears lateral to the ligament and hypoechoic (Figure 9). Ultrasound can visualize vocal cord nodules and polyps. False vocal folds sit slightly cephalad to the true vocal cords and appear hyperechoic (Figure 10).
Arytenoid cartilages are pyramidal shape and appear hyperechoic and homogeneous.
They are better explored during Valsalva manoeuvers which causes an adduction of the vocal cords that eliminates the air between the cords.
At this level an important space is paraglottic space and is best visualized in an oblique plane at the level of the thyroid cartilage (Figure 9).
The paraglottic space can also be invaded by glottic or supraglottic tumours hence the importance of its evaluation in these cases.
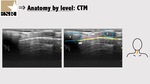
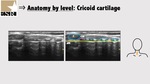
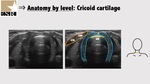
3.3: Cricoid cartilage and cricotracheal membrane
The cricoid cartilage (C) has an oval hypoechoic appearance in the parasagittal view (Figure 11 and 12) and can be seen as a hump in the transverse view (Figure 13).
The posterior surface of its anterior wall is delineated by an air mucosa interface.
At this level there is an acoustic window,
cricothyroid membrane.
Tracheal cartilages in longitudinal view appears as a “string of pearls”.
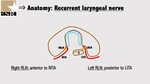
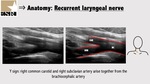
B4: Laryngeal recurrent nerve
Laryngeal recurrent nerve is seen as a linear structure,
hypoechoic surrounded by hyperechoic tissue,
1-2 mm in diameter on sagittal images of the lateral lobes of the thyroid gland.
It supplies all intrinsic muscles,
except cricothyroid.
On the left is seen between the thyroid and the cervical esophagus.
On the right is seen between the thyroid and the prevertebral plane (Figure 14 and 15).
The main causes of neuronal damage are:
- neoplasms;
- thyroid or parathyroid surgery complication;
- inflammation.
Non-recurrent laryngeal nerve (NRLN) is a rare anatomical variant (0.3–6%) that is associated with absence of the brachiocephalic trunk and presence of a right aberrant subclavian lusorian artery (Figure 16 and 17).
Usually,
the right common carotid and the right subclavian artery arise together from the bifurcation of the brachiocephalic artery,
describing a Y,
which has been named “Y sign”. The lusorian artery arises after the left subclavian artery as the fourth branch instead of the first one.The importance of recognizing this anomaly it’s because the right recurrent nerve could be divided thinking it is the inferior thyroid artery in patients with this anatomical variant.
C) Dynamic study
After the anatomic study,
the patient is asked to perform Valsalva manoeuvers and phonation with the intention of evaluating the vocal cord motion and vibration.
On quiet respiration,
the vocal cords can be distinguished as echogenic lines converging anteriorly. Asking the patient to say quietly a long "heee" establishes the correct positioning of the vocal cord plane for comparison of oscillation on the two sides.
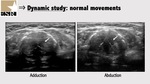
Normal vocal cord movements are summed up on Figure 18,
19 and 20:
- During normal inspiration,
the posterior cricoarytenoid muscle (PCA) contracts to abduct the vocal cords to enlarge the glottic opening.
- During expiration,
the relaxation of the PCA coupled with the contraction of the lateral cricoarytenoid muscle results in reduction of glottic opening.
- Normal vocal cord adduction also occurs during swallowing,
phonation,
the Valsalva maneuver and the early compressive phase of coughing
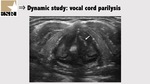
Vocal cord paralysis is seen when a vocal cord has no or little movement during phonation or with normal breathing,
with a median or paramedian position (Figure 21).
Even in patients with thyroid cartilage calcification it is possible to see the lack of comet tail and reverberation artefacts produced by air movement on the side of the paralyzed vocal cord (Video 22 and 23).
Unilateral involvement is much more common than bilateral involvement being the left side most commonly affected,
likely because the longer course of the left recurrent laryngeal nerve presents greater opportunity for injury.
D) Clinical indications:
The main application of US in the larynx are (Figure 24):
1- Vocal cord mobility:
- Preoperative detection of vocal cord palsy is important in thyroid and parathyroid surgery so that iatrogenic paralysis can be diagnosed and previous paralysis ruled out.
Routine fiberoptic laryngoscopy may bring patients unnecessary discomfort so ultrasound can be used to select patients to undergo laryngoscopic examination before surgery.
- Postoperative patients with dysphonia can be examined to evaluate vocal cord movement and possible tumor recurrence if the case.
- In unilateral vocal cord paralysis of unknown etiology lesions of the thyroid or parathyroid that cause compression or infiltration of recurrent laryngeal nerve can be found by ultrasound.
2- Laryngeal carcinoma:
Evaluation of the pre-epiglottic and paraglottic space and assessment of compromise of the thyroid and cricoid cartilages (limited with MR and CT).
These are of critical importance in the stratification of laryngeal cancer.
Other indications are:
3. Assessment of the diameter of the subglottic upper airway and prediction of endotracheal tube size specially in children.
4. Diagnose of epiglottitis specially in pediatric populations on emergency context.