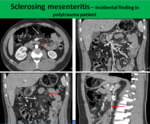
Sclerosing mesenteritis (SM)
Sclerosing mesenteritis is a rare condition characterized by pathologic processes of chronic inflammation (panniculitis),
necrosis (lipodystrophy) and fibrosis (scarring-retraction) of the adipose component of the intestinal mesentery.
(5) The prevalence ranges from 0.6% to 2.5 % (6) and cases are usually male (3:1) and older than 50 years of age,
although younger cases have been reported.
The disease can be asymptomatic when it is usually discovered as an incidental finding or can be related to unspecific symptoms such as abdominal pain,
nausea and diarrhea.
(7) (Fig 1) The etiology remains unknown but has been related to mechanisms such as abdominal trauma,
surgery,
ischemia,
infection and paraneoplastic syndrome and autoimmunity.
(7)
Many terms have been used in the literature to denote this condition: mesenteric panniculitis,
mesenteric lipodystrohy,
fibrosing mesenteritis,
retrectile mesenteritis,
liposclerotic mesenteritis,
mesenteric fibrosis,
mesenteric lipogranuloma,
xanthogranulomatous mesenteritis - often leading to confusion.
Some of them are used as synonyms and some are now considered obsolete.
(7,
8)
The evolution of the disease has been described in three stages,
according to histopathological findings:
1. Mesenteric lipodystrophy,
in which mesenteric fat is replaced by sheets of foamy macrophages.
Acute inflammatory signs are minimal or non-existent.
The disease tends to be clinically asymptomatic and prognosis is good.
2. Mesenteric panniculitis (MP) characterized by inflammatory changes and lymphatic distension with early fibrosis.
Histology reveals an infiltrate made up of plasma cells and a few polymorphonuclear leukocytes,
foreign-body giant cells,
and foamy macrophages.
This may be the beginning of symptomatic presentation.
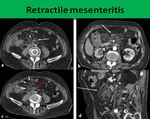
3. Retractile mesenteritis,
which shows collagen deposition,
fibrosis,
and inflammation.
Collagen deposition leads to scarring and retraction of the mesentery,
which in turn,
leads to the formation of abdominal masses and may cause obstructive symptoms.
(8)
For all that,
the exact correlation between these 3 stages hasn’t been proven yet and most articles refer to three types of the disease other than stages (8)
There are no uniform diagnostic criteria for diagnosing SM on CT.
However,
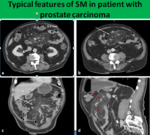
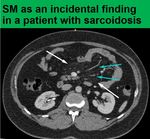
the subtype mesenteric panniculitis presents itself with typical findings on CT which are not specific as they may present themselves in other diseases of the mesentery as well.
(Fig.
2,
3):
1. Increased attenuation of mesenteric fat,
without mass effect on the mesenterial vessels,
though there might be a mild dislocation of the surrounding bowel loops.
The root of small bowel mesentery is most commonly affected (90%),
however mesocolon may be involved as well,
though far less common.
(7,8 )
2. Presence of tumoral pseudocapsule around the affected mesentery (usually <3mm thick) in 50-60% cases
3. Lymph nodes in the mesentery,
usually measuring <1cm in short axis diameter scattered around in 80% patients
4. “fat halo” sign,
around the vessels and lymph nodes (which denotes fat tissue unaffected by the inflammatory process) is present in 75% - 85%.
(7,8)
“Red flags” - signs whose presence should suggest a radiologist to consider another differential diagnoses
1. Presence of enlarged extramesenterial LN and short axis of mesenterial LN greater than 1cm (9) (Fig 4.)
2. Increased attenuation of fat spreading outside of the small bowel mesentery (mesocolon,
omentum,
retroperitoneum,
subcutaneous fat) (10)
Retractile mesenteritis (Fig 5) is on one hand considered final,
chronic,
stage of SM in which fibrosis predominates and the disease manifests itself as a mass of soft tissue attenuation with desmoplastic reaction in the surrounding mesentery thus causing retraction of adjacent vessels and bowel loops.
Calcifications may also be present.
(8).
Nevertheless,
there is still controversy regarding weather retractile mesenteritis presents the evolution of MP or should be considered a separate entity (6) Retractile mesenteritis cannot with certainty be distinguished from a mesenteric tumor (i.e.
carcinoid or lymphoma) based solely on radiological findings and extensive histological sampling is often required.
(10)
Some studies have suggested that some cases of idiopathic sclerosing mesenteritis might belong to the IgG4-related disease spectrum (11,
12,
13).
This is an immune-mediated systemic disorder characterized by the presence of lymphoplasmacytic infiltration rich in IgG4 plasma cells.
The incidence of isolated IgG4-related sclerosing mesenteritis remains unknown,
although it is considered uncommon.
(11,
12,
13)
There are no internationally accepted criteria for diagnosing of IgG4 related disease.
The criteria proposed by Japanese Research Committee for IgG4-related Systemic Sclerosing Disease propose the diagnosis to be made by combining radiographic,
serological and histopathological findings (11).
Whether or not MP can be regarded as paraneoplastic phenomenon is still a subject of debate as many studies have shown opposite results (6,
14). A matched pair analysis by van Putte-Katier et al showed patients with MP had a significantly higher prevalence of malignancies as well as a higher chance of future cancer development.
However it also stated that larger prospective studies with follow-up are necessary in order to confirm these findings,
to select high risk patients and establish recommendations for follow up imaging with regard to potential risk of cumulative radiation dose of a CT follow-up (6)
What should radiologist do when incidentally discovering findings of SM?
Even though further steps upon discovering signs of SM on CT are still not well established,
according to Nyberg et al (15) the possible connection between MP and malignancy should motivate a thorough clinical examination,
but does not motivate repeated radiological examinations if the symptoms are stationary.
They neither consider repeated radiological examinations to be an appropriate method for evaluation of the disease severity over time nor for determining the necessity of treatment and its effect.
Consequently,
decisions about the follow-up of patients with SM should primarily be based on the clinical picture (15)
The definite diagnosis of sclerosing mesenteritis is established by biopsy,
but it is rarely performed because of the high rate of cases presenting as incidental findings in asymptomatic patients (8)
Other causes of “misty mesentery”
Mesenteric edema
Mesenteric edema may occur due to systemic disease (hypoproteinemia,
heart failure,
nephrosis),
cirrhosis,
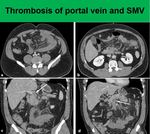
Budd-Chiari syndrome or mesenteric vein thrombosis.
When “misty mesentery” from edema is secondary to a systemic disease,
it is usually associated with generalized subcutaneous fluid and ascites.
On the other hand,
mesenteric edema secondary to mesenteric vein thrombosis tends to be focal (Fig.
6)
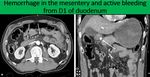
Mesenteric hemorrhage
Acute hemorrhage in the mesentery (Fig.
7) usually occurs due to trauma,
but may also be caused by anticoagulation therapy,
blood dyscrasia,
mesenteric ischemia or a ruptured vascular aneurysm Its main characteristic are high CT attenuation values (40–60 HU) and may be diffuse or focal.
(3)
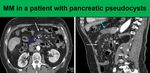
Inflammation
Inflammation within the mesentery and consequently its increased attenuation on CT can also occur as a secondary phenomenon due to inflammation in the surrounding organs.
(15).
Most commonly it occurs due to pancreatitis,
(Fig.
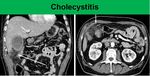
8) but also acute cholecystitis (Fig 9.),
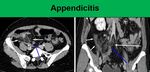
appendicitis (Fig 10),
diverticulitis,
inflammatory bowel disease,
infective peritonitis or tuberculous peritonitis,
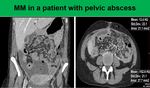
abscesses (Fig.
11) etc.
Mesenteric lymphoedema.
Primary mesenteric lymphoedema (small intestinal lymphangiectasia) is rare congenital abnormality in which dilated lymphatic channels within the intestinal villi lead to a diffuse nodular thickening of the small bowel wall and mesenteric lymphoedema as an accompanying finding.
Secondary mesenteric lymphoedema is caused by lymphatic obstruction due to constrictive pericarditis,
radiation-induced anomalies,
Crohn’s disease,
intestinal tuberculosis,
or intestinal lymphoma.
(3,
10)
Tumors
Primary neoplasms of the mesentery are rare.
They usually have a mesenchymal origin such as leiomyomas,
lipomas,
neurofibromas and their malignant counterparts.
In most cases,
primary mesenteric tumors are histologically benign,
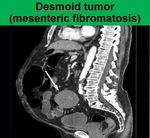
including desmoid tumors (mesenteric fibromatosis) (Fig.
12) which result from a benign proliferation of fibrous tissue and may occur in association with Gardner’s syndrome,
postpartum or post-surgery.
At CT,
they usually appear as soft-tissue masses with well-demarcated or poorly defined borders and strands radiating into the mesenteric fat.
Most mesenteric desmoid tumors are isoattenuating relative to muscle.
The mass usually doesn’t encase mesenteric vessels but often displaces them unlike SM.
(3,
4).
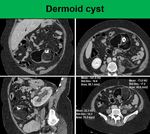
A very rare mesenteric tumor in adulthood represents mature teratoma (dermoid cyst) (Fig.
13)
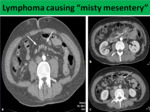
Lymphoma: Non-Hodgkin’s lymphoma is the most common malignant neoplasm affecting the mesentery.
It also represents the largest diagnostic dilemma towards SM,
especially early in the development of the disease when only mildly enlarged mesenteric lymph nodes are present.
Like MP lymphoma may also demonstrate “fat halo” sign and absence of displacement of mesenteric vessels (it encases them forming sandwich sign) (Fig.
4).
After therapy it may manifest only as increased attenuation of mesenteric fat,
without lymphadenopathy.
Calcification may also occur after treatment.
Features that favor diagnosis of lymphoma are:
1. Presence of lymphadenopathy outside of the mesenteric region (10)
2. Short axis diameter of largest LN within the mesentery larger than 1cm (3)
Carcinoid tumor: Primary carcinoid tumor as hyperenhancing nodule in the intestinal wall is often not detected due to small size.
Secondary carcinoid is found in mesentery by direct spreading and on CT can be seen as ill defined,
spiculated mass,
not so well demarcated,
with calcifications found in 70%,
desmoplastic reaction in the adjacent mesentery and no “fat hallo” sign.
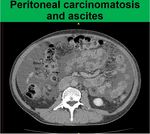
Small implants of carcinomatosis: In patients with primary malignancy small implants in the mesentery may cause stranding and nodularity which results in "pleated" or "stellate" appearance.
Other common sites include omentum,
paracolic gutters,
along surface of liver,
along undersurface of diaphragms,
and pelvic cul-de-sac,
thus distinguishing it from the primary diseases of the mesentery.
Ascites is usually present and in cases with advanced peritoneal carcinomatosis it is often loculated.
(4) (Fig.
14)
Primary mesenteric mesothelioma is a rare malignant neoplasm arising from peritoneum.
May present itself in two forms,
localized and diffuse and can also exhibit mesenteric soft-tissue implants without calcifications.