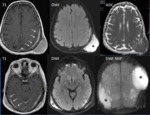
Case 1
A 61-year-old-patient receiving aspirin was attended by emergency medical services for seizures and head trauma.
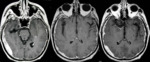
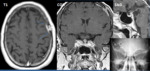
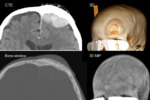
An emergency CT showed a right subdural mass with mass effect mimicking subdural hematoma.
The patient had no history of previous lymphoma.
MRI with contrast was performed and a diffuse thickening of the meninges due to lymphomatous dural infiltration was show (Fig.1).
Biopsy of the dura demonstrated a dural-based small B-cell lymphoma,
immunophenotypically most similar to those of mucosa-associated lymphoid tissues (MALT). After chemo and radiotherapy the patient responded well with complete response even after 1 year of follow-up was.
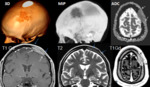
Case 2
A 27-year old male visited our center in May 2017 with right foot pain,
shortening of lower right limb and inability to march.
He was generally healthy and his medical history was unremarkable.
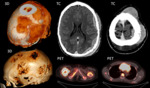
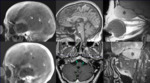
PET-CT showed a right femur lesion compatible with osteosarcoma and lesions in bones,
mediastinum and lung suggested metastasis (Fig.2).
The patient underwent a soft tissue biopsy of the femur's lesion and the result was compatible with diffuse large cell B lymphoma.
A cranial and cervical MRI made three months later showed several focal areas of iso- to low signal intensity alterations which were well enhanced with gadolinium in the left temporo-occipital and right temporo-parietal region of the skull compatible with bone tumor involvement (Fig.3).
Finally,
autologous transplant was decided with good evolution after treatment.
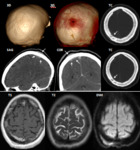
Case 3
A 62- year old woman,
with no remarkable medical history,
consulted on November 2016 in our emergency department with a palpable skull mass on the left parietal area.
The scalp mass was non-tender,
rubbery,
hard and non-movable.
She only referred bilateral periorbicular and upper lip paresthesias and weight loss in the last months.
She did not report headache or other associated clinic and the rest of neurological examination was normal.
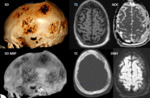
The scalp mass showed malignancy on PET-CT and the result of the biopsy made in June 2016 was compatible with diffused large b-cell lymphoma.
She received chemotherapy with complete remission of the lesions in a PET-CT made in October 2018 (Fig.
4).
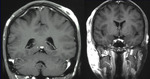
Case 4
A 66- year old woman consulted in our center in May 2018 for headache,
photophobia and memory loss.
She associated a motor deficit in lower right limb,
asthenia and weight loss in the last months.
She also referred a painful scalp mass in the right parietal area that she began to notice 15 days ago and a mass in right inguinal area.
Physical examination did not show neurological focality but two non-displaceable masses were palpated in the scalp and in the inguinal area.
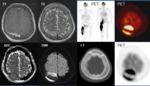
An abdominopelvic,
cranial CT and a biopsy were performed with the result of diffuse large cell lymphoma stage IV B and chemotherapy was decided (Fig.5)(Fig.6).
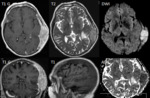
Case 5
A 68- year old woman consulted in our center for headache,
parietal lump 7 months of evolution.
She did not associate weight loss in the last months and his medical history was unremarkable except for diabetes.
Physical examination did not show neurological focality but two non-displaceable masses were palpated in the scalp.
An Chest-abdomino-pelvic CT was normal and biopsy was performed with the result of diffuse large cell B.
Brain MRI show diffuse intra- and extracranial agressive lytic mass (Fig.7).
Discussion
Primary dural diffuse lymphoma is a rare and aggressive B-cell NHL that arises in the dura mater,
mimicking primary central nervous system lymphoma.
It is a subentity of primary leptomeningeal lymphoma which represents 0.1% of all non-Hodgkin's lymphomas.
On the other hand,
although calvarial lymphoma is rare,
when painless scalp masses extending through the skull are seen lymphomatous involvement must be suspected.
Headaches,
convulsions or focal neurologic signs have been described as the first clinical manifestation of skull lymphoma.
Primary bone lymphoma PBL is a less common manifestation of lymphoma than secondary involvement from disseminated lymphoma.
It is also rare,
accounting for <5% of bone tumors and <1% of NHL.
This entity is defined as the presence of lymphoma isolated to one bone without distant spread for six months after diagnosis.
Multifocal PBL is less common and occurs with lymphoma is confined to two or more bones,
again without distant spread for six months. Imaging findings in primary and secondary lymphoma of the bone are similar.
Mycosis fungoides is a malignant,
cutaneous lymphoma of T-helper (TH or CD4+) cells usually limited to the skin,
with lesions that resemble eczema or psoriasis.
Neurologic involvement is uncommon but extracranial soft tissue infiltration can be a rare form of clinical presentation (Fig.8)
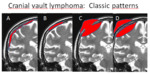
Cranial vault lymphoma patterns
Epicraneal soft tissues,
skull bones,
dura mater and brain parechimal can be affected.
Osseous involvement in haematological neoplasms may be confined to the bone marrow or involve the cortical and cancellous bone.
Cranial vault lymphoma have disseminated forms with multiple poorly-defined lytic lesions and focal forms as solitary lymphoma: a single large/expansile lesion most commonly both sides of calvaria.
So,
the radiographic features of skull and dural lymphoma could be variable (Fig.9) :
A. Diffuse dural thickening
B. Intraosseous infiltration (with sclerosing or moth-eaten pattern)
C. Expansive mass with and irregular cortical lytic destruction
D.
Expansive mass without obvious destruction of the cortical bone (permeative pattern),
reflecting the permeative lymphomatous nature.
Conventional radiography
ItôÇs still the first-order diagnostic study for the assessment of the cortical and trabecular bone; but,
it is not suitable for evaluation of the bone marrow.
It has a low sensitivity and a change of 30ã50% in mineral density is needed before a bone lesion becomes apparent on radiographs.
Computed Tomography
CT scan has higher sensitivity than plain radiography in detecting small lytic lesions.
CT is also useful for displaying cortical disruption,
periosteal reaction and soft tissue involvement.
CT is relative insensitivity in detecting subtle marrow changes.
Bone window and MPR-MIP increase the sensitivity.
PET/CT
18F-FDG PET/CT is a functional imaging technique which is useful in diagnosing focal osseous lesions as well as in detecting diffuse bone marrow involvement but it is less sensitive than MRI to detect marrow bone infiltration. PET/CT is the technique of choice for staging,
providing a whole-body (WB) evaluation.
Magnetic Resonance
MRI is the modality of choice for non-invasive evaluation of various marrow disorders because of its superior contrast resolution and ability to differentiate haematopoietic and fatty marrow. Relative absence of cortical destruction favours lymphoma over other bony neoplasms.
Commonly used MRI sequences include T1 weighted (T1W),
T2 weighted (T2W) sequences and T1W images after intravenous application of contrast agent (gadolinium).
Diffusion-weighted imaging
DWI is also helpful in evaluation of various marrow infiltrative disorders. Neoplasms exhibit more restricted water diffusion than normal tissues,
which is reflected as high signal intensity on DWI. Lymphomas in the skull base region have ADC values in the range of 0.51 to 0.59ãûã10ã3 mm2/s .
which are significantly lower than for nasopharyngeal carcinomas and skull base osteomyelitis.
So,
one characteristic finding of lymphoma is restricted diffusion with low ADC values due to hypercellularity of the tumor.
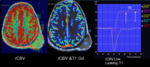
Dynamic susceptibility contrast-(DSC-) MRI
Perfusion DSC sequences are difficult to apply to calvaria lesions especially when they are small size.
However,
when the lesions are medium or large size,
you can try to perform them. As in CNS lymphoma we found a low rCBV values with a T1-dominant contrast leakage pattern.
So perfusion weighted image may be helpful in the diagnosis of calvarial lymphoma distinguish it from metastases or meningiomas (Fig.
6).
Differential diagnosis
Diffuse large B-cell subtype NHL diagnosis must be considered in the differential diagnosis in any patient with a painless scalp masses extending through the skull. The differential diagnosis of calvarial NHL includes other soft tissue masses as metastatic cancer,
leukemia,
plasmacytoma,
anaplastic meningioma and sarcoidosis. Ewing sarcoma and Langerhan cell histiocytosis usually occurs in younger patients and can also mimic calvaria lymphoma.
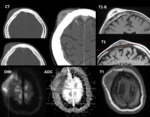
Metastasis
The main differential diagnosis of Skull lymphoma are metastases.
Skull metastases are seen in 20% of all cancer patients.
They have the same range of appearances as skeletal metastases elsewhere,
and in 90% of cases other skeletal metastases were evident in Tc99m-MDP planar skeletal scintigraphy. Solitary skull metastasis may be the only evidence of metastatic disease (11%).
This is particularly the case with renal cell carcinoma and thyroid carcinoma that usually present as expansive lytic lesions.
MR
There is a large semiological overlapping between metastatic lesions and calvarial lymphoma. DWI improves the conspicuity of metastatic lesions over conventional MRI.
Malignant skull lesions generally display lower diffusivity than benign lesions (like intraosseous hemangioma). Skull metastases are a histologically heterogeneous group of lesions that results in a wide range of ADC values with a mean value reported to be 0.99ãôÝã0.34ãûã10ã3 mm2/s.
Consequently,
there is overlap in the ADC values of metastases with other malignant lesions,
such as lymphoma and nasopharyngeal carcinoma.
In addition, metastatic sarcomas generally display lower ADC values than carcinomas. Furthermore,
DWI may be useful for monitoring treatment effects (Fig.10)(Fig.11).
Sarcoidosis
Bone sarcoidosis of the skull is very infrequent.
Osseous sarcoidosis should be considered during the differential diagnosis when evaluating new lytic lesions of the skull in a patient with pulmonary sarcoidosis. Gadolinium enhancement can be diffuse or nodular on post-contrast T1-weighted magnetic resonance imaging (MRI) [Fig.
12 ] Perivascular spread can be encountered,
producing enhancing foci in the brain surface .
Langerhans cell histiocytosis
Represents a spectrum of rare disorders characterised by idiopathic infiltration and accumulation of abnormal histiocytes .
Radiography remains the ãgold standardã of the diagnostic and staging procedure. The X-Ray is a low dose procedure that show the characteristic bevel shaped destruction of both inner and outer skull bone tables (Fig.13).
Multiple Myeloma
Plasma cell neoplasms arise from mature B lymphocytes and include multiple myeloma,
plasmacytoma and WaldenstrûÑm macroglobulinaemia.
Solitary plasmacytoma of the skull is rare entity and has a wide spectrum of pathology,
including a quite benign,
solitary plasmacytoma (SPC),
and an extremely malignant,
multiple myeloma (MM) at the two ends of the spectrum.
Classical skull patterns includes disseminated form: multiple well-defined "punched out" lytic lesions of the skull (Fig.
14),
diffuse lytic lesions of myeloma give rise to the classic ãpepper pot skullã,
diffuse skull osteopenia or solitary focal plasmacytoma: a single large/expansile lesion most commonly in periorbital area. Typical myeloma lesions involve the bone marrow and have low signal intensity on MRI T1W images (Fig.14) and high signal intensity on T2W and STIR sequences.
Meningioma
Meningiomas account for 37% of all primary brain tumors .
Meningioma grows from the arachnoid cells that form the middle layer,
and are firmly attached to the dura.
Because meningiomas tend to grow inward,
they cause local pressure on the brain.
They can also grow outward causing the skull to thicken,
hyperostosis and variable periosteal reaction.
(Fig.15).