Keywords:
Pelvis, Genital / Reproductive system female, CT, Ultrasound, Screening, Cancer
Authors:
C. Crowley, C. Houlihan, J. Barry; Cork/IE
DOI:
10.26044/ecr2019/C-3798
Results
Thirty-four histologically confirmed cases of ovarian cancer were identified.
Eleven of these had to be excluded as they either had no available pre-operative pelvic CT,
or no ovarian mass lesion was demonstrated on their CT imaging.
The average age of the 23 included patients at the time of their histological diagnosis was 56 years (range 17-80 years).
Of the 6 patients who were aged under 50 at the time of their histological diagnosis,
one had the risk factor of Lynch syndrome.
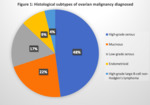
Figure 1 shows the breakdown of histological subtypes of ovarian cancer that the patients were diagnosed with.
The majority (48%) had high-grade serous carcinoma.
Fifty-two percent of the group were found to have bilateral ovarian involvement,
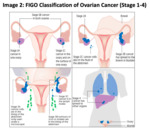
and 65% had advanced disease i.e.
Stage 3 or 4 of the FIGO classification (Figure 2)4.
There was 100% inter-rater agreement regarding the presence or absence of all five of the IOTA M-features on the CT imaging of these patients.
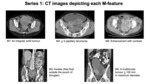
Figure 3 shows examples of CT images depicting each IOTA M-feature.
All patients had at least two M-features on their CT,
with the majority (74%) showing at least three M-features.
One patient’s CT showed all 5 M-features.
Assessing for the third M-feature,
the presence of at least four papillary structures defined as solid projections measuring over 3 mm in height,
proved difficult in some cases due to the poorer resolution of CT for pelvic structures compared with ultrasound.
This did not result in inter-rater disagreement however.
No association was demonstrated between the number of M-features present on CT and the histological subtype that was diagnosed nor stage of disease,
although the ability to assess for this was likely limited by low patient numbers.