Background
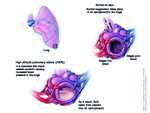
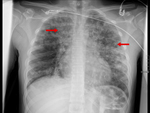
High altitude pulmonal edema (HAPE) is an acute noncardiogenic pulmonary edema caused by patchy hypoxic pulmonary vasoconstriction [1,2]. Typically, this form of pulmonary edema is seen in people who travel from lower elevation to high elevation (>2500 m) and is related to altitude and rate of ascent [3,4,5]. HAPE mainly occurs due to exaggerated hypoxic pulmonary vasoconstriction and elevated pulmonary artery pressure (Fig.1). The estimated incidence in high altitude in our region is about 0.05-0.1%. High altitude pulmonary edema must be considered in acute care units localized in mountain regions, like Himalaya, our alpine regions in the north of Italy and other regions of the world with altitudes above 2000 m. HAPE affects residents of high altitude when they descend to lower altitude and then return to high altitude, too [1]. In our Department we observed only two male patients (Fig. 2,3 and 4) in during the last year, so we tend to misdiagnose the pathology, especially in absent clinical information. In these two cases, an acute pulmonal embolism was suggested. So only the thoracic CT examination after contrast application could exclude thromboembolism.
Etiology
The underlying pathophysiology is a vascular hypoxic pulmonary vasoconstriction (HPV) leading to increased microvascular pressures. The resultant hydrostatic stress causes dynamic changes in the permeability of the alveolar capillary barrier and mechanical injurious damage leading to leakage of large proteins and erythrocytes into the alveolar space in the absence of inflammation [2].
This kind of edema causes a form of consolidation which tends to occur along peribronchovascular bundle and if it is extensive it tends to occur as more mass like areas of opacification occurring with a peribronchovascular distribution. It has been observed that HAPE is a high permeability type of edema occurring also due to leaks in the capillary wall (‘stress failure’). Slow descent is the most effective method for prevention; in addition, graded ascent and time for acclimatization, low sleeping altitudes, avoidance of alcohol and sleeping pills, and avoidance of exercise are the key to preventing HAPE.
Common symptoms are dyspnea, cough, headache, fever, and weakness. Men appeared to be more susceptible than women to high-altitude pulmonary edema [4].
The most important differential diagnosis of high altitude pulmonal edema is pneumonia.
Other important differential diagnoses are acute pulmonary embolism, acute decompensated heart failure, acute coronary syndrome, bronchitis, reactive airway disease, and exercise-associated hyponatremia.
Treatment
Treatment of HAPE consists of immediate improvement of oxygenation either by supplemental oxygen, hyperbaric treatment, or by rapid descent [6]. Pharmacological therapy like Nifedipine, Tadalafil or Dexamethasone are other therapeutic options. Nifedipine is a nonspecific calcium channel blocker that reduces pulmonary vascular resistance and PA pressure and improves PaO2. Tadalafil is a phosphodiesterase-5 inhibitor that augment the pulmonary vasodilatory effects of nitric oxide by blocking the degradation of cyclic guanosine monophosphate. Glucocorticoids can improve the functions of capillary endothelial cells and alveolar epithelial and are indicated in treatment of acute mountain sickness and suspected cerebral edema.
If treated rapidly, HAPE has a good prognosis.
Differential Diagnoses of HAPE
-
Pneumonia
Differentiating HAPE from Pneumonia can be difficult. HAPE may be precipitated by or co-exist with pneumonia and distinguishing between these diagnoses can be challenging. The presence of marked hypoxemia (common with HAPE), extensive infiltrates on chest radiograph, and modest elevations of the white body count frequently influence clinicians treating HAPE to administer antibiotics for the possibility of concomitant bacterial pneumonia. Pneumonia can have different radiological features like extensive infiltrates with or without pleural effusion, lobar consolidations, interstitial infiltrates and/or cavitation. In CT findings reach from tree in bud signs to ground glass opacities and lobar consolidations.
-
Acute pulmonary embolism
Acute pulmonary embolism is another clinical exclusion diagnosis in suspected HAPE, in presence of pulmonary hypertension with or without fever. In this case the only valuable diagnostic is thoracic computed tomography after contrast administration to exclude endoluminal defects in the pulmonal arteries.
Peripheral wedge-shaped pulmonary consolidations are typical parenchymal findings.
-
Acute decompensated heart failure
Radiographic findings can range from mild pulmonary vascular perihilar to marked cardiomegaly and extensive bilateral interstitial markings. Bilateral perihilar alveolar edema causes the typical "bat wing opacities “appearance on chest radiograph. Only mitral insufficiency can cause unilateral cardiogenic pulmonary edema. Other signs on chest radiograph are Kerley B lines, dilated upper lobe vessels and pleural effusion. CT-findings are thickened septal lines due to interstitial edema, ground glass opacity in the dependent part of the lungs and bilateral pleural fluid.