Sheaths, Angiographic Catheters, Guidewires & Embolic Materials
Access sheaths: standard 5Fr or 6Fr sheath are used for co-axial access site. 6Fr are usually needed when balloon occlusion device is anticipated.
Angiographic catheters: 4Fr or 5Fr Cobra C1, Simmons 1 & pigtail. Microcatheter system such as 2.6Fr Progreat TERUMOTM or 1.8Fr Carnelian TOKAITM
Guidewires: 0.035” hydrophilic floppy tip wire TERUMOTM, 0.014” hydrophilic shapable tip microwire TRANSENDTM
Embolic Agents: Gelfoam slurry, Polyvinyl alcohol (PVA) particles (300-500um), Pushable Platinum Coils, Glue-Lipiodol emulsion.
Angioplasty Balloons: Compliant angioplasty balloon such as MUSTANGTM PTA balloon 6mmx 40mm
The equipments listed above are the standard equipments that are often used, more different variations of the devices are available depending on the center of practice. The common femoral arteries are usually punctured under ultrasound guidance for access.
The contralateral internal iliac artery (IIA) is usually cannulated with Cobra C2 catheter and the ipsilateral internal iliac artery can then be cannulated from the same side of the femoral access with a Sim 1 catheter. Single femoral access is often adequate except for cases where bilateral internal iliac temporary occlusion are needed then bilateral femoral access can be performed.
Gelfoam is a water-insoluble haemostatic sponge that expands on contact with fluids, incites foreign body reaction within 2 – 3 weeks and then resolves over several months(1), thus rendering it a temporary embolic agent. Commonly, this is used when temporary haemostasis control is required.
PVA particles occlude small arteries and arterioles with aggregation within the vessel lumen(1). It is commercially available in narrow size ranges but most applications require 300–500um or 500-700um. It is a permanent agent, commonly used in embolisation for uterine fibroids or gynaecological tumours.
Coils & glue are permanent embolic agents. The detailed discussion of these agents is beyond the scope of this article.
Pelvic Arterial Anatomy & Angiographic Views
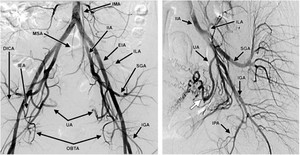
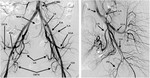
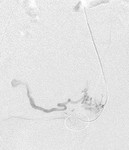
Fig. 1: Pelvic iliac artery anatomy. Adopted from reference(2). Digital substraction angiography (DSA) of the pelvic aorta and the magnified left IIA DSA. DCIA= deep iliac circumflex artery, EIA=external iliac artery, IGA=inferior gluteal artery, ILA=iliolumbar artery, IMA=inferior mesenteric artery, IPA=internal pudendal artery, MSA=median sacral artery, SGA=superior gluteal artery, UA=uterine artery, IIA=internal iliac artery, IEA=inferior epigastric artery.
References: Katz MD et al. (2012) Beyond hemostasis: Spectrum of gynecologic and obstetric indications for transcatheter embolization. Radiographics. 2012;32(6):1713-1731.
Diagnostic flush pelvic aortogram are sometimes performed with a 5Fr pigtail angiographic catheter for an overview of the iliac arterial anatomy prior to any intervention.
Further selective views in anterior oblique 30 – 350 projections are performed for better delineation of the anterior and posterior divisions of the internal iliac artery (IIA).
Obstetric Intervention:
Abnormal Placenta Implantation
Case 1: 27 years old (yo), G2P1 at 36weeks of gestation, antenatal ultrasound (US) showed findings of placenta accreta. Bilateral internal iliac artery balloon occlusion was planned prior to caesarean section.
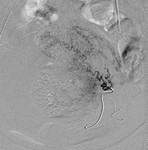
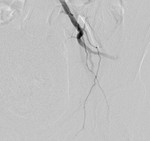
Technique: Both internal iliac arteries (IIA) were cannulated with 4Fr Cobra C1 through bilateral femoral artery access sites. MUSTANGTM PTA balloon size 6mmx40mm placed with test inflation done to confirm adequate occlusion.
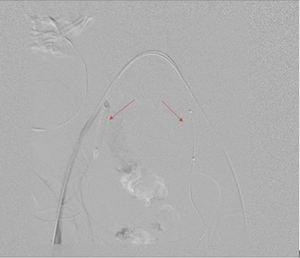
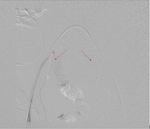
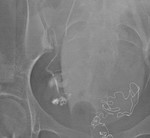
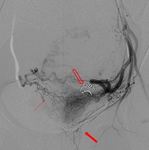
Fig. 2: Inflated PTA balloons (arrows) during test inflation showing no flow to the internal iliac arteries.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: PTA balloons were inflated after delivery of the newborn. Placenta increta diagnosed intra-operatively but complete placenta removal was achieved. Minimal blood loss. Sheath and balloon removed after surgery. Patient had an uneventful recovery.
Post-partum Haemorrhage
Case 2: 35yo, massive post-partum haemorrhage secondary to uterine atony and genital laceration post caesarean section. Patient was still bleeding despite hysterectomy and bilateral internal iliac artery ligation.
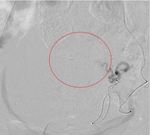
Technique: Right IIA cannulated with 4Fr Cobra C1, superselective cannulation of right internal pudendal artery with 1.8Fr Carnelian microcatheter & 0.014” TRANSENDTM microwire via left common femoral artery access. Active bleeder embolised with Glue-lipioidol emulsion. Anterior division of right IIA embolised with Gelfoam prophylactically.
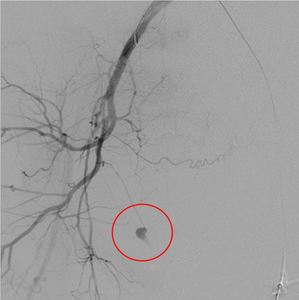
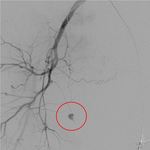
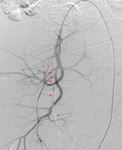
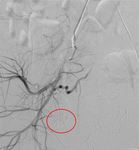
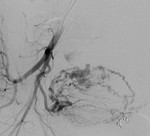
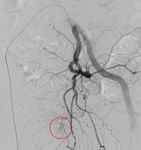
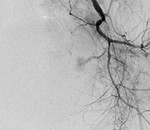
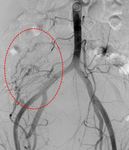
Fig. 3: Right IIA run showing active contrast extravasation (red circle) from a tiny side branch of the right internal pudendal artery.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
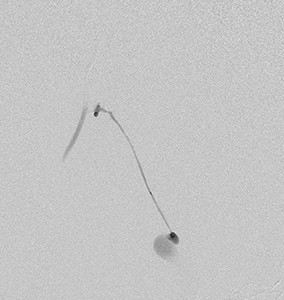
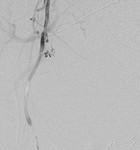
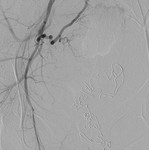
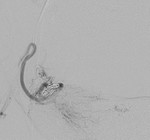
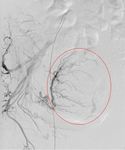
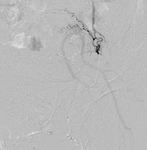
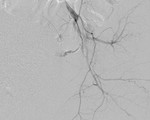
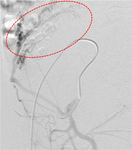
Fig. 4: Superselective cannulation of the tiny side branch of the internal pudendal artery with the active bleeder.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
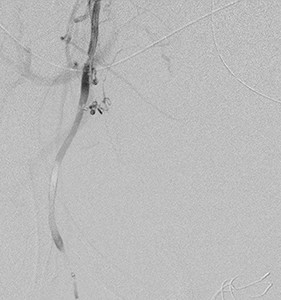
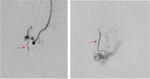
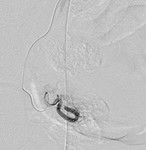
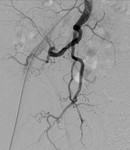
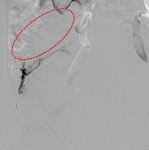
Fig. 5: Post embolization with glue emulsion. Run showed complete occlusion of the side branch.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
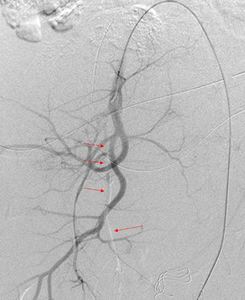
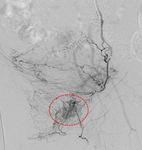
Fig. 6: Post gelfoam embolization of the anterior division of the right IIA for further temporary secure of haemostasis. Post embolization run showing complete truncation of the anterior division of right IIA (red arrows).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Patient had no clinical signs of bleeding post embolization with recovery of haemoglobin levels.
Case 3: 32yo, post vaginal delivery complicated with vaginal tear, primary team was unable to secure bleeding.
Technique: Bilateral IIAs were cannulated with 4Fr Vert & SIM1 catheter via left common femoral access, followed by superselective cannulation of the right uterine and vaginal artery with 2.7Fr Progreat microcatheter and 0.014” TRANSENDTM guidewire. Active bleeder embolised with glue-lipiodol emulsion and anterior trunk of the right internal iliac artery was embolised prophylactically with gelfoam slurry.
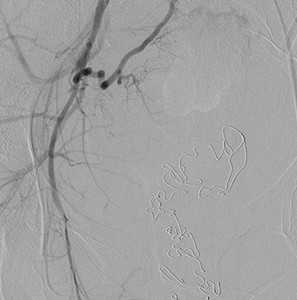
Fig. 7: Initial right IIA run showing no obvious contrast extravasation or blush.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
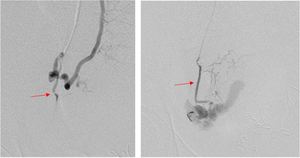
Fig. 8: Subsequent cannulation of right uterine artery unveiled a tiny suspicious branch of right vaginal artery (red arrow) which confirmed active bleeding (red arrow) on further ultraselective cannulation of this branch.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
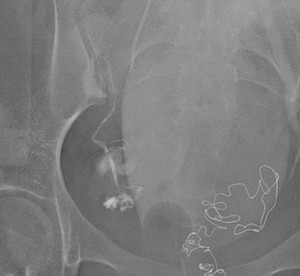
Fig. 9: Post embolization with Glue-lipiodol emulsion in acquired image
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
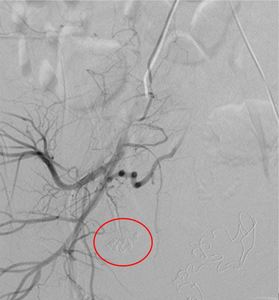
Fig. 10: Post embolization run show complete occlusion of the right vaginal artery (red circle) branching from the right uterine artery. Bilateral anterior trunk of internal iliac arteries bilaterally embolised prophylactically as well (images not shown).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Bleeding stopped post embolization. Patient had an uneventful recovery.
Ectopic Pregnancy – Extra-uterine Abdominal Pregnancy
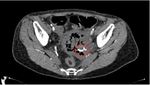
Case 4: 28yo, had abdominal pregnancy with fetal demise detected late at late 2nd trimester. Computed tomography (CT) of the abdomen was performed and interventional radiology team was called in for uterine artery embolization prior to explorative laparotomy in anticipation of severe intra-operative haemorrhage.
Technique: Both IIAs were cannulated with 4Fr Cobra C1 catheter followed by selective cannulation of the bilateral uterine arteries with 2.7Fr Progreat microcatheter. Both uterine arteries were embolised with platinum coils of varying sizes and length until flow stasis was achieved.
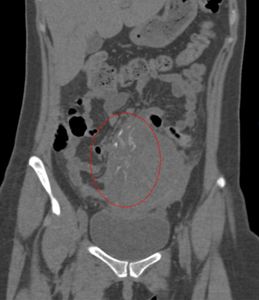
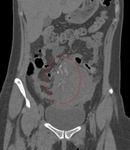
Fig. 11: Plain CT abdomen in coronal view show a heterogenous pelvic mass with fetal parts within (red dotted circle).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
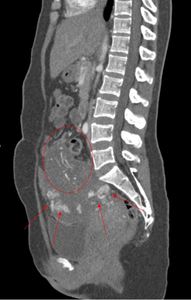
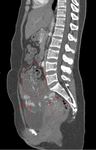
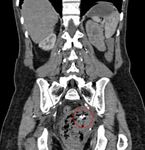
Fig. 12: CT angiogram of the abdomen in sagittal view showing the distinct pelvic mass with fetal parts(red dotted circle) locating outside of the uterus, superior to the uterine fundus and urinary bladder. The abnormal vasculature within may be part of the placental tissues (red arrows).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
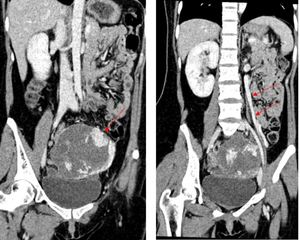
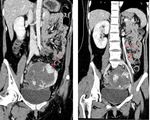
Fig. 13: Portovenous phase of CT Abdomen in coronal view showing an abnormally dilated left ovarian vein (red arrows) draining from the fetal pelvic mass suggestive of either an ovarian origin or arteriovenous fistula within the fetal/placental tissue.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Fig. 14: Anterior trunk of left IIA run showing the abnormal vasculature of the pelvic ectopic pregnancy arising from the left uterine artery with drainage to the left ovarian vein.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
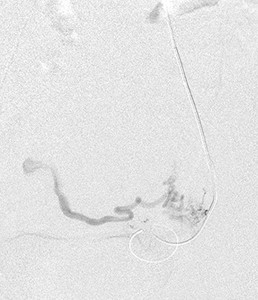
Fig. 15: Selective cannulation of the left uterine artery as distal as possible to avoid the supply to the normal uterus and vaginal branches.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
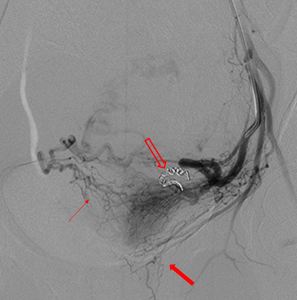
Fig. 16: Post embolization with platinum coil (hollow broad red arrow) run showed occlusion of the left uterine artery with opening of the inter-uterine collaterals (thin red arrow) supplying the ectopic pregnancy. The normal supply to the uterus is preserved, vaginal branches are visualized now and preserved (broad red arrow).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
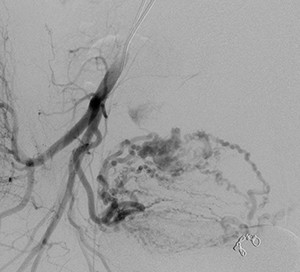
Fig. 17: Right IIA run showing the other part of the ectopic pregnancy’s abnormal vasculature with supply from the right uterine artery.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
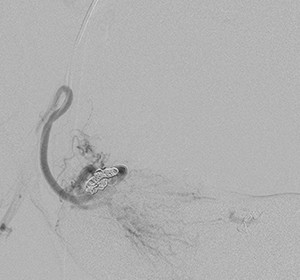
Fig. 18: Post embolization with platinum coil run show occlusion of the uterine supply to the abnormal vasculature with preservation of the uterine branches supplying the normal uterus.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Patient had her extra-uterine non viable pregnancy removed. Blood loss was minimal. No significant involvement of bowels or urinary bladder noted intraoperatively. Patient had an uneventful recovery after the surgery.
Gynaecologic Intervention:
Bleeding due to gynaecological malignancy (cervical carcinoma & endometrial carcinoma)
Case 5: 42yo, advanced endometrial carcinoma with concurrent pulmonary embolism, had persistent per vaginal bleeding resultant in anaemia despite on palliative radiotherapy. Therefore, primary team was unable to start her on anti-coagulation. Uterine artery embolization was performed to control the bleed.
Technique: Bilateral IIAs were cannulated with 4Fr Cobra C1 catheter, followed by selective cannulation of both uterine arteries and superselective cannulation of the thesmaller supplying branches to the tumour with various 1.8Fr Carnelian & 2.6Fr Progreat microcatheter system and 0.014” TRANSENDTM microwire. Embolisation performed with 355 – 500um PVA particles and gelfoam slurry.

Fig. 19: Left IIA run showing a large tumoural blush at the midpelvis with supply from the prominent left uterine artery.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
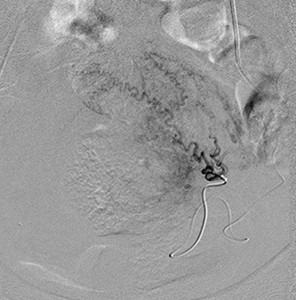
Fig. 20: Superselective cannulation of the smaller distal branches supplying the tumour from the left uterine artery.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
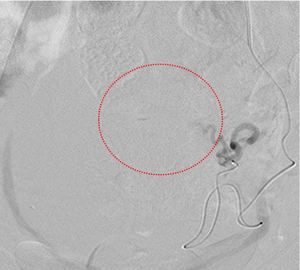
Fig. 21: Post embolization with PVA particles run showing reduction in tumoural blush (red dotted circle).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
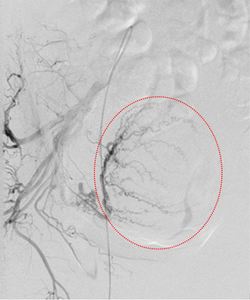
Fig. 22: Right IIA run showing a large tumoural blush (red dotted circle) with supply from a dilated tortuous right uterine artery.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
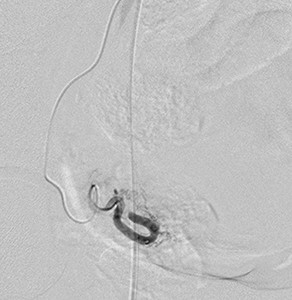
Fig. 23: Post superselective cannulation of smaller supplying uterine branches to the tumoural blush followed by PVA particle and gelfoam embolization. Run showed significant reduction of the tumoural blush.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Significant reduction in tumoural blush was achieved. Her per vaginal bleeding was controlled. Subsequently, the gynaeoncology team was able to put her back on anticoagulation for treatment of pulmonary embolism.
Case 6: 68yo, advanced cervical carcinoma with severe per vaginal bleeding.
Technique: Bilateral IIAs were cannulated with 4Fr Cobra C1 catheter, followed by selective cannulation and superselective cannulation of the cervicovaginal branches supplying the tumour. Embolisation performed with 355 – 500 um PVA particle and gelfoam slurry.
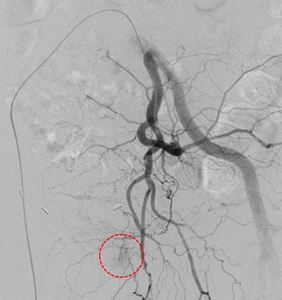
Fig. 24: Left IIA run showing small tumoural blush (red circle) with tiny supplying vessels from the presumably cervicovaginal branches.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
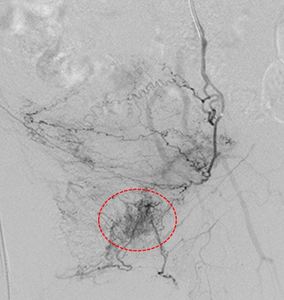
Fig. 25: Superselective cannulation of the tiny cerviovaginal branches with better delineation of the tumoural blush (red circle).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
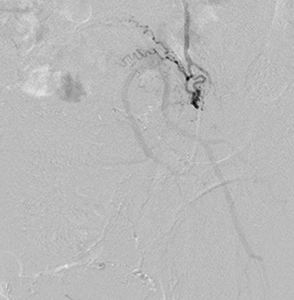
Fig. 26: Post embolization with PVA particles and gelfoam emulsion run showing complete obliteration of the tumoural blush.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
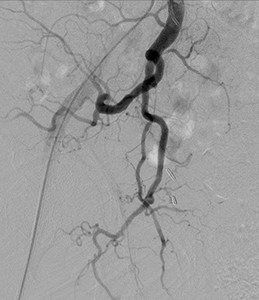
Fig. 27: No demonstrable tumoural blush from the right IIA.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Symptom was controlled and patient continued her follow-up under gynaeoncology.
Case 7: 43yo, another patient with recurrent cervical carcinoma complicated with uncontrolled per vaginal bleeding.
Technique: Bilateral IIAs were cannulated with 4Fr Cobra C1 catheter, followed by selective cannulation of the left uterine artery and superselective cannulation of the smaller branches supplying the tumour. Embolisation performed with gelfoam slurry.
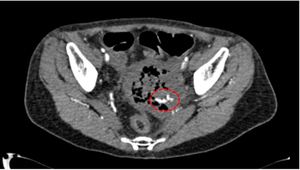
Fig. 28: CT angiogram of the abdomen in coronal (Fig 29) and axial view (Fig 28) showing contrast blush (red circle) within the vaginal packing adjacent to the cervical mass which persist with dispersal on delayed 3 minutes (not shown) indicative of active haemorrhage.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
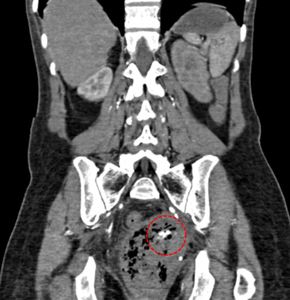
Fig. 29: CT angiogram of the abdomen in coronal (Fig 29) and axial view (Fig 28) showing contrast blush (red circle) within the vaginal packing adjacent to the cervical mass which is persistent with slight dispersal at delayed 3 minutes scan(not shown) indicative of active haemorrhage.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
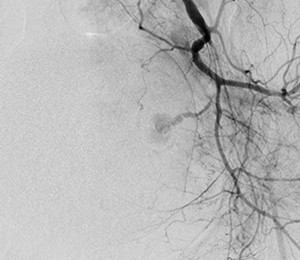
Fig. 30: Left IIA run showing focal contrast blush corresponding to the findings on CT angiogram arising from a side branch of the anterior division of the left internal iliac artery.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
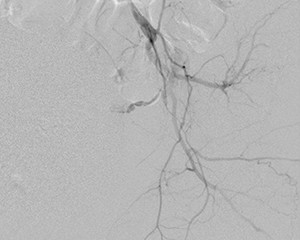
Fig. 31: Superselective cannulation of the tiny branch attributing to the contrast blush. Some reflux to the posterior division.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
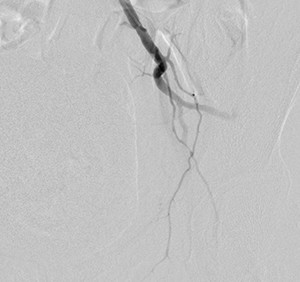
Fig. 32: Post embolization with gelfoam showing resolution of the contrast extravasation.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Per vaginal bleeding was controlled and continued her follow-up under gynaeoncology team.
Uterine Fibroids
Case 8: 43yo, Para 1, has large uterine fibroid which does not respond to intramuscular GnRH inhibitor (Lucrin).
Technique: Bilateral IIAs were cannulated with 4Fr Cobra C1 catheter, followed by selective cannulation of both uterine arteries and superselective cannulation of the smaller supplying branches to the fibroid with 2.7Fr Progreat microcatheter. Embolisation performed with 355 – 500um PVA particles and gelfoam slurry.
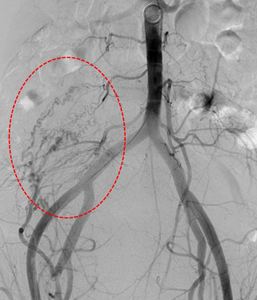
Fig. 33: Flush pelvic aortogram showing large fibroid blush (red circle) at the right lower abdomen.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
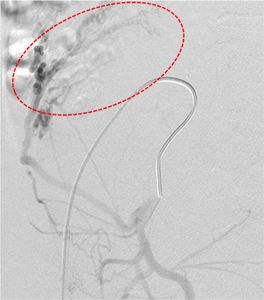
Fig. 34: Anterior division of right IIA run showed ascending uterine arterial branches (red circle) supplying the large fibroid.
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
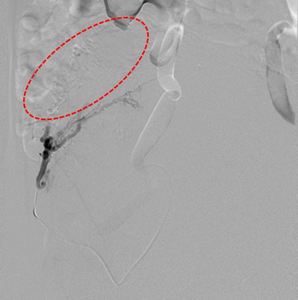
Fig. 35: Superselective cannulation of the ascending uterine arterial supply with post embolization with PVA particles and gelfoam showing significant occlusion of the supply (red circle).
References: Department of Radiology, Sarawak General Hospital – Sarawak/MY
Outcome: Her repeat MRI pelvis showed reduction in the size of tumour.
Others – adenomyosis, pelvic congestion syndrome & uterine arteriovenous malformation.
Endovascular treatments are also infrequently performed for these conditions with few publish case reports in the literature, such as in the case of uterine AVMs[3], and pelvic congestion syndrome[4].