Musculoskeletal Complications of Hemophilia
In severe hemophilia, 90% of bleeding episodes involve the MSK system, and in 80% of cases, the joints are particularly affected (Figure 12).
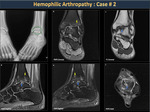
These hemorrhages are spontaneous, without apparent cause and usually affect one joint at a time. The frequency and location of bleeding vary with age; Knees and elbows are most often affected in people over 30 years and in adolescents, the ankles are more compromised (figure 13).
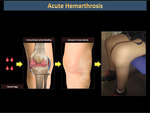
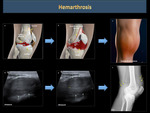
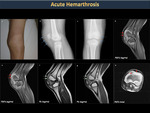
Acute hemarthrosis
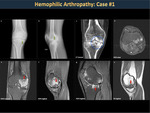
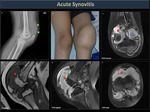
In hemophilia, the onset of pain and local discomfort are the most common signs that indicate bleeding has begun. (Figures 14, 15, 16).
Subacute hemarthrosis
Subacute hemarthrosis arises after repeated episodes of hemarthrosis have occurred in the same joint. At this stage, the joint presents incomplete recovery.
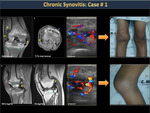
Chronic arthropathy
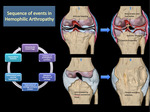
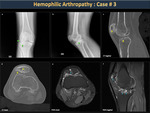
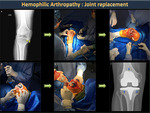
Repeated episodes of hemarthrosis generate chronic synovitis with progressive joint destruction, known as hemophilic arthropathy (Figure 17). In the first stage, there is articular hypertrophy due to chronic synovitis and effusion. Afterward, epiphyseal hypertrophy deforms the joint and limits the range of motion.
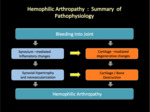
Pathophysiology of hemophilic arthropathy
The absence of tissue factor in joints and muscles explains the articular tropism of bleeding in these patients.
The pathological mechanism in the development of arthropathy is complex. It is likely to be multifactorial and involves cartilage degradation and synovial inflammation due to the harmful effects related to bleeding (Figure 18).
More than 80% of hemarthrosis occurs in the knee, elbow and ankle. The joints that bleed frequently are the most affected by chronic arthropathy (Figures 19,20,21).
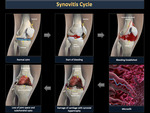
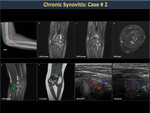
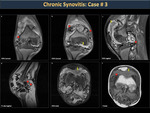
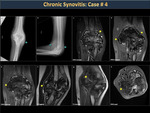
Synovitis (Figure 22)
The synovial is a very vascularized structure that has abundant lymphatic and nerve endings.
Blood accumulates in the joint and should be treated ideally within two hours, otherwise, the synovium becomes inflamed due to deposits of degradation and iron products that are toxic to the bones, cartilage and synovial (Figure 23).
Repetitive bleeding in the same joint generates chronic inflammation with synovial thickening and digital projections called microvilli appear, which make the membrane more prone to impingement by bone structures and perpetuate the bleeding. Subsequently, subchondral cysts appear with bone loss and reduced joint mobility. (Figures 24,25,26,27).
Orthopedic surgery
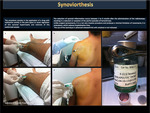
Repeated hemarthrosis in a joint, with the risk of synovitis and chronic arthropathy, justifies synovectomy or synoviortesis.
Synoviortesis consists in injecting a chemical or radioisotopic product into the joint (Figure 28), facilitating the formation of fibrous tissue that inhibits vascular proliferation and reduces the risk of bleeding.
Surgical synovectomy consists of performing a more complete surgical excision of the synovial membrane.
Total knee replacement has become the treatment of choice for patients with severe knee arthropathy, as it eliminates pain and corrects deformities (Figure 29).
Muscular complications: hematomas (Figure 30)
Muscle hematomas represent 10% of hemorrhages in patients with severe hemophilia.
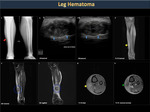
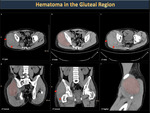
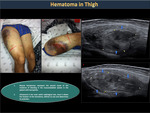
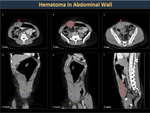
Subcutaneous hematomas (Figure 31) rarely grow large due to the limited space available. In contrast, hematomas on large muscles, such as the gluteal region or the thigh (Figures 32,33) reach a large size by being in an expandable space.
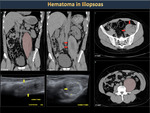
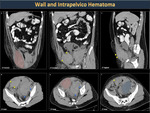
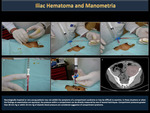
Iliopsoas hematomas (Figure 34) initially produce inguinal pain and sometimes the diagnosis is made when femoral nerve compression or severe anemia are observed. Hip flexion contracture and a positive iliopsoas sign may indicate bleeding in the hip, rectus femoris muscle or the anterior abdominal wall (Figure 35,36).
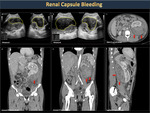
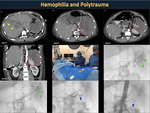
Having hemophilia increases the possibility that a physical impact, even of low resistance, on the spleen, liver, kidneys, intestine or pancreas can cause pericapsular bleeding that progresses to an expanding hematoma (Figures 37,38).
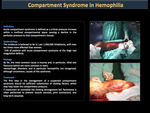
Compartment syndrome in hemophilia (Figure 39)
It was first described by Richard von Volkmann in 1881.
Compartment syndrome is well described in people with hemophilia where hemorrhages located in the calf and forearm represent the greatest risk for its development.
The first step in the management of compartment syndrome is the replacement of coagulation factors, and if this fails, fasciotomy should be considered (figures 40).
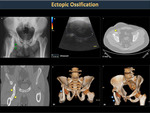
Heterotopic ossification (Figure 41)
The specific pathophysiology is not clear. Several causes of this pathology are recognized.
A common site for its development is the hip (figure 42).
The signs and symptoms of which these patients complain will begin 1–3 months after a precipitated injury.
A patient will usually have a positive bone scan within 2 to 4 weeks after the start of their development.
An x-ray will not see new bone formation until 3 to 6 weeks after its formation.
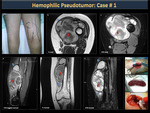
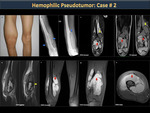
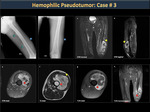
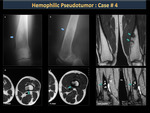
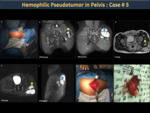
Hemophilic Pseudotumor (figure 43)
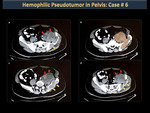
Hemophilic pseudotumors are heterogeneous hematomas with a hypointense, chronic and slowly expanding fibrous capsule that occurs frequently in soft (intramuscular) but occasionally subperiosteal tissues. Pseudotumors that occur in muscles with wide tendon insertions progress easily and cause erosion due to severe pressure from the adjacent bone (Figures 44,45,46,47). The most affected bones by pseudotumors are the femur, the pelvis (Figures 48,49), the tibia and the bones of the hand.
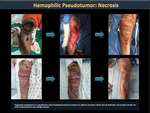
Bones can be destroyed, and muscles and skin often compress and may suffer from necrosis (Figure 50).