INTRODUCTION (Figure 1)
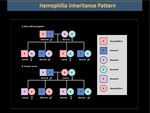
Hemophilia is an inherited bleeding disorder linked to the X chromosome caused by a deficiency in coagulation factor VIII, for hemophilia A, and factor IX, for hemophilia B.
Approximately 85% of patients with hemophilia suffer from hemophilia A, and 15% of hemophilia B.
The varying degrees of deficiency of factor VIII or factor IX defines the disease form as mild, moderate or severe. Severe hemophilia is characterized by basal levels of factor VIII or factor IX of less than 1%, moderate hemophilia at baseline levels between 1% and 5%, and mild hemophilia at baseline levels between 6% and 40%.
Plain radiography
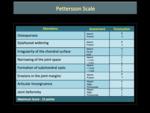
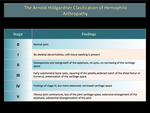
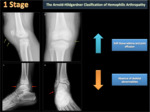
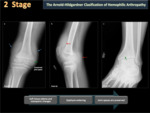
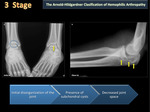
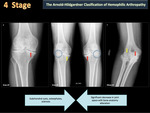
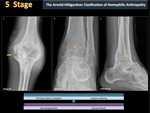
There are two main classification systems used to qualify hemophilic arthropathy (HA) on simple radiography; these are the scale of Arnold Hilgartner and Pettersson scale. The Arnold Hilgartner system is a progressive scale of arthropathy (Figure 2). The Pettersson's score is an additive scale (Figure 3) in which each anomaly is rated from 0 to 1 or 2 and where the highest score for an individual joint is 13, indicating a destroyed joint. While the progressive system is easy to use (Figures 4,5,6,7,8), the additive is more meticulous, but it better discriminates the different stages of HA, without evaluating soft tissue changes.
Ultrasound
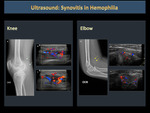
Ultrasound is useful for the assessment of changes in soft tissue and joint effusions in acute episodes.
The normal synovial membrane is thin, barely seen in ultrasound; when it becomes inflamed, diffuse or if there’s nodular thickening observed, it shows an increase in vascular flow in Doppler ultrasound (Figure 9).
MRI
No exact recommendations of the sequences to be performed in hemophilic arthropathy have been established. A T1 sequence is useful for demonstrating anatomy and osteochondral lesions, and STIR or T2FS sequences are sensitive to demonstrate bone edema.
T2 * GRE techniques give greater visibility of blood products in the acute and chronic stages.
Detailed images of the cartilage can be obtained with a PDFS sequence or a 3D-SPGR sequence.
Intravenous contrast is generally not recommended in the evaluation of arthropathy.
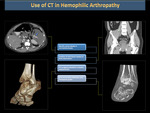
CT
The cross-sectional imaging capability of CT, combined with its high spatial resolution, offers an attractive alternative, which also helps us as a therapeutic guide.
Contrast CT helps to determine the leakage of the contrast dye in case of suspected active bleeding and helps to define interventional therapy as embolization (Figures 10, 11).