Keywords:
Performed at one institution, Diagnostic or prognostic study, Retrospective, Cancer, Calcifications / Calculi, Diagnostic procedure, Comparative studies, Biopsy, Ultrasound, MR, Mammography, Oncology, Breast
Authors:
L. Kovačević, S. Barsic Ostojic, L. Korsa, Z. Marusic, M. Prutki; Zagreb/HR
DOI:
10.26044/ecr2020/C-03848
Purpose
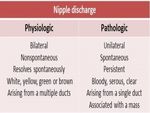
Nipple discharge (ND) is one of the most commonly reported complaints related to the breast for which women seek advice from physicians [1]. The vast majority of these reported cases are of benign origin [2]. Clinically, ND can be classified either as physiologic or pathologic (pND). Clinical characteristics of pathologic and physiologic nipple discharge are listed in Table 1.
pND is often described as being unilateral, bloody or serous, persistent, spontaneous, associated with a mass and arising from a single duct [3-5]. Unlike physiologic ND, clinical diagnosis of pND should always lead to additional diagnostic evaluation due to the associated increased risk of malignancy with an incidence of up to 21.3% [5]. Furthermore, pND is most commonly caused by papilloma or benign duct ectasia, but can also suggest malignancy [6].
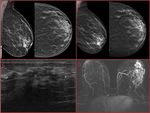
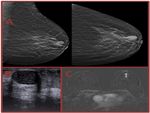
Initial diagnostic approach in the evaluation of pND includes mammography (MMG) and ultrasound (US) [3,7]. Although magnetic resonance imaging (MRI) is not a part of the initial evaluation, it is recommended in the assessment of pND if MMG and US results are negative [8,9]. Illustrative examples of the imaging features of patients with pND are shown in Fig. 1 and Fig. 2.
To the best of our knowledge, there were no reports published on the diagnostic performance of digital breast tomosynthesis (DBT) in the evaluation of pND.
Therefore, the goal of this study is to determine the diagnostic performance of DBT in the assessment of patients with ND and to compare it with MMG, US and MRI.