Anatomical aspects
The knowledge of the arterial anatomy of the district is essential to choose the right point of puncture.
The radial artery is one of two continuations of the brachial artery, the other being the ulnar artery. It supplies the anterior compartment of the forearm. The radial and ulnar arteries originate as a bifurcation of the axillary artery in the cubital fossa and serve as the major perforators to the forearm. Following its bifurcation, the radial artery runs along the lateral aspect of the forearm between the brachioradialis and flexor carpi radialis muscles. Immediately proximal to the wrist, it splits into the superficial and deep palmar branches forming an anastomosis with the distal branches of the ulnar artery in the hand. The radial artery is quite superficial. It is easily palpated proximal to the wrist crease immediately lateral to the tendon of the flexor carpi radialis muscle.
An ultrasound exam may be fundamental in order to assess the diameter of the radial artery and to exclude the presence of unfavourable variants such us the high bifurcation of the radial artery. It is essential to rule out the presence of loop, tortuosity or coiling.
Patient selection
A correct evaluation of indications and contraindications is essential to perform radial artery access. Mainly, radial artery access is indicated in patients with coagulation disorders, obese patients, and on the basis of patient predilections if no technical obstacles are present. This vascular access should be always considered when traditional routes are not available or in case the pushability provided with this kind of access may be helpful.
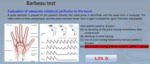
Barbeau-test and measurement of radial artery(>2mm) are crucial steps. Barbeau test is a useful and simple test to verify the patency of the ulnoradial pathway and adequate collateral perfusion to the hand. A pulse oximeter is placed on the patient's thumb, the radial pulse is identified, and the waveform is analyzed. The radial artery is then compressed, and the pulse-oximeter waveform is again analysed for up to 2 minutes and graded. Ulnopalmar patency includes the following 4 types: (A) no damping of the pulse tracing immediately after compression,(B)damping of pulse tracing,(C)loss of pulse tracing followed by recovery within 2 minutes,and (D) loss of pulse tracing without recovery within 2 minutes (Fig1). It is essential to consider as contraindication also the presence of AVF or graft, past upper limb trauma, previous major surgery to forearm or wrist, skin infection or compromised integrity, severe vasospasm, atherosclerotic or calcified PAD, prothesis, vasculitis.
Room setting and Procedural flowchart
The left approach is preferred, even if there is a lack of general consensus. It allows to avoid the brachiocephalic trunk during the navigation and to reduce stroke risk; there is a shorter distance to the visceral vessel (15cm of track saved – anatomy of the aorta); the arm is abducted at 45 or 90 degrees. This position allows to use the not dominant hand of the patient in most of the cases and the operator may use his right hand for fine movements just like in femoral access. Moreover, the operator distance from the x-ray beam is considered acceptable. Angio-suite is prepared with special attention to radioprotection of the operator (Fig 2-3).
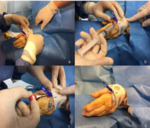
The procedure starts with two crucial moments: informed consent and radial artery evaluation. Risks and benefits of the procedure are described to the patients (special focus on spasms, pain, risk of occlusion, risk of bleeding and hematoma). Barbeau test and US evaluation are essential to avoid D pattern of Barbeau test and diameter. After the radial artery puncture, the arterial administration of the spasmolytic cocktail is helpful to avoid spasms and reduce pain(Fig 4-5).
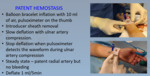
Dedicated material should be used and chosen properly on the base of the procedure target. At the end of the procedure, the sheath is removed and the patent haemostasis protocol is instituted (Fig 6-7)
Learning curve
Incremental improvements in technical success and safety are observed in the initial 200 procedures for most operators compared to highly experienced operators. The suggestion is to start with the easiest patient and to improve US skills in vessel puncture performing PICC insertion or arterial blood gas test.
As operator experience increases, higher-risk patients and more technically complex cases are selected for transradial access. A learning curve of 40 cases is estimated for transradial access and improvements continue after the initial learning curve is overcome(volume-outcome relationship).