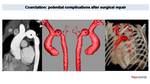
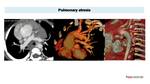
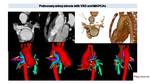
In this work we review the key imaging CT findings of different CHD focusing on 3D imaging reconstructions.
We organize imaging findings depending on the anatomical location for a systematic evaluation.
Aorta
Coarctation
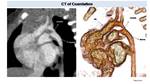
Coarctation of the aorta represents a congenital narrowing of the aortic arch Fig. 4
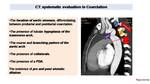
CT can define Fig. 5:
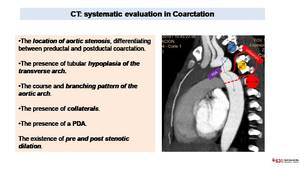
Fig. 5: CT: systematic evaluation in Coarctation
References: Hospital Sant Joan de Deu, Barcelona
CT can assess associated CHD, key in the management of these patients Fig. 6, Fig. 7.
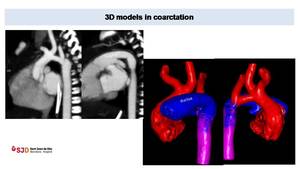
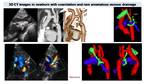
Fig. 6: Preductal coarctation in newborn, low dose CT (0,3 mSV). MPR images (images on the left) shows a large vascular structure probably corresponding to a ductus arteriosum.
3D model (images on the right) depicts better than MPR or VR images the anatomy of the aortic arch (in red), the course of carotid and subclavian arteries and the presence of a large ductus arteriosum (in blue). All these information are key for a correct surgical planning.
References: Hospital Sant Joan de Deu, Barcelona
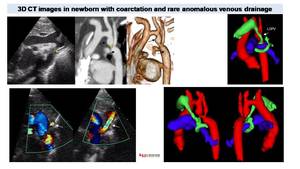
Fig. 7: Coarctation in newborn. Echocardiography shows preductal coarctation (*) and the presence of an anomalous vessel (white arrow). CT with MPR and VR reconstructions better shows pre and post stenotic dilation of the aorta (arrows). 3D model depicts an anomalous drainage (vessel in green) of the left superior pulmonary vein (LSPV), with a rare course surrounding ipsilateral pulmonary artery.
References: Hospital Sant Joan de Deu, Barcelona
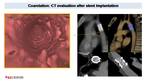
CT represents the best noninvasive technique for the evaluation of coarctation treated with intravascular stents Fig. 8.
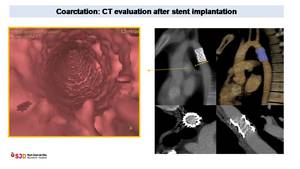
Fig. 8: Coarctation treated with stent implantation. MPR and VR images depict a vascular permeable stent in the aortic isthmus. Virtual endoscopic images (orange border) confirm the absence of re-stenosis.
References: Hospital Sant Joan de Deu, Barcelona
Even more can depict post surgical complications Fig. 9, Fig. 10.
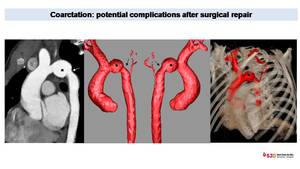
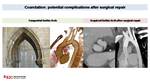
Fig. 9: Control in twelve years old patient with bicuspid aortic valve and coarctation treated with surgical repair. MPR and 3D Model images demonstrate an aneurysm (*) in the transverse aortic arch and a moderate re-stenosis in the isthmus (arrows). Both are rare but potential complications after surgical repair.
References: Hospital Sant Joan de Deu, Barcelona
Interrupted aortic arch
It is a rare form of coarctation characterized by the lack of luminal continuity between ascending and descending aorta Fig. 11
CT can define
- The level of aortic obstruction.
- The presence of the PDA.
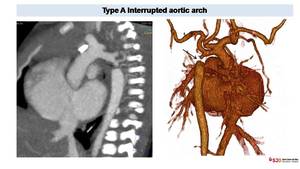
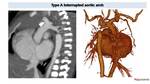
Fig. 11: Interrupted aortic arch in newborn with cyanosis. CT easily depicts the location of aortic interruption (arrows) better define in VR reconstructions. The interruption is located after left subclavian artery ostium, representing a type A in the Celoria-Patton classification.
References: Hospital Sant Joan de Deu, Barcelona
Aortic pseudocoarctation
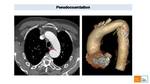
Aortic pseudocoarctation is characterized by kinking of the aortic arch at the level of the ligamentum arteriosus without a pressure gradient or collaterals Fig. 12.
Vascular rings
Left aortic arch with an aberrant right subclavian artery (ARSA)
In this anomaly the right subclavian artery is the last branch off the aortic arch, crossing behind the trachea and esophagus to reach the right arm Fig. 13.
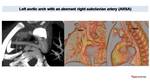
Right aortic arch anomaly with an aberrant left subclavian artery (ALSA)
In this anomaly arteries present a mirror distribution compared with ARSA Fig. 14 Fig. 15. A left-sided arterial duct or ligamentum completes the vascular ring.
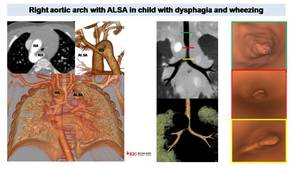
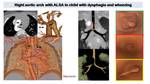
Fig. 14: Vascular ring in child with dysphagia and wheezing.
Low dose CT (0,3 mSV) shows a right aortic arch (RA) and a retroesophagic left subclavian artery (ALSA) with proximal dilation corresponding to Kommerell diveticulum (KD). VR and MinIP reconstructions demonstrate tracheal stenosis due to aortic and ALSA compression. Virtual endoscopic images (on the right) depict luminal tracheal stenosis above the carina.
References: Hospital Sant Joan de Deu, Barcelona
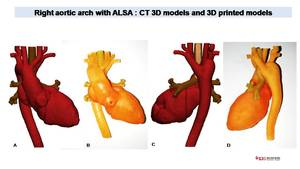
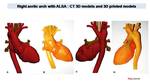
Fig. 15: Same patient with ALSA than figure 14
CT allows generate accurate 3D models (A,C) for analysis of complex cardiac or vascular anatomy. 3D models can be printed (B,D) for pre-surgical evaluation or to evaluate potential use of cardiac and vascular devices.
References: Hospital Sant Joan de Deu, Barcelona
Cervical aortic arch (CAA)
CAA is characterized by an elongated aortic arch with a retroesophageal descending aorta.
Circumflex aorta (CxA)
This anomaly is extremely rare and is characterized by an aortic arch that passes the midline posterior to the esophagus.
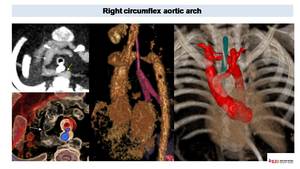
Fig. 16: Right circumflex aortic arch.
Axial CT images defines a right aortic arch with coarctation (arrows), that passes the midline posterior to the esophagus (yellow arrow). VR sagittal images evidence no tracheal stenosis (airways in pink). 3d model demonstrates the posterior course of the aortic arch (Arch) and its relationship with the esophagus (in green). We can also appreciate a posterior left subclavian artery (LSA) and a left descending aorta (DA).
References: Hospital Sant Joan de Deu, Barcelona
Double aortic arch (DAA)
The DAA is characterized by the presence of two aortic arches arising from a single ascending aorta Fig. 17.
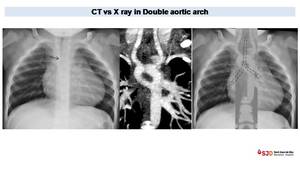
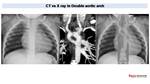
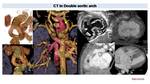
Fig. 17: Double aortic arch in one year old patient with TOF and a Complete Atrioventricular Canal Defect (CAVC).
Chest X ray shows a stenosis of distal portion of the trachea (arrow). Aortic arch in not well visualized and descending aorta is medialized. CT with coronal reconstructions confirm the presence of a double aortic arch generating a complete vascular ring with two symmetric aortic arches that encircle the trachea and the esophagus as shown in the superposition of CT and X ray con the right.
References: Hospital Sant Joan de Deu, Barcelona
DAA represents the most common cause of a symptomatic vascular ring Fig. 18.

Fig. 18: Double aortic arch in one year old patient with TOF and a Complete Atrioventricular Canal Defect (CAVC).
VR images better define the double aortic arch generating tracheal (T)and esophagic stenosis (E) and proximal esophagic dilation (yellow arrow). Cardiac chamber can also be studied and CAVC, right ventricle stenosis (S) and interventricular communication (IVC) can be define (no as better than in echocardiography because is not a cardiac gated study).
References: Hospital Sant Joan de Deu, Barcelona
The right arch is typically larger and the left, may be hypoplastic or atretic Fig. 20.
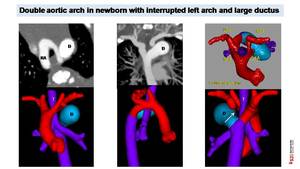
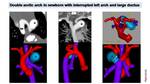
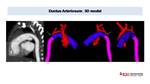
Fig. 19: Suspected Double aortic arch in newborn.
Low dose CT (0,3 mSV) shows double aortic arch with dominant right arch (RA). 3D model images demonstrate four artery sign and an interrupted left aortic arch (arrow) with the presence of a big ductus (D) contributing to trachea (T) and esophagic stenosis. LA: left arch. LSA: left subclavian artery, RSA right subclavian artery, LC: left carotid artery, RC right carotid artery.
References: Hospital Sant Joan de Deu, Barcelona

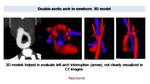
Fig. 20: 3D model in patient with double aortic arch helped in diagnose left arch interruption (arrow), not visualized in CT image on the left.
References: Hospital Sant Joan de Deu, Barcelona
3D mages can be useful in post-surgical evaluation Fig. 21.
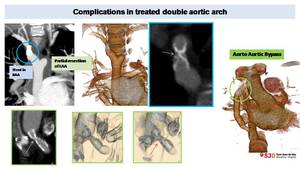
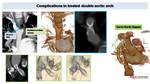
Fig. 21: Complicated DAA in ten years old patient.
Right arch, treated with stent implant for coarctation, shows stent severe stenosis (blue contours image, arrow). Aorto-aortic bypass was realized. Later stenosis of the proximal portion of this bypass was also treated with intraluminal stent (green circle). Successive CT control show stent severe stenosis (green images, arrows).
References: Hospital Sant Joan de Deu, Barcelona
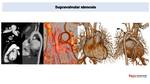
Supravalvular stenosis
It is a focal narrowing of the aorta starting at the sinotubular junction. It is a rare condition, generally associated with Williams syndrome Fig. 22.
Aorto-pulmonary window (AP window)
AP window is a rare anomaly that represents a communication between the main pulmonary artery and the ascending aorta.
CT evaluates: Fig. 23
- The presence of both aortic and pulmonary valves.
- The location and size of the AP window.
- Differentiate AP window from truncus arteriosum.
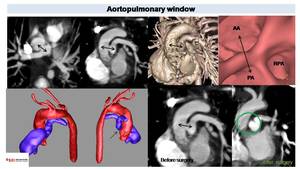
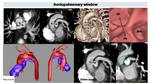
Fig. 23: CT in two years old patient with TOF.
We can appreciate a communication between main pulmonary artery (PA) and ascending aorta (AA) (Black arrows) corresponding to aortoplmonary window. VR and endoscopic images shows vessel distribution at this level. 3D models helps in the evaluation of vessel anatomy and in the pre surgical planning. Post surgical image depict absence of communication between aortic and pulmonary lumen (green circle).
References: Hospital Sant Joan de Deu, Barcelona
Ductus arteriosus (PDA)
PDA is a persistent communication between the descending aorta and main or left pulmonary artery Fig. 6 Fig. 24
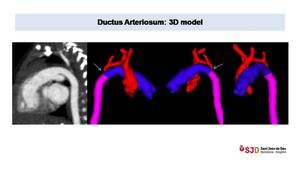
Fig. 24: Large ductus arteriosum in newborn with severe aortic coarctation. 3D models depict perfectly the aortic anatomy, the location of the severe stenosis (arrow), the presence of a large ductus connecting pulmonary artery (blue) with descending aorta (pink).
References: Hospital Sant Joan de Deu, Barcelona
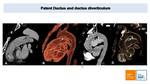
CT differentiates between PDA and Ductus diverticulum Fig. 25.
Pulmonary arteries
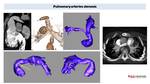
Stenosis
PA stenosis, observed in different CHD, may be key in planning surgical treatment Fig. 29. CT can evaluate pulmonary arteries course Fig. 26 or stenosis treated with intravascular stents.
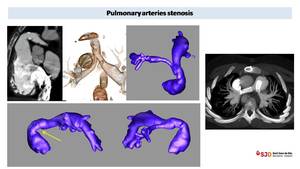
Fig. 26: PA Stenosis in 8 years old child with previous Truncus arteriosum Type II (treated in another center) and a Gore-Tex conduct connecting RV and PA. Echocardiography showed a probable stenosis. CT angiography and 3D model of pulmonary arteries confirmed a kinking (arrow) in the proximal portion of the conduct and a small right pulmonary artery with proximal stenosis. On the axial image on the right we can see good CT visualization of pulmonary artery in patient with TOF and pulmonary stenosis treated with intravascular stents
References: Hospital Sant Joan de Deu, Barcelona
Atresia
Pulmonary atresia is characterized by an atretic pulmonary valve and different degrees of anomalies of pulmonary arteries.
CT can:
- define pulmonary arteries morphology, shape and size.
- demonstrate a PDA or the presence of MAPCAs Fig. 27.
Agenesis
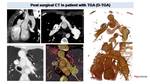
Absence of PA is a rare anomaly in which the pulmonary circulation is only supplied by MAPCAs. Fig. 28.
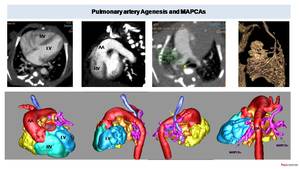
Fig. 28: Newborn with dyspnea and agenesis of pulmonary artery. Low dose (0,3 mSV) thoracic AngioCT (sedation, 6 ml of i.v. contrast and 5 ml of saline solution at 1ml/s). CT shows thoracic aorta (AA) originating from right ventricle (RV) and right aortic arch. Descending aorta (DA) is located on the right. Pulmonary arteries are absent (circle) and lung arterial supply is granted from large collateral arteries (MAPCAs) originating from the aorta and subcalvian arteries. 3D model helps to understand the complex cardiac and vascular anatomy and to visualize MAPCAS (in pink) before eventual endovascular catheterism. Even more, we can better appreciate the tracheal compression (arrows) in correspondence of the origin of the brachiocephalic trunk.
References: Hospital Sant Joan de Deu, Barcelona
MAPCAs (Major aortopulmonary collateral arteries)
MAPCAs are large collateral vessels that connect the systemic circulation to the native pulmonary arteries.
CT can assess their course and morphology and their relationship with surrounding structure Fig. 30 .
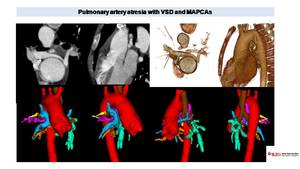
Fig. 30: CT in ten years old patient with PA with VSD. Axial image shows two small pulmonary arteries and a small main PA not communicating with RV. Ascending Aorta (AA) is dilated and originates above a VSD as an overriding aorta. VR images define better the anatomy of pulmonary arteries and the presence of MAPCAs originating from thoracic aorta. 3D model better show the anatomy and course of these collaterals (painted in pink, yellow, orange and green) and their relationship with aorta (in red), trachea (in brown) and pulmonary arteries (in blue).
References: Hospital Sant Joan de Deu, Barcelona
Pulmonary veins
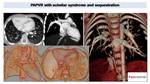
In complex anomalies of pulmonary veins, such as scimitar syndrome Fig. 31, CT can identifyl pulmonary vein connections or associated findings as pulmonary hypoplasia or sequestration.
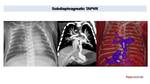
In total anomalous pulmonary return 3D images represents the best technique to define this complex venous anatomy.
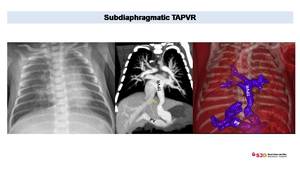
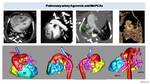
Fig. 32: TAPVR in newborn with congestive pulmonary edema. Chest x ray shows enlarges congestive hila indicative of interstitial edema. CT, with MPR and 3D model, demonstrates TAPVR into portal vein (PV). We can appreciate diaphragmatic stenois of pulmonary vein (arrow).
References: Hospital Sant Joan de Deu, Barcelona
Cardiac chambers
Tetralogy of Fallot (TOF)
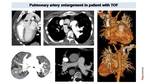
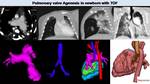
CT can depict all the anatomic features of TOF and may be useful in the analysis of pulmonary artery stenosis Fig. 33 or dilation Fig. 34.
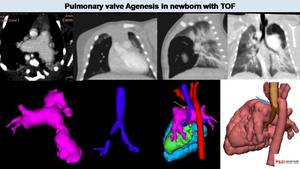
Fig. 34: Pulmonary valve agenesis in TOF. CT image shows dilated pulmonary arteries. MPR images (lung window) depict diffuse air trapping, predominant in right lung. 3D model images define the clear compression of the right main bronchi (arrows) due to severe right pulmonary artery enlargement.
References: Radiology, Hospital Sant Joan de Deu, Barcelona
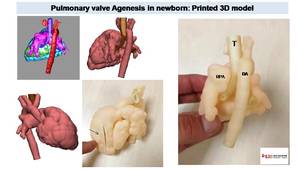
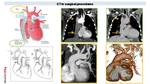
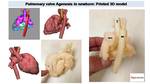
Fig. 35: 3D printed model obtained from 3D model created with CT images. We can appreciate complex cardiovascular anatomy and relationship between vessel and airways. Surgeon can observe interior ventricular cavity (by a cut realized in ventricle surface, arrow) and decide surgical treatment or decide what kind of pulmonary prosthesis is better to use.
References: Hospital Sant Joan de Deu, Barcelona
CT evaluation of associated anomalies as RAA and anomalous origin of coronary arteries can have an impact on the surgical strategy.
Double outlet ventricle (DOV)
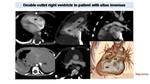
In DOV the aorta and PA arise from the same ventricle. CT allows a comprehensive evaluation of heart morphology and can differentiate DOV from a transposition of the great arteries. Fig. 36
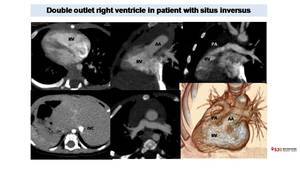
Fig. 36: CT in patient with Double outlet right ventricle (DORV). Axial images shows dextrocardia with a right apex. Abdominal images demonstrate situs inversus with liver and inferior vena cava (IVC) on the left, spleen on the right. MPR images shows how both thoracic aorta and pulmonary artery origin from right ventricular cavity. VR images better demonstrate the DORV and the spatial relationship between vessels and heart cavities.
References: Radiology, Hospital Sant Joan de Deu, Barcelona
Transposition of the great arteries (TGA)
While cardiac anatomy is better defined by echocardiography, associated anomalies can be diagnosed by CT. Even more CT helps in the evaluation of post-surgical anatomy (after Switch procedure) Fig. 37.
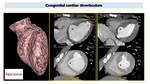
Congenital aneurysms and diverticula
Congenital aneurysm and diverticula are rare congenital outpouchings of the ventricular cavity. Cardiac MR is the best diagnostic tool, however ECG-gated CT can be useful in the diagnosis Fig. 38 .
Coronary arteries
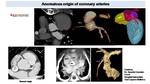
Anomalous origin
In newborns and infants, when TTE in not diagnostic, CT can be used to evaluate coronary origin and course Fig. 39 Fig. 40 .
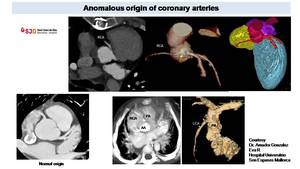
Fig. 39: Cardiac CT in patient with supraortic stenosis. CT, thanks to VR reconstructions and 3D model images, demonstrates anomalous origin of the right coronary artery (RCA) from left sinus with an intramural course (yellow arrow). With CT is possible to detect anomalous origin from pulmonary artery as in the images on the right (Courtesy Dr. Amador Gonzalez Eva R Hospital Universitrio Son Espases Mallorca)
, with an origin of the left coronary artery (LCA) from the pulmonary artery (PA) defined ALCAPA
References: Hospital Sant Joan de Deu, Barcelona and Hospital Universitrio Son Espases, Mallorca
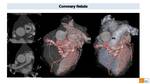
Ectasias
It is is generally associated with Kawasaki disease. CT demonstrates coronary aneurisms avoiding repeated invasive angiography.
Fistulas
Large coronary fistulas may represent a CT indication. If untreated or asympthomatic we can diagnose this anomaly later Fig. 41.
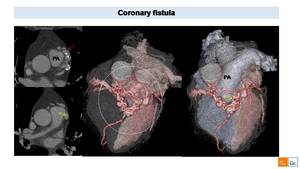
Fig. 41: Cardiac CT in adult patient with coronary fistula. Axial images shows an enlarged left coronary artery that continues with a tortuous vascular structure characterized by multiple dilations and calcified walls. This anomalous vascular structure drains (yellow arrow) into pulmonary artery (PA) representing a coronary fistula to PA. VR images better shows the complex anatomy of the coronary fistula (white circle) and its relationship with surrounding structures.
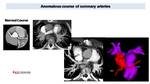
In all patients with CHD coronary artery origin, diameter and course should be evaluate becsuse these anomalies can modify the patient management.
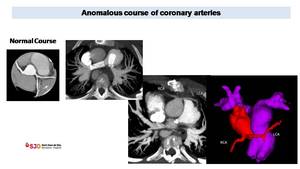
Fig. 40: Anomalous origin and course of LCA in patient with TOF. CT was realized without ECG gating to study pulmonary arteries stenosis, treated with vascular stents. Even if contrast enhancement of coronary artery is not ideal, we can appreciate an anomalous origin of LCA from an anterior right ostium. We can also appreciate (better on 3D models) LCA course, anterior to pulmonary artery in violet), important to determine before possible new surgical treatment, to avoid iatrogenic lesions.
References: Radiology, Hospital Sant Joan de Deu, Barcelona
Cardiac valves
Bicuspid aortic valve (BAV)
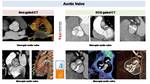
BAV is the most common CHD and may lead to aortic stenosis or regurgitation. When BAV is extremely calcified CT can be used Fig. 42.
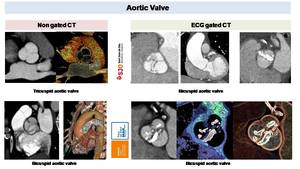
Fig. 42: CT can define BAV morphology both in non gated than in gated ECG CT scan. It’s especially useful when BAV is calcified and MRI or Echocardiography are limited.
CT can evaluate associated aortic arch anomalies Fig. 43.
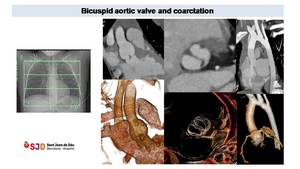
Fig. 43: Seven years old patient with bicuspid aortic valve and aortic coarctation surgically repaired. Prospectively gated CT was realized from supraortic arteries to diaphragm to define aortic arch morphology after surgery at evaluate ascending aorta and aortic valve at the same time.
References: Radiology, Hospital Sant Joan de Deu, Barcelona
Truncal valve
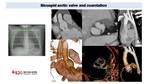
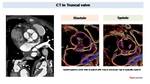
Truncus arteriosum is characterized by a single arterial trunk with a single truncal valve typically dysplastic with thickened cusps and supernumerary leaflets than can be assessed by CT Fig. 44.
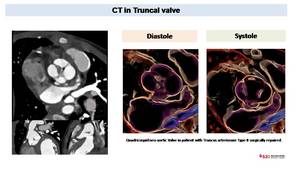
Fig. 44: Retrospectively gated cardiac CT in infant with truncus arteriosum Type II surgically repaired. CT shows a quadricuspid valve that now it is connected to the new aorta (previously to surgery was the truncal valve). MPR images and Diastolic and systolic VR reconstruction shows thickened leaflets with good opening but incomplete closure.
References: Radiology, Hospital Sant Joan de Deu, Barcelona
Pulmonary valve agenesis
Pulmonary valve agenesis is a rare malformation characterized by a total or partial absence of the pulmonary valve leaflets Fig. 34
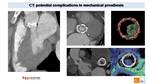
Mechanical prosthesis
Mechanical prosthesis can be easily evaluated by CT.
With retrospectively gated CT, acquired without e.v. contrast, we can analyze leaflets movements and angles to define a good function Fig. 45.
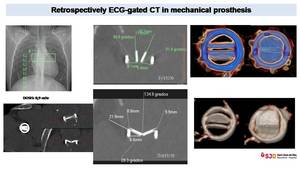
Fig. 45: CT in mechanical prosthesis. Retrospectively ECG-gated CT realized without i.v. contrast only focused on the prosthesis allows to define leaflets movements and calculate the angle between the prosthetic ring and the leaflets in diastole or in systole to define a good function. VR reconstructions better define prosthesis morphology at any time of cardiac cycle.
References: Radiology, Hospital Sant Joan de Deu, Barcelona
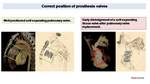
CT and 3D images are key to determine correct prosthesis positioning Fig. 46.
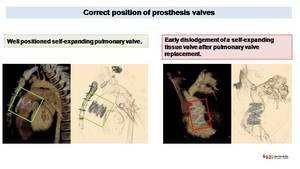
Fig. 46: CT evaluation of correct and incorrect prosthesis position. VR images easily depict a correct positioning into pulmonary valve of a self-expanding pulmonary valve (images on the left). We can easily define an incorrect position due to early displacement of a self-expanding pulmonary valve on the right, where the prosthetic pulmonary valve is displaced into the right ventricular outflow tract, parallel to pulmonary artery long axis and its diameter is enlarged (43 mm vs the normal value of 32 mm)
References: Radiology, Hospital Sant Joan de Deu, Barcelona
When we suspect complication as pannus, thrombi or paravalvular leaks, the use of i.v contrast in necessary Fig. 47.
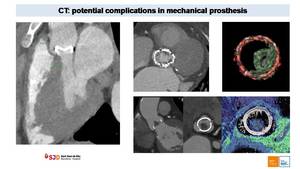
Fig. 47: Potential complications of mechanical prosthesis. Paravalvular leak (image on the left) and thrombus (other images) can be detected with ECG-gated CT scan with i.v contrast.
References: Radiology, Hospital Sant Joan de Deu, Barcelona and Radiology Hospital del Mar
Systemic Veins
Persistent left superior vena cava (PLSVC) and double superior vena cava
The PLSVC usually drains into the right atrium through a dilated coronary sinus. In a minority of patient PLSVC drains into the left atrium Fig. 48 generating right-to-left cardiac shunt.
CT easily defines the presence of PLSVC as its drainage, key in the management of these patients.
When PLSVC is accompanied by a normal right-side vena cava we have a double superior vena cava, where right vena cava drains into the right atrium.